Discovering a dark spot or an unusual breakout inside your mouth can be a cause for concern. While many of these occurrences are benign, understanding their potential causes and appropriate treatments is crucial for maintaining oral health. This guide delves into the various reasons for dark spots and breakouts within the oral cavity, ranging from harmless pigmentation to more serious conditions, and outlines when to seek professional medical advice.
Causes of Dark Spots Inside the Mouth
Dark spots within the mouth can manifest due to a variety of factors, some of which are entirely harmless, while others warrant medical attention.
Amalgam Tattoos
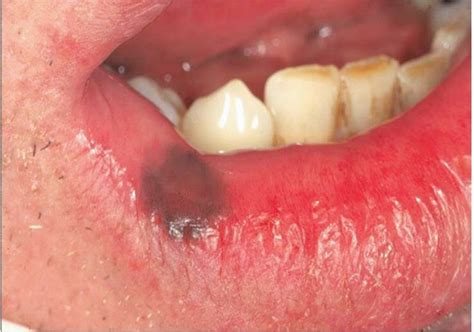
If the spot inside your cheek is dark blue, gray, or black, it could be a leakage from a dental filling. Amalgam tattoos are not permanent ink decorations but rather the result of particles from amalgam fillings, a silvery substance dentists use to fill cavities, made from a mixture of tin, zinc, mercury, copper, and silver. These tattoos are permanent but do not cause any harm. If the mark is inside your cheek, it's unlikely anyone will see it.
Smoker's Melanosis
Smoking can leave dark stains inside the cheeks and other areas of the mouth, such as on the gums. This condition is called smoker's melanosis, and approximately 22 percent of smokers may notice this kind of discoloration in their mouths. While these stains do not require treatment, they are a visible sign of the damage smoking can inflict on oral tissues. A biopsy may be recommended to rule out other conditions, and laser treatment or electrosurgery can be used for removal if desired.
Benign Pigmented Lesions
The inner lining of your cheek may simply be patchily pigmented. You could have a benign melanotic macule, which is a spot similar to a freckle that can appear in the oral cavity. These are flat, noncancerous areas of hyperpigmentation. Another benign condition is oral melanoacanthoma, a rare, harmless spot that can grow quickly and may look like an ulcer. These spots usually do not require treatment unless they cause discomfort or cosmetic concern.
Oral Nevi (Moles)
Oral nevi are small, slightly raised spots that can form inside the mouth, appearing brown, bluish-gray, or nearly black. While typically harmless and asymptomatic, they can occur on the roof of the mouth, inner lip, or cheek. Though generally not cancerous, a doctor or dentist might recommend a biopsy to confirm the diagnosis and rule out melanoma.
Blood Blisters
Blood blisters are sacs of fluid that fill with blood, appearing dark red or purple. They can develop in the mouth due to accidentally biting the cheek, minor trauma, or as a result of an allergic reaction. These blisters are often painful when touched. While most blood blisters heal on their own within a couple of weeks, persistent or recurring ones should be evaluated by a doctor.
Genetic and Systemic Conditions
Certain genetic disorders can also cause dark spots inside the mouth:
- Peutz-Jeghers Syndrome: This rare inherited disorder causes dark freckles around the face and inside the mouth, as well as noncancerous growths (polyps) in the gastrointestinal tract. The spots usually fade with age, but the polyps may require surgical removal.
- Addison's Disease: This endocrine disorder, also known as adrenal insufficiency, occurs when the adrenal glands do not produce enough hormones. A symptom can be hyperpigmented blotches of skin inside the mouth, along with fatigue, weight loss, and salt cravings. Treatment involves hormone replacement medication.
Medication-Induced Oral Pigmentation
Certain medications can cause unexpected changes in oral pigmentation, leading to the appearance of black spots inside the cheek. Distinguishing this from other causes can be challenging, and consulting a healthcare professional is essential for accurate diagnosis and management.
Oral Cancer
Very rarely, a black or dark spot on the inside of the cheek could be a sign of oral malignant melanoma or another type of oral cancer. Oral melanoma is a rare but serious condition that affects pigmented cells. Symptoms can include white, gray, or bright red sores or bumps that are oddly shaped, may bleed, and don't heal. It can appear anywhere inside the mouth. Early detection is crucial for successful treatment, which often involves surgery, immunotherapy, or radiation therapy.
