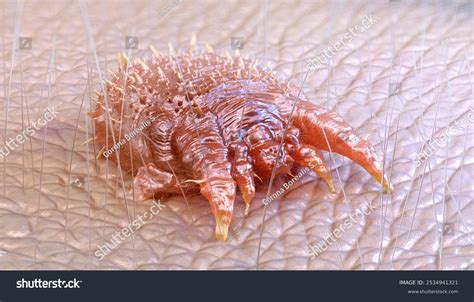
Scabies is a contagious skin disease caused by the microscopic mite Sarcoptes scabiei. While it can affect individuals in any climate, it is particularly prevalent among children under the age of two and is endemic in tropical regions. The female mite, with a lifespan of approximately 30 days, burrows into the epidermis to lay eggs. These eggs hatch into larvae within three to four days, and the larvae mature into adult mites over the subsequent 14 to 17 days. Male adult mites are smaller than females and typically die shortly after mating, remaining on the skin's surface.
Symptoms of scabies infestation are characterized by a rash and intense pruritus, which is often exacerbated at night. The initial lesions appear as small erythematous papules and can progress to vesicles or pustules. While linear burrows are a classic diagnostic feature, they are not always readily apparent. Excoriation and ulceration may also be present, and in some cases, a more generalized hypersensitivity reaction, including urticaria, can occur. Common areas affected by scabies include the axillae, the web spaces between fingers, and the flexor surfaces of the wrists. The male genitalia, female breasts, gluteal crease, waistband, and antecubital fossae are also frequently involved. A typical distribution of lesions, severe itching, and patchy, discrete lesions with secondary excoriation are strong indicators of scabies infection.
Historical and Modern Treatment Approaches
For centuries, topical sulfur treatments have been employed to manage scabies infections. More recently, topical benzyl benzoate and lindane were considered primary therapeutic agents. However, a comparative study in 1990 revealed that topical permethrin (Nix) demonstrated superior efficacy to lindane after 28 days, with a reduced risk of neurotoxicity.
In 1993, a study comparing oral ivermectin with topical 10% benzyl benzoate indicated that while ivermectin showed favorable absolute results, the difference in efficacy was not statistically significant. A smaller study involving both healthy individuals and those with human immunodeficiency virus (HIV) suggested that a single dose of ivermectin (200 mcg per kg) was curative for most patients. However, several HIV-infected patients required a second dose two weeks later, and one patient needed a third dose of ivermectin combined with topical permethrin for complete resolution of the infection.
A randomized study involving 53 patients compared topical lindane with oral ivermectin. Fifteen days post-treatment, 74% of patients treated with ivermectin and 59% of those using topical lindane were cured. This difference was not statistically significant. At the four-week follow-up, one patient treated with ivermectin and two patients treated with lindane still showed signs of ongoing infection. Another study comparing oral ivermectin with topical 5% permethrin found that fewer patients responded to ivermectin at the one- and two-week follow-ups compared to permethrin. At the end of the second week, patients who did not respond to either treatment repeated their assigned dose. By the end of the fourth and eighth weeks, all but two patients in the ivermectin group and all patients in the permethrin group were cured, a difference that was not statistically significant.
Ivermectin in Scabies Treatment
An estimated 6 million people globally have taken ivermectin for various parasitic infestations, with no serious drug-related adverse events reported. While standard topical treatments are effective for many scabies patients, oral ivermectin may play a crucial role in managing refractory infestations or in situations where adherence to topical application is challenging, such as in large institutional outbreaks or with individuals who have cognitive impairments. Immunocompromised patients with crusted scabies, who have particularly high parasite loads, may also benefit from oral ivermectin treatment.
The cost of a single dose of ivermectin for a 70 kg adult is approximately $38 for three 6 mg pills or about $67 for the same dose in 3 mg pills. In comparison, lindane (2 oz of 1% lotion) costs about $17, and permethrin (2 oz of 5% cream) costs approximately $38.
FDA Approval and Off-Label Use
Products used to eradicate scabies mites are known as scabicides. Permethrin is a synthetic pyrethroid, similar to naturally occurring pyrethrins derived from chrysanthemum flowers. Permethrin 5% cream is applied to the entire body from the neck down and washed off after 8-14 hours. It is generally safe and effective with a single application, though two or more applications, spaced about a week apart, may be necessary for complete eradication of mites. Additional treatment may be required if new symptoms arise.
Oral ivermectin tablets are not FDA-approved for the treatment of scabies. Nevertheless, topical permethrin and oral ivermectin demonstrate similar efficacy in curing scabies. For classic scabies, it is recommended to take two doses of oral ivermectin (200µg/kg per dose) with food, each spaced 7 to 14 days apart. The safety of ivermectin in children weighing less than 15 kg and in pregnant women has not been established.
The choice between topical permethrin and oral ivermectin may depend on patient preference for topical versus oral therapy, potential drug interactions with ivermectin (such as with azithromycin, trimethoprim/sulfamethoxazole, or cetirizine), and cost.
Scabies and ivermectin
Alternative and Adjunctive Treatments
Several alternative medications are available for scabies treatment, with providers considering factors such as availability, efficacy, cost, adverse effects, and patient preferences when selecting a therapy. Limited data exists for direct comparisons of these alternative treatments.
- Crotamiton lotion 10% and Crotamiton cream 10%: Crotamiton is approved by the US Food and Drug Administration (FDA) for scabies treatment in adults and is considered safe when used as directed. It is not FDA-approved for children.
- Sulfur ointment: Sulfur in an ointment base (petrolatum) is safe for topical use in children, including infants under two months of age.
