Candida albicans is a fungus that naturally resides in the human body, including the gut, mouth, throat, vagina, and skin. Under normal conditions, it exists in balance with other microorganisms like bacteria, viruses, and fungi, forming a healthy microbiome and typically causing no harm. However, when conditions allow for its uncontrolled growth, it can lead to an imbalance known as candidiasis or candida overgrowth.
This overgrowth is thought by some to contribute to a variety of symptoms, including fatigue, headaches, poor memory, bloating, gastrointestinal discomfort, skin rashes, frequent vaginal yeast imbalances, thrush (a white coating on the tongue), and feelings of fatigue. The overgrowth in the gastrointestinal (GI) tract is often associated with an imbalance in the gut flora of bacteria, viruses, and fungi, or issues with the immune system that permit the yeast to multiply beyond normal levels. A diet high in sugar and processed foods is frequently cited as a significant contributing factor.
While there is little definitive proof that diet changes alone can resolve significant yeast overgrowths, many individuals report feeling better when following a candida cleanse diet. This is often attributed to the removal of processed foods, sugar, and refined carbohydrates, which are replaced with nutrient-dense, fresh foods and whole grains. This dietary shift can lead to general improvements in well-being.
What is Candida Overgrowth?
Candida albicans is the most common type of yeast found in the human body. In a balanced state, it is a normal component of the gut, mouth, throat, vagina, and skin microbiome. The gut mycobiome, which includes various fungi, is a small but vital part of the overall gut microbiome, working alongside bacteria to support immunity and manage inflammation.
When the body's internal ecosystem is disrupted by imbalanced nutrition, medications, or factors impacting the immune system, candida can multiply beyond its normal levels. This disruption allows candida to overgrow, potentially leading to symptoms throughout the body.
Candida Overgrowth Symptoms
The symptoms of candida overgrowth can vary depending on the location of the imbalance. Common gastrointestinal symptoms include:
- Belching
- Bloating
- Gas
- Indigestion
- Fullness in the upper abdomen
- Nausea
- Diarrhea
If candida overgrowth extends beyond the gut, systemic symptoms may occur, such as:
- Red patches of skin with small, raised bumps
- Itching
- Burning
- White or yellow cottage cheese-like vaginal discharge
- White patches on the tongue or sores in the mouth causing loss of taste or discomfort
- Joint discomfort
- Chronic fatigue

Gastrointestinal Problems
Candida overgrowth in the GI tract can impact the gut lining, potentially increasing the risk of leaky gut syndrome (gut permeability) and further imbalancing the microbiome. This can manifest as general irritable bowel syndrome (IBS) symptoms like bloating, discomfort, constipation, and diarrhea. The excess candida can ferment carbohydrates, producing gases that contribute to bloating. This fermentation can also produce ethanol/alcohol, potentially mimicking food intolerances or sensitivities.
Small intestinal fungal overgrowth (SIFO) is a specific type of dysbiosis where an excess of fungi or yeast proliferates in the small intestine. This can lead to similar GI symptoms and, over time, nutrient imbalances and weight changes if not addressed.
Feelings of fatigue can arise because gut imbalances associated with candida overgrowth can affect the immune system and lead to deficiencies in nutrients like vitamin B6, essential fatty acids, and magnesium. These imbalances can contribute to inflammation and nutrient deficiencies.
Autoimmunity
Candida overgrowth can compromise the gut lining, allowing toxins, microbes, proteins, and undigested food particles to enter the bloodstream. The immune system may identify these as pathogens, triggering an immune response. This can contribute to food sensitivities, tissue-specific immune reactions, and chronic inflammation. Research suggests a link between candida overgrowth and conditions such as Sjogren's syndrome, gastric ulcers, ulcerative colitis, and Crohn's disease.
Vaginitis
When candida overgrows in the gut, it can also lead to imbalances in the vaginal flora, resulting in vaginal candidiasis. Symptoms include burning, itching, redness, and discharge from the vagina.