Causes of Breakouts Around the Mouth (Perioral Acne)
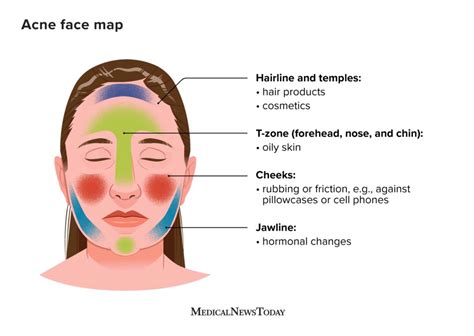
Breakouts around the mouth, often referred to as perioral acne, can be stubborn and frustrating. These typically involve pimples, red bumps, or clusters of irritation forming around the lips, chin, and jawline. Unlike occasional pimples, perioral acne tends to recur and can be influenced by various internal and external factors.
Hormonal Fluctuations
Hormonal shifts, such as those occurring during puberty, menstrual cycles, pregnancy, or periods of stress, can cause oil glands to become overactive, leading to breakouts in the mouth and chin areas.
Cosmetics and Skincare Products
Heavy makeup, pore-clogging lip balms, or certain sunscreens applied near the mouth can contribute to clogged pores and irritation, resulting in acne in this region.
Lifestyle Habits
Frequent touching of the face, using unwashed masks, or wearing sports gear like chin straps can trap sweat and bacteria, exacerbating breakouts.
Dental and Oral Care Products
Toothpastes or mouthwashes containing fluoride or harsh ingredients may irritate the sensitive skin around the lips, leading to pimples.
Perioral Dermatitis
Sometimes mistaken for acne, perioral dermatitis is an inflammatory condition that causes clusters of small red bumps around the mouth and nose. A dermatologist can distinguish between true acne and this condition.
Diet
For some individuals, certain dietary choices can influence acne flare-ups. Research suggests that high-glycemic foods (like white bread, sugary drinks, and processed snacks) and dairy may increase the likelihood of pimples forming along the jawline and chin. Keeping a food diary can help identify personal triggers.
When to Seek Professional Medical Advice
While many dark spots and breakouts inside the mouth are harmless, it is always advisable to consult a dentist or doctor if you notice any of the following:
- An abnormal spot that doesn't go away after a couple of weeks.
- A spot that bleeds or grows larger.
- Increased swelling, changes in skin texture, or color of the lesion.
- Pain associated with the spot or breakout.
- If you have a history of oral cancer and notice a recurrence.
- Persistent or worsening breakouts around the mouth that do not respond to home care.
A healthcare professional can perform a visual inspection, ask about your medical history, and may recommend further tests, such as a biopsy or blood tests, to make an accurate diagnosis and determine the appropriate course of treatment.
Treatment and Prevention Strategies
Treatment and prevention strategies vary depending on the underlying cause.
For Dark Spots:
- Amalgam Tattoos, Smoker's Melanosis, Benign Lesions: These typically do not require treatment. However, if a spot is a cosmetic concern, options like laser therapy may be available. For smoker's melanosis, quitting smoking is the most effective lifestyle change.
- Oral Nevi: Usually no treatment is needed, but a biopsy may be performed for confirmation.
- Blood Blisters: Most resolve on their own. Over-the-counter pain relief can manage discomfort.
- Genetic/Systemic Conditions (Peutz-Jeghers, Addison's): Management focuses on treating the underlying condition, which may include surgical removal of polyps or hormone replacement therapy.
- Oral Cancer: Treatment is critical and may involve surgery, radiation, or chemotherapy. Early detection significantly improves outcomes.
For Breakouts Around the Mouth (Perioral Acne):
- Skincare Routine: Use a gentle, non-comedogenic cleanser twice daily. Avoid over-washing.
- Targeted Treatments: Over-the-counter options like benzoyl peroxide or salicylic acid can help. Prescription retinoids are effective at preventing new breakouts.
- Product Review: Switch to non-comedogenic lip balms and makeup. Consider fluoride-free or less harsh toothpaste and mouthwash if irritation is suspected.
- Lifestyle Adjustments: Keep hands away from the face, clean makeup brushes regularly, change pillowcases and face masks frequently, maintain a balanced diet, stay hydrated, and manage stress.
- Professional Care: If breakouts persist, a dermatologist can prescribe topical or oral medications and recommend in-office treatments.

Maintaining good oral hygiene, including brushing twice a day and flossing once a day, along with regularly checking the inside of your mouth for any changes, can help reduce concerns and ensure early detection of any potential issues.