While most blood transfusions proceed without complications, some individuals may experience adverse reactions during or after the procedure. These reactions can range in severity from mild to severe and can manifest in various ways, including fever, chills, itching, or difficulty breathing. Understanding the potential causes, recognizing the symptoms, and knowing the appropriate management strategies are crucial for ensuring patient safety.
Types of Transfusion Reactions
Transfusion reactions are broadly categorized into acute and delayed reactions, each with distinct causes and clinical presentations.
Acute Transfusion Reactions
Acute reactions occur during or within 24 hours of a blood transfusion. They can be immunologic or non-immunologic in nature.
Simple Allergic Reaction
Simple allergic reactions, also known as mild allergic reactions, are among the most common transfusion reactions. They occur when the recipient's blood reacts to specific plasma proteins or other allergens present in the donor blood. Symptoms are typically mild and can include:
- Rash
- Itching
- Hives
Treatment for a mild allergic reaction usually involves stopping the transfusion and administering an antihistamine to alleviate the symptoms.
Anaphylactic Transfusion Reaction
Anaphylactic reactions are more severe and occur primarily in individuals with immunoglobulin A (IgA) deficiencies who have developed IgA antibodies. These antibodies can react with the IgA in the donor blood, triggering a serious systemic response. Symptoms can include:
- Flushed skin
- Itching
- Hives
- Swelling
- Difficulty breathing
- Wheezing
- Blue lips
- Vomiting
- Diarrhea
- Low blood pressure
Immediate cessation of the transfusion is necessary. Management involves addressing the specific symptoms with interventions such as intravenous (IV) epinephrine, IV steroids, antihistamines, and bronchodilators.
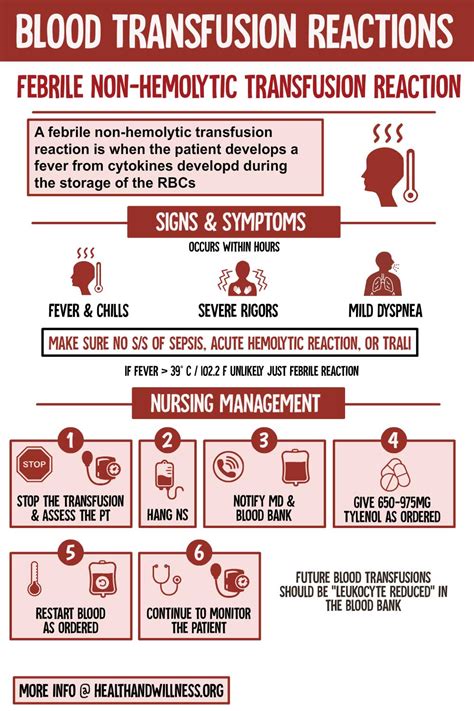
Febrile Non-Hemolytic Transfusion Reaction (FNHTR)
FNHTR is the most common type of transfusion reaction, characterized by an unexplained rise in temperature during or within 4 hours after the transfusion. This fever is often a response of the recipient's white blood cells to the transfused blood. Symptoms may include:
- Fever (temperature higher than 38ºC or 100.4ºF)
- Chills
If other symptoms are present, contacting a doctor is advised. If FNHTR occurs during the transfusion, the procedure is stopped. Treatment depends on the symptoms, but most reactions are mild and respond quickly. It is important to investigate all cases of fever as it can indicate a more severe underlying cause. Treatment may involve taking aspirin or acetaminophen.
Acute Hemolytic Transfusion Reaction (AHTR)
AHTR is a serious reaction that occurs if a patient receives the wrong blood type. The body begins to destroy the donated red blood cells. Symptoms can manifest during, immediately after, or within 24 hours of the transfusion and may include:
- Chills
- Low blood pressure
- Renal failure
- Back pain
- Flank pain
- Fever
- Red or brown urine
Upon suspicion of AHTR, the transfusion is stopped. Treatment depends on the severity and may involve IV fluids, dialysis, management of bleeding, and supportive care.
Septic Transfusion Reactions
These reactions typically result from bacterial contamination of the donor blood components, most commonly platelet products. Bacteria such as Staphylococcus aureus and Staphylococcus epidermidis can cause septic reactions. Symptoms include:
- Fever
- Chills
- Low blood pressure
Septic transfusion reactions require immediate medical attention. Management involves fluid management, respiratory support, and antibiotic therapy.
Transfusion-Related Acute Lung Injury (TRALI)
TRALI is a rapid-onset reaction caused by antibodies in the donor blood (e.g., human leukocyte antibodies) reacting with the recipient’s white blood cells, leading to pulmonary edema (fluid in the lungs). There is no specific test to identify blood products that will cause TRALI. Symptoms include:
- Severe shortness of breath
- Fever
- Low blood pressure
Treatment depends on severity, ranging from oxygen therapy for mild cases to artificial ventilation for more severe cases. While most cases resolve within 48-72 hours, TRALI can be fatal, with a mortality rate of 5-25%.
