Ringworm, also known medically as tinea, is a common fungal infection that affects the skin, nails, and scalp. Despite its name, it is not caused by a worm but by a group of fungi called dermatophytes, which thrive on keratin, a tough, fibrous protein found in skin and hair. This highly contagious infection can affect people and animals and is characterized by itching, redness, and often a distinctive ring-shaped rash.
Globally, fungal skin infections are estimated to affect more than 650 million people at any given time, with ringworm accounting for over half of these cases. In some regions, particularly in resource-poor tropical settings, the prevalence of scalp ringworm infections among children under 10 years old can exceed 25% of school pupils. While ringworm is found in every country, certain forms are more prevalent in specific environments, sometimes leading to outbreaks in schools or posing occupational health challenges.
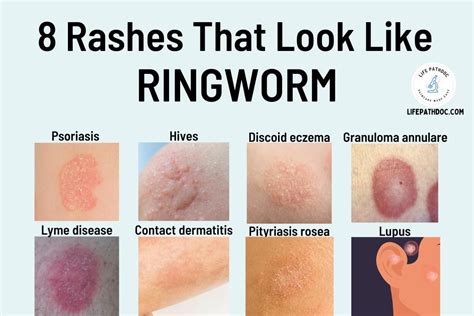
Scope of the Problem and Risk Factors
Tinea is one of the most common dermatological conditions worldwide. Its prevalence is substantial, especially in developing countries. While sporadic cases occur in high-income countries, outbreaks can emerge, particularly in settings like schools. Tinea pedis (athlete's foot) is often endemic in heavy industries, potentially leading to work absence and complications from secondary bacterial infections. A growing global concern is the emergence of drug-resistant ringworm strains, which are proving difficult to treat with common antifungal medications.
Several factors can increase an individual's risk of developing ringworm:
- Age: While ringworm can affect people of all ages, scalp infections are particularly common among school children.
- Exposure: Close contact with an infected person or animal is a primary risk factor for transmission.
- Immune Status: Individuals with weakened immune systems are more susceptible to tinea infections, which may also present with atypical symptoms.
- Lifestyle: Athletes, especially those involved in contact sports, and industrial workers face a higher risk due to shared equipment, changing rooms, and close physical contact.
- Environment: Fungi thrive in warm, moist environments. Areas like showers, locker rooms, and swimming pools can harbor the fungus.
- Sharing Personal Items: Sharing clothing, towels, combs, hairbrushes, and other personal items can facilitate the spread of infection.
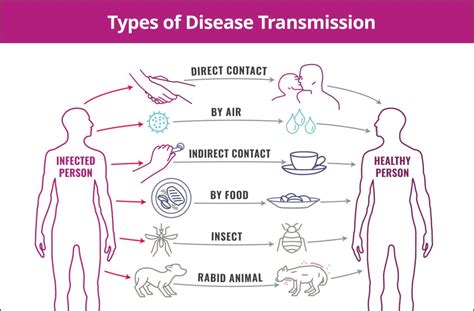
Transmission of Ringworm
Ringworm is contagious and can spread through several pathways:
- Direct Contact: Skin-to-skin contact with an infected person or animal.
- Indirect Contact: Touching contaminated objects or surfaces such as clothing, towels, floors, sports equipment, hairbrushes, or bedding.
- Environmental Contact: Exposure to the fungi present in soil.
Symptoms of Ringworm
The symptoms of ringworm can vary depending on the location of the infection on the body. The onset of symptoms typically occurs 4 to 14 days after exposure.
Tinea Capitis (Scalp Ringworm)
This form of ringworm affects the scalp and is more common in children. Symptoms include:
- Itching
- Redness
- Hair loss, which can be significant and potentially permanent if not treated promptly.
- Patches of dry, scaly skin.
- Brittle hair that breaks off easily.
- Sometimes, crusty areas may develop, which can be mistaken for dandruff.
- In severe cases, the affected area can become boggy (spongy), discharge pus, and develop areas of hair loss, forming lesions known as kerions.
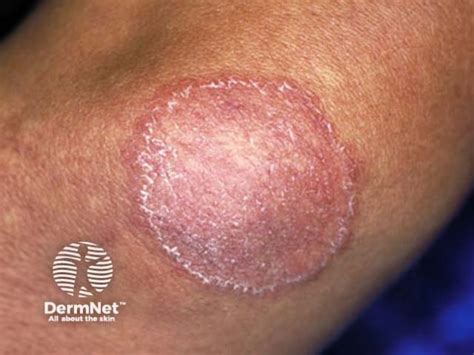
Tinea Corporis (Body Ringworm)
This type of ringworm appears on the skin, often on the trunk, limbs, or face. It is characterized by:
- A characteristic ring-shaped rash with raised, red borders.
- The inside of the ring may clear, giving it a distinct appearance.
- The rash can be itchy and may spread to other parts of the body.
- It can become very widespread, covering large areas of the body.