Skin and Nail Infections
An imbalance in the gut microbiome can be accompanied by an imbalance in the skin microbiome. Candida, which normally lives on the skin's surface, can cause an imbalance called cutaneous candidiasis when it overgrows. This often occurs in warm, moist skin folds, presenting as a raised, red patch with itchy bumps. In some cases, the fungi can infect the nails, leading to nail fungus.
Oral Candidiasis (Thrush)
Candida overgrowth in the mouth leads to an imbalance causing white patches or sores known as thrush. This can affect the mouth, throat, esophagus, or tongue.
Frequent Urinary Tract Infections (UTI)
While typically caused by bacteria, Candida albicans, being an opportunistic organism, can overgrow in the urinary tract, contributing to frequent UTIs.
Invasive Candidiasis (Systemic Candidiasis)
When a candida imbalance spreads into the bloodstream (candidemia), it can lead to a serious systemic condition affecting the blood, heart, brain, eyes, bones, and other organs. Candidemia is a common cause of bloodstream infections in hospitalized patients in the US, with growing concern over drug-resistant strains like candida auris.
What Causes Candida Overgrowth in the GI Tract?
Several factors can increase the likelihood of candida overgrowth:
- Weakened Immune System: Illnesses or medications such as steroids, chemotherapy, or immunosuppressants can compromise the immune system, allowing candida to overgrow or spread into the bloodstream.
- Gut Dysbiosis: An imbalance between beneficial and harmful microbes in the gut can allow candida to multiply rapidly. This imbalance can result from:
- Antibiotic Use: Antibiotics can eliminate not only harmful bacteria but also beneficial ones.
- Low Stomach Acid: Reduced stomach acid, which is crucial for controlling bacteria and fungi before they reach the small intestine, increases fungal overgrowth risk. This can be caused by long-term use of proton-pump inhibitors (PPIs), aging, nutrient deficiencies (protein, iron, calcium, vitamin B12), H. pylori infection, and atrophic gastritis. PPIs reduce acid production and inhibit beneficial bacteria like Lactobacillus species.
- Diet: A diet high in refined carbohydrates, sugars, or excessive alcohol can lead to dysbiosis and candida overgrowth.
- Diabetes: Higher blood sugar levels in individuals with diabetes can dysregulate the immune system and promote candida growth.
- Slowed Gastrointestinal Motility: When food moves slowly through the small intestine, it increases the risk of candida overgrowth. Causes include diabetes, Ehlers-Danlos syndrome, colectomy surgery, gastroparesis, thyroid disorders (hypothyroidism, Hashimoto's), and sedentary behavior.
- Inflammatory Bowel Disease (IBD): Conditions like Ulcerative Colitis and Crohn's disease, and their treatments (e.g., anti-TNFa agents), can affect gastrointestinal health and allow pathogens like candida to overgrow.
- Chronic Stress: High stress levels can impact the immune system and disrupt the gut microbiome.
- Heavy Metal Exposure: Heavy metals can affect the immune system and microbiome, creating an environment conducive to candida overgrowth. Candida can absorb heavy metals into biofilms, potentially giving it an advantage.

Functional Medicine Approach to Candida Overgrowth
A functional medicine approach aims to uncover and address the underlying factors that allow fungi to overgrow. This often involves advanced lab testing, dietary changes, lifestyle modifications, and targeted supplements to rebalance the body. For instance, focusing on non-starchy vegetables, lean protein, healthy fats, and gluten-free grains can help prevent candida overgrowth.
Functional Medicine Labs for Testing
Several laboratory tests can help identify the root causes of candida overgrowth and personalize treatment:
Evaluating the Microbiome
- Comprehensive Stool Tests (e.g., GI-MAP, GI-Effects Gut Pathogen Profile): These tests evaluate the balance of the microbiome, measuring levels of candida species and other fungal organisms. They can help identify candida overgrowth and investigate potential causes like dysbiosis.
Candida Testing
- Blood Tests (e.g., Candida Profile): Measuring IgA, IgG, and IgM reactivity to candida can indicate an immune reaction.