Transfusion-related Acute Lung Injury (TRALI): Warning Signs and How to Avoid It.
Transfusion-Associated Circulatory Overload (TACO)
TACO occurs when the circulatory system cannot process the volume or speed of the transfused blood, leading to volume overload and pulmonary edema. Individuals with heart or kidney conditions are at higher risk. Symptoms typically appear during or within a few hours of the transfusion and include:
- Rapid breathing
- Coughing
- Shortness of breath
- High blood pressure
- Rapid heartbeat
If symptoms arise during transfusion, the procedure is stopped immediately. Treatment depends on severity, with mild cases managed by positioning the patient upright, more advanced cases treated with diuretics, and severe cases requiring intubation for respiration support.
Delayed Transfusion Reactions
Delayed reactions occur days to weeks after a transfusion.
Delayed Hemolytic or Delayed Serologic Transfusion Reaction
This reaction occurs when a pre-existing antibody in the recipient reforms and reacts with red blood cell antigens. Reactions can occur between 1 day and 4 weeks post-transfusion. Antibodies are often acquired through previous pregnancies or transfusions and may decrease over time to undetectable levels. Symptoms typically include:
- Fever
- Jaundice
- Abdominal pain
- Dark urine
- High blood pressure
- Labored breathing
These reactions tend to be mild and may not require treatment. Hydration is important if the reaction is significant.
Transfusion-Associated Graft-Versus-Host Disease (TAGVHD)
TAGVHD is a very rare but severe complication where donor T-lymphocytes multiply in the recipient and attack the recipient's cells. It is less prevalent since the introduction of blood product irradiation. Symptoms include:
- Rash
- Nausea
- Vomiting
- Diarrhea
- Abdominal pain
- Fever
- Bone marrow failure
TAGVHD is challenging to treat, with mortality rates between 90-100%. Prevention through blood irradiation is the most effective strategy.
Posttransfusion Purpura (PTP)
PTP is a rare condition where the recipient develops antibodies against platelets, leading to their destruction and a drop in platelet count. Symptoms can include:
- Bleeding of the gastrointestinal tract and urinary tract
- Fever and chills
Treatment may involve supportive care, IV immunoglobulins, and steroids.
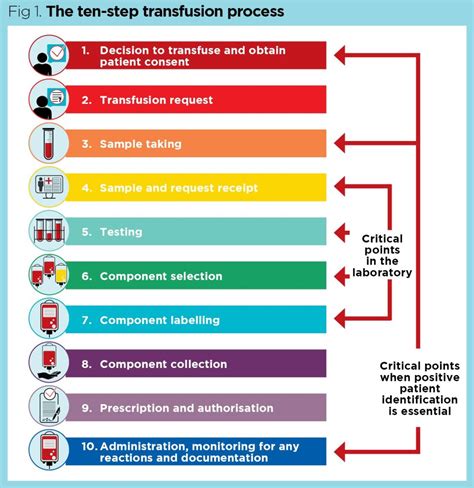
Diagnosis and Management
The diagnosis of a transfusion reaction begins with recognizing signs and symptoms. A critical first step is to immediately stop the transfusion and maintain an open IV line with saline. A clerical check is essential to ensure the correct patient received the correct blood product. Monitoring vital signs at regular intervals is crucial. A post-transfusion blood sample should be collected for laboratory testing, and the blood bag and tubing should be sent to the blood bank for further investigation.
Treatment for specific transfusion reactions is often supportive. For mild allergic reactions, antihistamines like diphenhydramine are effective. For febrile non-hemolytic reactions, antipyretics may be administered. In more severe cases, interventions are tailored to the specific reaction and may include fluid resuscitation, respiratory support, or specific medications.
Prevention and Outlook
While some reactions are unavoidable due to the unique nature of donor-recipient interactions, many can be prevented or mitigated through careful patient selection, proper crossmatching, and vigilant monitoring during and after transfusions. Understanding the risk factors associated with each type of reaction allows healthcare providers to take appropriate precautions.
The outlook for patients experiencing transfusion reactions varies greatly depending on the type and severity of the reaction. Mild reactions like simple allergic responses often resolve quickly with minimal or no treatment. However, severe reactions such as acute hemolytic transfusion reactions, TRALI, and TAGVHD can have significant morbidity and mortality. Continuous improvement in blood screening, component processing, and clinical monitoring practices aims to further enhance transfusion safety.
tags: #rash #after #blood #transfusion