- Malathion lotion 0.5%: Malathion is not FDA-approved for scabies but is recommended in international treatment guidelines.
- Spinosad topical suspension 0.9%: This topical treatment received FDA approval in 2021 for scabies infestations in patients aged 4 years and older.
- Lindane lotion 1%: Although FDA-approved, lindane is not recommended as a first-line therapy due to potential neurotoxicity if overused, misused, or accidentally ingested. Its use should be reserved for patients who have failed other treatments or cannot tolerate less risky medications. Lindane is contraindicated in premature infants, individuals with uncontrolled seizure disorders, crusted scabies, and those with skin conditions that may increase systemic absorption.
Crusted Scabies Management
For crusted scabies, oral ivermectin should be administered concurrently with a topical agent. There is no definitive consensus on the optimal frequency of ivermectin administration, with some experts suggesting three doses (days 1, 2, and 8), five doses (days 1, 2, 8, 9, and 15), or even seven doses (days 1, 2, 8, 9, 15, 22, and 29), depending on the severity of the infection. The safety of ivermectin in children weighing less than 15 kg and in pregnant women remains unestablished.
Topical permethrin 5% cream should also be applied to the entire body for crusted scabies, in conjunction with an oral agent. A topical keratolytic cream may be beneficial to reduce skin crusting and enhance the penetration of topical permethrin in affected areas.
Clinical Trial Findings: Ivermectin vs. Permethrin
A multicenter, assessor-blinded, cluster-randomized clinical trial, known as the Scabies Randomised Trial in Children and Adults (SCRATCH), investigated the efficacy of oral ivermectin versus topical 5% permethrin cream in treating classic scabies. The trial involved 28 French hospitals and included both children and adults confirmed to have scabies by dermoscopy.
Participants were randomly assigned to receive either oral ivermectin (200 µg/kg) or 5% permethrin cream, with treatments administered on days 0 and 10. All members of an index case's household (cluster) received the same treatment as the index case, with the exception of children weighing less than 15 kg, who were prescribed topical 5% permethrin.
The primary outcome was clinical cure of the cluster on day 28, defined as the disappearance of scabies signs and symptoms for all household members. Secondary outcomes included individual-level cure rates for index cases and all participants, as well as safety assessments.
Results of the SCRATCH Trial
The trial included 507 participants in 142 households treated with ivermectin and 568 participants in 147 households treated with permethrin. Cluster-level cure rates were 71.8% for ivermectin compared to 88.5% for permethrin, indicating a statistically significant inferiority of ivermectin (-16.7 percentage point difference, 95% CI -26.3 to -7.1).
Secondary outcome analyses also showed that ivermectin was less effective than 5% permethrin for index cases (76.6% vs. 91.5%; -14.9 percentage point difference, 95% CI -23.6 to -6.2) and for all participants (85.3% vs. 94.2%; -9.2 percentage point difference, 95% CI -14.9 to -3.5).
Intraclass correlation coefficients, which measure the similarity of outcomes within clusters, were higher for permethrin than for ivermectin, suggesting better consistency of treatment effect within households for permethrin. Cutaneous adverse events were reported in 11.9% of participants treated with ivermectin and 15.6% of those treated with permethrin.
Conclusions of the SCRATCH Trial
The results of this cluster-randomized trial did not demonstrate the non-inferiority of oral ivermectin compared to 5% permethrin cream for the clinical cure of classic scabies on day 28 in index cases and their household members. Conversely, the trial indicated the statistical superiority of 5% permethrin cream.

Diagnosis and Management of Scabies
Diagnosing scabies typically involves a healthcare professional examining the skin for characteristic signs of mite infestation. In some cases, a skin scraping may be taken to identify mites or their eggs under a microscope. Treatment aims to eradicate the mites and their eggs using a medicated cream or oral medication. Due to scabies' highly contagious nature, it is often recommended that all individuals in a household and close contacts be treated simultaneously.
Key Treatment Modalities
- Permethrin cream: A widely used topical treatment that kills scabies mites and their eggs. It is usually applied from the neck down and left on for 8 to 14 hours, often overnight. Two treatments, spaced about a week apart, may be necessary.
- Sulfur cream: Another topical option, typically applied overnight and washed off in the morning, used for 5 to 7 consecutive nights.
- Ivermectin: An oral medication prescribed when topical treatments are ineffective, particularly for crusted scabies or in individuals with compromised immune systems.
Itching may persist for several weeks even after successful treatment. Over-the-counter medications like antihistamines and calamine lotion can help alleviate itching. It is crucial to consult a healthcare provider for proper diagnosis and treatment, especially if symptoms persist or worsen.
Environmental and Personal Hygiene Measures
To prevent reinfestation and transmission, several environmental and personal hygiene measures are recommended:
- Laundering: All clothing, bed linens, and towels used within the past week should be washed in hot water (50°C or higher) and dried on a hot cycle.
- Isolation of non-washable items: Items that cannot be washed should be sealed in a plastic bag for at least 7 days.
- Vacuuming: Carpets and upholstered furniture should be thoroughly vacuumed, with vacuum bags immediately discarded.
- Avoiding skin-to-skin contact: Individuals with scabies should avoid close physical contact with others until treatment is completed.
Mass screening and treatment programs have shown significant reductions in scabies prevalence in affected communities. However, ongoing efforts are necessary to maintain these gains. For persistent or severe cases, re-examination and re-initiation of treatment may be required, alongside an investigation into potential sources of reinfection among close contacts.
tags: #scabies #ivermectin #treatment