- Urine Testing (e.g., Candida Panel): Detects candida DNA to help identify invasive fungal imbalances.
Heavy Metal Testing
- A heavy metals profile measures accumulated heavy metals that may contribute to candida overgrowth and affect immune function.
SIBO Testing
- Breath Tests: A 3-hour breath test assesses for bacterial overgrowth in the small intestine (SIBO), which often co-occurs with SIFO and can present with similar symptoms.
Small Bowel Aspirate Test
Considered the "gold standard" for identifying SIFO, this procedure involves collecting fluid during an upper endoscopy for laboratory analysis of abnormal fungi or bacteria.
Urinalysis
If a UTI is present, a urinalysis and urine culture can confirm if the infection is bacterial or yeast-related.
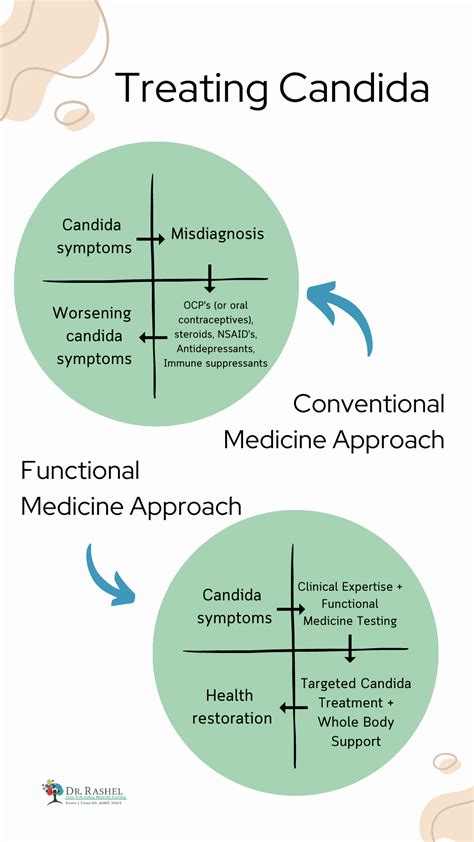
Conventional Approaches for Candida Overgrowth
Conventional medical treatment for candida overgrowth typically involves antifungal medications. These include oral 'azole' antifungals like fluconazole, itraconazole, or posaconazole, which inhibit fungal growth by disrupting the cell membrane. Other medications such as caspofungin, terbinafine, and amphotericin B may also be used, sometimes in combination with -azole drugs for increased efficacy.
Functional Medicine Approach for GI Candida Overgrowth
The functional medicine approach focuses on addressing the underlying root causes of candida overgrowth in the GI tract through a combination of optimized nutrition, natural therapies, and lifestyle modifications. Treatment plans are individualized based on a patient's specific factors.
Therapeutic Diet and Nutrition Considerations
A dietary approach to candida overgrowth involves focusing on low-sugar fruits, non-starchy vegetables, gluten-free grains, some fermented foods, and specific dairy products. Diets such as the Anti-Candida, Low FODMAP, anti-inflammatory Mediterranean diet, and elemental diets may be employed.
Blood sugar dysregulation, often stemming from high-carbohydrate diets, can create an environment conducive to candida proliferation. Therapeutic diets for candida overgrowth typically avoid sugars (including honey and artificial sweeteners), high fructose corn syrup, alcohol, and starchy carbohydrates like potatoes.
Reducing inflammation is also critical. An individualized anti-inflammatory diet should exclude known allergens or sensitivities, processed meats, sodas, sweetened beverages, and processed oils.
The Anti-Candida Diet
This diet emphasizes low-sugar, anti-inflammatory foods to promote a healthy microbiome, manage inflammation, support the immune system, and stabilize blood sugar levels. It aims to reduce yeast overgrowth and restore microbial balance.
The Low FODMAP Diet
This diet limits short-chain carbohydrates that are difficult to digest and can feed yeast and bacteria in the small intestine.

Foods to Include on the Candida Diet
- Low-sugar fruits (in moderation): Lemon, limes, berries.
