Acne is a prevalent skin condition that affects a significant portion of the population, particularly between the ages of 11 and 30. It arises when bacteria, oils, and dead skin cells accumulate and inflame pores, the small openings in the skin responsible for releasing oil and sweat. While dead skin cells naturally shed, sometimes they can clog pores, leading to various forms of acne. Hormonal fluctuations, especially during teenage years, are a primary driver, but adults may also experience acne due to stress, environmental factors, menstrual cycles, oil-based cosmetic products, and oral contraceptives.
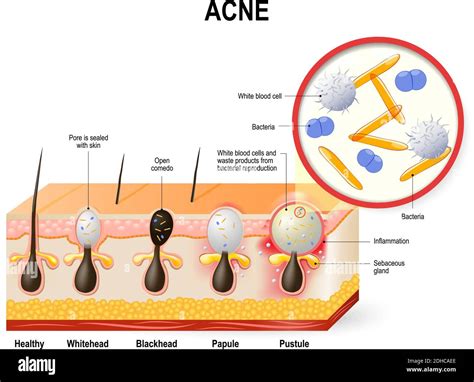
Types of Acne and Their Appearance
Acne manifests in several forms, ranging from mild to severe. Whiteheads and blackheads are common and often heal without significant scarring. However, certain types of acne lesions can lead to more persistent marks:
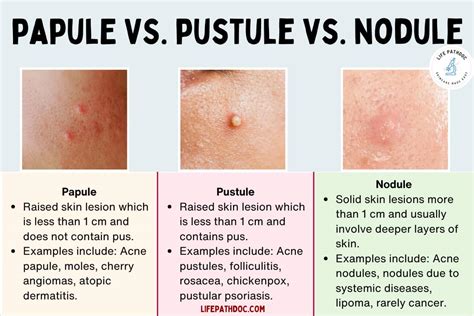
- Papules: These are small, pink to red bumps that can be tender to the touch.
- Pustules: Characterized by pus-filled lesions, they typically have a red base and a white or yellow top.
- Nodules: These are larger, solid lesions that extend deeper into the skin, often causing more pain.
- Cysts: Located deep within the skin, cysts are painful, pus-filled, and have the highest likelihood of causing scars.
The Process of Acne Scar Formation
Acne scars are a consequence of the inflammation that occurs during an acne breakout. When an acne pore swells, the wall of the pore can break down. Small blemishes might result in shallow scars that heal quickly. However, if the contents of a blemish spill into surrounding tissues, deeper scars can form. The skin's natural healing response involves creating new collagen fibers to repair the damaged area.
Acne scars generally fall into two main categories:
- Atrophic (depressed) scars: These result from a loss of tissue, creating indentations in the skin's surface.
- Hypertrophic (raised) scars: These occur when the skin produces an excessive amount of collagen during the healing process, leading to a raised scar tissue formation. This is the skin's way of over-repairing the wound.
It's important to note that not everyone with acne will develop scars. Approximately one in five individuals with acne will experience scarring. Fortunately, many acne scars are not permanent, and various treatments can help minimize their appearance or encourage the skin's natural healing processes.
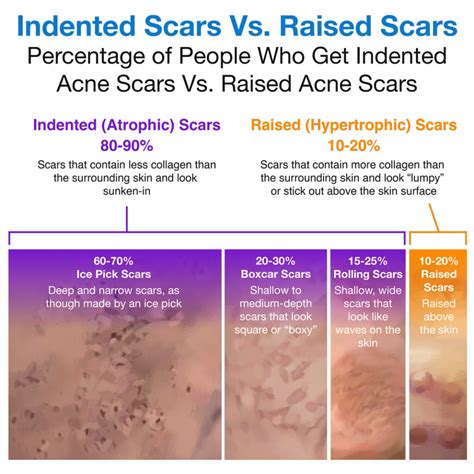
Types of Acne Scars and Their Characteristics
Individuals with acne scarring often present with a combination of scar types. The following are the most common:
Atrophic or Depressed Scarring
- Ice pick scars: These are narrow, deep scars that resemble puncture wounds, wide at the surface and tapering to a point as they go deeper. They are frequently found on the forehead and upper cheeks, areas where the skin is thinner, and can be challenging to treat.
- Rolling scars: Typically appearing on the lower cheeks and jawline where the skin is thicker, these scars have sloping edges that give the skin an uneven, wavy appearance.
- Boxcar scars: Characterized by sharp, well-defined edges, these indentations extend deep into the skin. They are also common on the lower cheeks and jaw.
Hypertrophic or Keloid Scars
These scars are raised above the skin's surface and result from an overproduction of fibrous tissue (collagen) during healing. Hypertrophic and keloid scars are often found on the chest, back, shoulders, and jawline and can be itchy, tender, or painful.
The Prevalence of Acne Scarring
Acne scarring is very common, affecting a significant portion of those who experience acne. With approximately 80% of individuals aged 11 to 30 having acne, and one in five of this group developing scars, it highlights the widespread impact of this condition.
Understanding Papules and Their Role in Scarring
Papules are a common type of inflammatory acne, appearing as small red bumps on the face. They occur when excess sebum (skin's natural oil) and dead skin cells clog a pore. The inflammation that defines a papule arises when bacteria contribute to the inflammatory process, leading to these characteristic red bumps.
