Cystic acne is a severe and often painful form of inflammatory acne characterized by deep, pus-filled nodules that form when bacteria, oil, and dead skin cells become trapped beneath the skin's surface. Unlike milder forms of acne, over-the-counter topical treatments often lack the ability to penetrate deeply enough to effectively treat these lesions. This aggressive type of acne can persist for weeks and, if left untreated or improperly managed, carries a significant risk of causing permanent scarring.
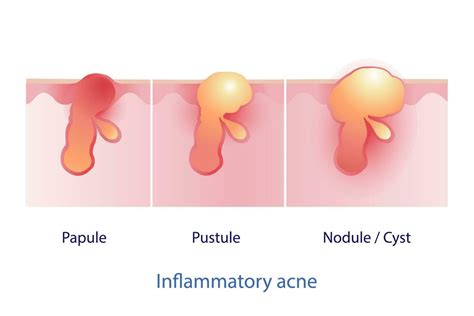
Understanding Cystic Acne
The formation of cystic acne occurs when pores become blocked. This blockage can be caused by the skin's natural oil, bacteria, and dead skin cells. Once a pore is clogged, inflammation and swelling can develop. In some cases, bacteria may colonize the blocked pore, leading to the characteristic deep, painful cysts.
Causes and Triggers
Several factors can contribute to the development of cystic acne:
- Hormonal Fluctuations: Hormonal imbalances, such as those experienced during puberty, pregnancy, or menopause, can trigger cystic acne. In women, an excess of androgens (hormones present in both sexes) can stimulate the glands in hair follicles to produce more oil, leading to clogged pores. This type of hormonal acne often appears on the lower face, including the jawline.
- Genetics: Some individuals may be genetically predisposed to developing acne, including cystic acne.
- Stress: Stress can increase cortisol levels, which in turn can exacerbate inflammation and contribute to acne development.
- Medications: Certain medications, including oral contraceptives, steroids, and lithium, can sometimes trigger or worsen acne.
- Diet: Some people find that certain foods, particularly those with a high glycemic index (GI) and dairy products, can aggravate their acne. Refined carbohydrates, which convert to glucose in the body, are often cited as contributors to inflammation.
- Skin Microbiome: Imbalances in the skin's microbiome, including the presence of certain bacteria, can also play a role in causing inflammation associated with acne.

Treatment Approaches for Cystic Acne
Cystic acne typically requires professional medical intervention due to its severity and depth. Dermatologists offer a range of treatments designed to reduce inflammation, combat bacteria, and prevent scarring.
Prescription Medications
Dermatologists often employ a combination of topical and oral medications to manage cystic acne:
- Oral Antibiotics: Low-dose oral antibiotics, such as doxycycline or minocycline, are frequently prescribed as a first-line treatment. These medications primarily target inflammation rather than infection directly, helping to calm the inflammatory response associated with cystic acne.
- Topical Treatments: While over-the-counter options may not be sufficient, prescription-strength topical treatments can be effective.
- Azelaic Acid 15%: This naturally occurring acid possesses antibacterial and anti-inflammatory properties. It also helps to slow down the production of keratin, a substance that can cause dead skin cells to stick together and clog pores. Additionally, azelaic acid can help reduce post-inflammatory hyperpigmentation (dark spots left after acne heals).
- Topical Antibiotics: These can kill acne-causing bacteria and help prevent new pimples from forming.
- Benzoyl Peroxide: This ingredient is effective at killing bacteria and preventing pores from becoming blocked.
- Retinoids: Topical retinoids, including retinol, tretinoin, and adapalene, are vitamin A derivatives that are a common component of acne treatment. They help to unclog pores and promote skin cell turnover. Dermatologists may recommend using topical retinoids in conjunction with topical antibiotics or benzoyl peroxide.