- Non-starchy vegetables: Asparagus, broccoli, Brussels sprouts, cabbage, kale, celery, cucumber, eggplant, onion, spinach, zucchini, tomatoes, rutabaga.
- Gluten-free grains: Millet, quinoa, oat bran, buckwheat.
- High-quality protein: Organic, pasture-raised chicken, eggs, wild-caught salmon, turkey, sardines.
- Healthy fats: Avocado, olives, unrefined coconut oil, flax oil, extra-virgin olive oil, sesame oil.
- Certain dairy products: Butter, ghee, organic kefir, plain yogurt.
- Low-mold nuts and seeds: Almonds, sunflower seeds, coconut, flaxseed.
- Herbs and spices: Black pepper, salt, cinnamon, dill, garlic, ginger, oregano, rosemary, paprika, turmeric, thyme.
- Condiments: Apple cider vinegar, coconut aminos, sauerkraut.
- No-sugar sweeteners: Stevia, erythritol, xylitol.
- Non-caffeinated beverages: Herbal teas, filtered water, homemade almond milk, coconut milk.
Foods to Avoid on the Candida Diet
- High-sugar fruits: Bananas, dates, raisins, grapes, mango.
- Grains containing gluten: Wheat, rye, barley, spelt.
- Certain meats: Deli meats, farm-raised fish.
- Refined oils and fats: Canola oil, soybean oil, sunflower oil, margarine.
- Condiments: Ketchup, soy sauce, white vinegar, BBQ sauce, horseradish, mayonnaise.
- Certain dairy products: Cheese, milk, cream.
- Sugars and artificial sweeteners: Aspartame, agave, cane sugar, corn syrup, honey, maple syrup, molasses, table sugar, malitol, sorbitol, fructose, glucose, sucrose.
- Nuts and seeds higher in mold: Peanuts, cashews, pecans, pistachios.
- Caffeine, alcohol, and sugary beverages: Caffeinated teas, coffee, energy drinks, soda, fruit juice, beer, wine, spirits.
- Additives: Nitrates, sulfates.
- Yeast-containing foods: Bread, beer.
- Moldy foods: Mushrooms, peanuts, pistachios, cashews.
- Fermented foods containing vinegars: Salad dressings, pickles, ketchup, mustard, mayonnaise.
- Starchy vegetables: Potatoes, corn, beans, peas.
What I ate during my Candida Cleanse + my diet a year later | Candida Overgrowth
Candida Cleanse Protocol
Before starting the candida diet, proponents often recommend a short-term candida cleanse. This is believed to reduce stress on the digestive tract and release toxins. While scientific studies do not support the benefits of a candida cleanse, it may help individuals transition into the stricter candida diet mindset. Cleanse methods can include fluid-only intake (e.g., lemon water, bone broth) or a diet primarily of vegetables with a small amount of protein. Some individuals may experience temporary side effects like fatigue, headaches, or mood swings during a cleanse, which should not last more than a few days.
Duration of the Candida Diet
There is no specific timetable for the candida diet. Proponents suggest that symptom relief can occur within weeks or months. It is advisable to work with a healthcare provider to ensure adequate nutrient intake while following the diet.
Considerations Before Starting the Candida Diet
- Start Slowly: Gradually eliminate items like sugar, caffeine, and gluten rather than all at once.
- Short-Term Focus: The diet is intended for symptom management and not as a long-term eating plan.
Sample Meal Plan for the Candida Diet
Monday
- Breakfast: Scrambled eggs with tomatoes and avocado.
- Lunch: Turkey salad with greens, avocado, cabbage, broccoli, and olive oil dressing.
- Dinner: Quinoa stir-fry with chicken breast, steamed vegetables, and coconut aminos.
Tuesday
- Breakfast: Plain yogurt parfait with berries, cinnamon, and almonds.
- Lunch: Thai red curry chicken.
- Dinner: Salmon cakes with steamed broccoli and a cup of bone broth.
Wednesday
- Breakfast: Turkey-and-sage breakfast sausages with Brussels sprouts.