Tinea Cruris (Groin Ringworm or Jock Itch)
Affecting the groin and upper thighs, this is more common in adolescent and adult males, often associated with activities that lead to sweating and wearing tight clothing. Symptoms include:
- Scaly, itchy, red spots in the groin area.
Tinea Pedis (Foot Ringworm or Athlete's Foot)
This infection occurs on the feet, particularly between the toes, but can also affect the sole and heel. Symptoms include:
- Itching, burning, and scaling of the skin.
- Dry, cracked skin, especially between the toes.
- In severe cases, blisters may form.
- It can spread in workplace or public changing rooms and can be an occupational problem in certain industries.
Tinea Unguium (Nail Ringworm or Onychomycosis)
This affects the fingernails and toenails, causing them to become:
- Thick
- Discolored
- Brittle
- Easily breakable
- This can impair mobility, especially in the elderly.
Tinea Barbae (Beard Ringworm)
Occurring on the cheeks, chin, and upper neck, this form of ringworm presents as:
- Scaly, itchy, red spots.
- The spots might become crusted over or filled with pus.
- Hair loss may occur in the affected areas.
Diagnosis of Ringworm
Ringworm is typically diagnosed based on its characteristic appearance and symptoms. A healthcare provider may also perform additional tests to confirm the diagnosis:
- Skin Scraping or Nail Clipping: A small sample of affected skin or nail is collected.
- Microscopic Examination: The sample is examined under a microscope.
- Fungal Culture or Molecular Diagnosis: The sample may be sent to a laboratory for further testing to identify the specific fungus.
Treatment of Ringworm
The treatment for ringworm depends on the location and severity of the infection. Mild cases often clear up within a few weeks, while more serious infections may require treatment for six to 12 weeks.
Over-the-Counter (OTC) Antifungal Medications
For mild cases, nonprescription (over-the-counter) antifungal medications are usually effective. These come in various forms:
- Creams, Gels, or Powders: Applied directly to the affected skin. Common OTC products include:
- Clotrimazole (Lotrimin®, Mycelex®)
- Miconazole (Desenex®)
- Terbinafine (Lamisil AT®)
- Tolnaftate (Tinactin®)
It is important to apply these creams, lotions, or ointments for the entire treatment period, even after the rash has cleared, to ensure the infection is fully eradicated. Creams should typically be applied for an extra week after the rash has disappeared.
Prescription Medications
For more widespread infections, or when OTC treatments are ineffective, a healthcare provider may prescribe stronger medications:
- Oral Antifungal Medication: These are prescribed for ringworm on the scalp, nails, or when the infection is widespread on the body. Common oral medications include:
- Fluconazole (Diflucan®)
- Griseofulvin (Griasctin®)
- Itraconazole (Sporanox®)
- Terbinafine (Lamisil®)
- Most oral antifungal medications are prescribed for a duration of one to three months.
Antifungal Shampoo
For scalp ringworm (tinea capitis), antifungal shampoos, such as ketoconazole shampoo (Nizoral A-D®), can help stop the infection from spreading. However, these shampoos typically do not cure the infection on their own and should be used in conjunction with prescribed oral antifungal medication. Unaffected family members may also benefit from using the shampoo as a preventative measure.
Antifungals
Home Remedies and Other Treatments
While some home remedies like apple cider vinegar or tea tree oil are sometimes suggested, they have little to no proven benefit for treating ringworm. Apple cider vinegar may even cause irritation or open sores. Tea tree oil possesses some antifungal properties, but its efficacy for ringworm is not well-established.
Corticosteroid creams may help reduce inflammation associated with skin conditions, but they should not be used to treat ringworm, as they can potentially worsen the infection.
Promoting Healing and Preventing Spread
In addition to medication, several practices can promote healing and prevent the spread of ringworm:
- Keep the affected area clean and dry.
- Avoid touching the infected area and wash hands thoroughly before touching other parts of your body to prevent spreading the fungus.
- Cover the rash with clothing or a dressing, especially when in public or at school, to avoid transmission.
- Wash clothes, sheets, and towels in hot water and detergent to kill the fungus.
- Disinfect living spaces using disinfectant sprays like Lysol® or bleach, as the ringworm fungus can survive on surfaces for months.
- If ringworm is on the feet, spray shoes with anti-fungal spray.
- Wash hands properly after playing with pets.
Note: There is generally no need to keep a child home from school if they have ringworm, provided the rash is covered to prevent spreading it to others. Treatment should be started promptly.
Prevention of Ringworm
There is no vaccine to prevent ringworm, but several simple measures can significantly lower the risk of infection:
- Keep your skin and fingernails clean and dry, paying special attention to areas prone to sweating.
- Avoid sharing personal items such as sports gear, towels, socks, and hairbrushes.
- Wear protective footwear in public areas like bathrooms, showers, locker rooms, and pool areas.
- Regularly clean and disinfect surfaces and objects that may be contaminated.
- Avoid skin-to-skin contact with individuals or animals known to have ringworm.