- Isotretinoin: For severe or persistent cystic acne, a potent oral retinoid medication like isotretinoin (formerly known as Accutane) may be recommended. This medication is highly effective, with a significant percentage of patients experiencing long-term clearing after a single course of treatment. However, isotretinoin can cause significant side effects, including birth defects, so it is not suitable for pregnant women or those planning to become pregnant. Other potential side effects include joint pain and dryness of the skin and lips, which can often be managed with over-the-counter pain medication and moisturizers like Aquaphor. Isotretinoin is usually considered after other treatments have failed, but may be discussed earlier if scarring is present at the initial consultation.
- Spironolactone: This medication is particularly useful for women experiencing hormonal cystic acne, especially along the jawline. It works by blocking androgen hormones that stimulate oil production.
- Oral Contraceptives: For females, certain contraceptive pills containing estrogen can help improve cystic acne by regulating hormone levels. Sometimes, this is combined with spironolactone.
Pharmacology - ACNE TREATMENTS (MADE EASY)
In-Office Procedures
In addition to medications, dermatologists can perform procedures to address acute cystic acne:
- Corticosteroid Injections: For individual, inflamed cystic lesions, a dermatologist may inject a corticosteroid medication directly into the cyst. This can rapidly reduce inflammation, pain, and swelling, helping to speed up healing and minimize the risk of scarring.
- Light and Laser Therapies: Certain light and laser treatments can help reduce acne-causing bacteria and calm inflammation on the skin.
Home Care and Lifestyle Adjustments
While professional treatment is crucial for cystic acne, certain home care practices and lifestyle changes can support skin health and potentially reduce flare-ups:
Skincare Routine
- Gentle Cleansing: Wash your face up to twice daily and after sweating. Use a gentle, non-abrasive cleanser that is alcohol-free.
- Exfoliation: While avoiding harsh exfoliants, consider using an exfoliating cleanser containing ingredients like glycolic acid or sulfur to help remove dead skin cells from the surface. Use such a cleanser both in the morning and at night. Some sources suggest avoiding products with salicylic acid for cystic acne.
- Moisturizing: Keeping the skin hydrated is important, especially if using drying acne treatments.
- Sun Protection: Many acne treatments increase sensitivity to UV light, and sun exposure can worsen acne. It is essential to wear facial sunscreen daily.
- Avoid Picking or Popping: It is critical not to pop, pick, or squeeze cystic pimples. Doing so can push inflammation deeper into the skin, significantly increasing the risk of infection and permanent scarring.
- Avoid Unproven Home Remedies: Many online home remedies for acne are not based on strong evidence and may be ineffective or even harmful. It is best to rely on advice from trusted sources or a board-certified dermatologist.

Lifestyle Modifications
- Dietary Changes: Consider reducing your intake of refined carbohydrates and potentially dairy products if you notice they aggravate your acne.
- Stress Management: Incorporate stress-reducing activities into your routine, such as mindfulness, yoga, or meditation.
- Regular Exercise: Physical activity can help decrease stress levels.
- Adequate Sleep: Ensure you are getting enough restful sleep, as this is crucial for overall health and skin recovery.
When to See a Dermatologist
If you are struggling with cystic acne, especially if it is painful, persistent, or leaving scars, it is highly recommended to consult a dermatologist. They can accurately diagnose your condition, discuss appropriate treatment options, and help prevent further complications.
A cystic pimple can last for several weeks, and while some mild cysts may eventually improve on their own, many do not fully resolve without professional treatment. With the right dermatologic care, inflammation usually improves within a few weeks, although complete clearing may take several months depending on the severity of the acne.
Preventing and Managing Scarring
Cystic acne has a much higher risk of scarring compared to other types of acne, particularly if the acne is severe, long-lasting, or picked at. After successful acne treatment, a dermatologist can discuss options to reduce the appearance of scarring. These may include:
- Microneedling or Dermarolling: These procedures use tiny needles to stimulate collagen production.
- Chemical Exfoliants and Peels: These treatments remove damaged skin cells to allow new ones to grow.
- Laser Resurfacing: This can help make scars flatter and less noticeable.
- Incision or Subcision: In some cases, scars may be physically removed.