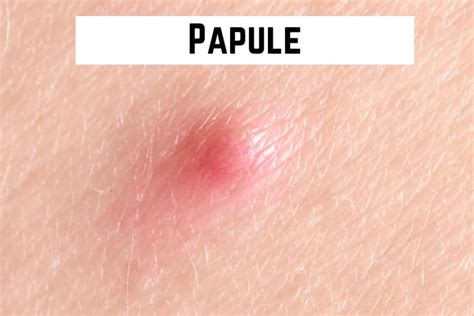
Identifying a Papule
A papule typically presents as a red or pink bump that may feel firm to the touch and can be tender. Unlike pustules, papules are not filled with pus.
Contributing Factors to Papules
The formation of papules is influenced by several factors:
- Excess Sebum Production: Overactive sebaceous glands produce more oil than necessary, creating an environment conducive to acne.
- Buildup of Dead Skin Cells (Hyperkeratinization): When dead skin cells don't shed properly, they accumulate within the pore.
- Bacteria: Propionibacterium acnes (P. acnes) bacteria thrive in clogged pores, feeding on sebum and triggering an inflammatory response.
- Hormones: Fluctuating hormone levels can exacerbate oil production and contribute to acne breakouts, including papules.
- Stress: Stress is known to worsen acne conditions.
- Genetics: Predisposition to acne can be inherited.
Papules vs. Nodules
While papules are small, inflamed bumps, nodules are a more severe form of inflammatory acne. Nodules develop deeper within the skin, are typically larger and more painful than papules, and carry a higher risk of scarring. Unlike papules, nodules are not pus-filled.
Treatments for Acne Papules
Fortunately, papules are treatable, with various options available depending on the severity of the acne. A combination of treatments may be most effective.
Over-the-Counter (OTC) Treatments
- Benzoyl Peroxide: This ingredient effectively fights acne-causing bacteria and reduces inflammation.
- Salicylic Acid: As a beta-hydroxy acid (BHA), salicylic acid helps to exfoliate the skin and unclog pores.
- Retinoids: Available OTC (e.g., adapalene) and by prescription (e.g., tretinoin), retinoids help prevent clogged pores and treat existing papules.
Prescription Treatments
- Topical Antibiotics: Medications like clindamycin and erythromycin can reduce inflammatory lesions.
- Oral Contraceptives: For women, hormonal birth control pills can help regulate hormones that contribute to acne.
- Oral Antibiotics: Prescribed for persistent acne, antibiotics like doxycycline or minocycline help combat bacteria.
- Isotretinoin: A potent form of vitamin A, often used for severe or persistent acne, it significantly reduces sebum production and inflammation.
- Anti-androgens: These medications block the effects of hormones that can worsen acne.
- Dapsone: A topical gel with antibacterial properties.
Consulting a healthcare professional is crucial to determine the most suitable treatment plan, as individual responses can vary.
Preventing Papules
Preventive measures can significantly reduce the occurrence of papules:
- Regular Facial Cleansing: Using cleansers with ingredients like salicylic acid or benzoyl peroxide can help keep pores clear.
- Use Non-Comedogenic Products: Opt for skincare and makeup products formulated not to clog pores.
- Remove Makeup Daily: Thoroughly removing makeup before bed prevents pore blockage.
- Be Patient: Acne treatments often take several weeks (six to eight) to show noticeable improvement.
Acne: Understanding the Types of Acne and Treatment Options
The Importance of Not Popping Papules
It is strongly advised not to pop or pick at papules. Doing so can:
- Introduce bacteria, leading to infection.
- Cause further inflammation and irritation.
- Push oil, bacteria, and dead skin cells deeper into the skin.
- Result in acne scars, which are more challenging to treat than the original blemish.
Since papules do not contain pus, attempting to pop them is particularly counterproductive and increases the risk of complications.
Do Papules Go Away on Their Own?
Most papules will resolve on their own within three to seven days, though some may take several weeks to disappear completely.
Managing Acne Papules
Effective management of acne papules involves understanding the specific type of acne and choosing appropriate treatments. Knowing whether you have inflammatory acne (papules, pustules, nodules, cysts) or noninflammatory acne (blackheads, whiteheads) is the first step.
When a clogged pore ruptures and disperses bacteria into the skin tissue, the body's inflammatory response creates a papule. The primary causes include bacteria, excess oil production, and hormonal influences. Stress, diet, and certain medications can also aggravate acne.
For persistent or severe cases, a dermatologist may recommend prescription treatments such as topical dapsone, retinoids, antibiotics (topical or oral), birth control pills, or anti-androgen agents.
It's important to distinguish papules from nodules. Nodules are more severe, deeper, and more likely to scar. If you suspect nodular acne, seeking professional dermatological advice is recommended.
Papules are small, raised bumps that lack visible pus initially but often develop into pustules. They are a symptom of inflammatory acne and can be treated with both OTC and prescription medications. While home remedies like apple cider vinegar, green tea, honey, ice, lemon juice, and tea tree oil may offer some benefits, it's advisable to consult a healthcare provider before using them, especially if you have sensitive skin.