- Lunch: Lemon-roasted chicken over salad greens.
- Dinner: Hamburger patty (no bun) with avocado, steamed vegetables, and sauerkraut.
Thursday
- Breakfast: Vegetable omelet with eggs, shallots, spinach, and tomatoes.
- Lunch: Leftover turkey-and-sage breakfast sausages with sautéed cabbage.
- Dinner: Coconut curry chicken over quinoa and steamed vegetables.
Friday
- Breakfast: Omelet with red peppers, onions, kale, and fried eggs.
- Lunch: Turkey meatballs with a kale salad and millet topped with ghee.
- Dinner: Wild-caught salmon with lemon and dill, plus asparagus.
Saturday
- Breakfast: Buckwheat breakfast muffins with chicory coffee.
- Lunch: Leftover coconut curry chicken over quinoa and steamed vegetables.
- Dinner: Zucchini noodles with chicken, raw garlic, pesto, and olive oil.
Sunday
- Breakfast: Smoothie with plain kefir, berries, almond butter, coconut, and cinnamon.
- Lunch: Chef salad with hard-boiled eggs, turkey, tomatoes, cucumbers, olives, and olive oil dressing.
- Dinner: Chicken fajita bowl with chicken, peppers, onions, cilantro, avocado, and salad greens.
Potential Benefits and Downsides of the Candida Diet
Despite the lack of extensive scientific evidence, the candida diet may offer benefits due to its emphasis on whole, nutrient-dense foods. These foods can support weight loss, heart health, gut function, and reduce inflammation. Eliminating sugary foods is also beneficial for overall health, as they are linked to obesity, diabetes, heart disease, and metabolic syndrome.
However, a major pitfall is the limited and often controversial human research supporting its effectiveness. While one small study showed dietary changes reduced candida yeast in stool, the diet's strictness is a significant downside. Banning sugar, gluten, most fruits, starchy vegetables, certain meats, nuts, seeds, alcohol, and caffeine requires considerable adjustment. The diet can also be challenging for those on a budget or who dislike cooking and meal planning. It is typically intended for short-term use during symptom flare-ups.
The candida diet is claimed to help eliminate candida overgrowth by removing sugar, gluten, alcohol, and certain dairy products. It prioritizes organic, low-sugar, high-quality produce, meats, and fats. While laboratory studies suggest these substances may contribute to yeast growth, robust evidence for the candida diet as a treatment for yeast infections is lacking.
Research on the Candida Diet
High-quality research on the candida diet is scarce. Some small studies have examined the influence of sugar and gluten on candida growth. For instance, a test tube study indicated that sugar alternatives might reduce candida growth in the mouth, and a 2019 study found that wheat products were associated with increased candida growth. However, due to the complexity of diet and lifestyle, these studies are insufficient to prove the diet's efficacy. Nevertheless, reducing sugar intake and adopting a diet rich in fiber, healthy fats, and probiotics can benefit overall health.
Nutrient Considerations
Working with a healthcare provider is recommended when following the candida diet to ensure adequate nutrient intake. Probiotic supplements may also help alleviate inflammation, combat harmful organisms, and reduce candida symptoms.
Candida and Children
Candida overgrowth in children can result from excessive antibiotic use and diets high in processed carbohydrates and sugars. Candida can produce toxic metabolites like ammonia, acetaldehyde (which can make children act as if intoxicated), and gliotoxin. Functional medicine approaches for children often include antifungal compounds, beneficial yeasts, binders, probiotics, and liver support supplements like glutathione. Testing, such as organic acid tests (e.g., Genova Diagnostics Metabolomics Test, Great Plains Laboratories OAT test) and stool tests, can help assess yeast overgrowth. For mold exposure, tests like the Great Plains Laboratory MycoTOX Profile are useful.
It is crucial to address underlying issues and replenish the gut microbiome to maintain candida in check. A functional medicine-based approach considers diet, lifestyle, toxic load, mitochondrial function, and nutrient status to restore gut health. Always seek medical advice before making significant dietary changes or starting supplements.