Summer's arrival often ushers in a common yet frustrating foot condition: athlete's foot. Affecting up to 70% of adults at some point, this fungal infection, medically termed tinea pedis, typically surfaces when temperatures rise, leading to an increase in cases of itchy, burning rashes, particularly between the toes. Despite common knowledge about prevention, athlete's foot can be a persistent ailment, with over-the-counter fungal creams not always proving effective.
Understanding the Culprit: The Fungal Environment
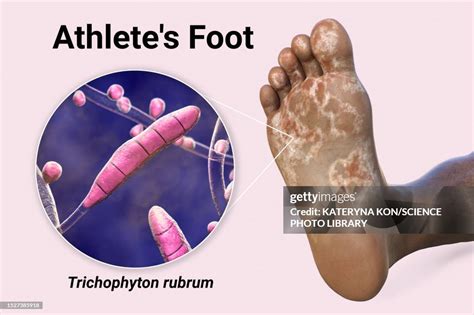
The dermatophyte fungus responsible for athlete's foot thrives in warm, moist conditions. This environment is readily created within shoes, especially during summer activities like swimming, running, or hiking, where sweat accumulates. Communal areas such as locker rooms, public showers, and swimming pools also provide fertile ground for these fungi, which can live in slightly damp conditions for weeks.
The Trichophyton fungus, a common cause of athlete's foot, requires two key elements to flourish: moisture and heat. When feet are kept dry, the risk of developing a fungal infection is significantly reduced, regardless of external temperatures.
Key Symptoms of Athlete's Foot
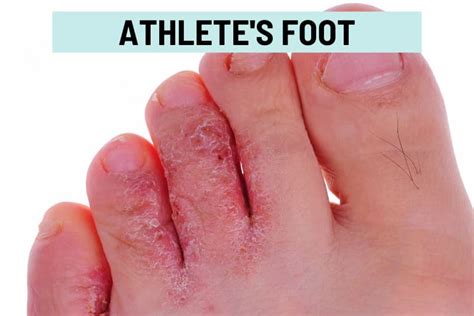
The most common symptoms of athlete's foot include burning, redness, flaking, and itchiness. In more severe cases, the skin of the foot may crack, making it more vulnerable to secondary bacterial infections and causing significant soreness that can impede daily activities. Blisters can also form, and the affected areas might become dry or scaly, extending beyond the toes to other parts of the foot. While not life-threatening, athlete's foot can become quite bothersome and spread to other body parts if not treated properly.
Preventive Measures: Keeping Your Feet Dry and Healthy
Proactive foot hygiene is paramount in preventing athlete's foot, especially during warmer months. This involves a multi-faceted approach focusing on footwear, socks, and personal habits.
Footwear Choices and Care
- Avoid thick and tight shoes: These can constrict your feet and trap moisture.
- Invest in quality shoes: Opt for footwear made from breathable materials like leather or canvas. Shoes with plastic components tend to heat up faster and have poor breathability.
- Rotate your shoes: Switching between two pairs of shoes daily allows them adequate time to dry completely. The materials inside shoes can hold moisture longer than the exterior suggests, and fungal spores can persist for weeks in slightly damp conditions.
- Remove shoes after exercising: This allows your feet to air out.

The Importance of Socks
- Choose moisture-wicking socks: Materials like wool, bamboo, or specialized synthetic blends are superior to cotton. Cotton absorbs moisture and holds it against the skin, whereas wool fibers wick moisture away, allowing the sock's surface to remain relatively dry.
- Switch socks when damp: Waiting until your socks feel damp is often too late, as the fungus begins to multiply immediately in moist conditions. Think ahead and change socks proactively.
- Consider sock height: Socks that come higher on the leg offer more fabric for moisture to spread and dissipate.
Personal Hygiene and Habits
- Wash and dry feet thoroughly: Regularly wash your feet with soap and lukewarm water, paying close attention to drying the areas between your toes, where moisture tends to accumulate.
- Wear sandals in communal areas: To minimize direct contact with potentially contaminated surfaces in places like gym locker rooms, public showers, and pool areas, wear flip-flops or water shoes.
- Do not share footwear or sandals: Athlete's foot is contagious, and sharing shoes can easily spread the infection.
- Keep nails trimmed and clean: Long nails can harbor dirt and fungus, creating an entry point for infections.

When to Seek Professional Help
While over-the-counter treatments and home remedies can be effective for early or mild cases of athlete's foot, professional medical attention may be necessary in certain situations:
- Persistent Symptoms: If symptoms do not significantly improve after two weeks of using over-the-counter antifungal treatments, prescription-strength medication may be required.
- Worsening Condition: An increase in redness, swelling, the development of blisters, or increased pain indicates the infection may be escalating.
- Underlying Health Conditions: Individuals with diabetes, a weakened immune system, or circulatory issues are at a higher risk of complications from foot infections. In these cases, prompt medical evaluation is crucial. Pregnant women should also consult a healthcare professional, as OTC antifungals may not be suitable.
A healthcare professional can perform diagnostic tests to confirm the fungal infection and recommend a personalized treatment plan, which may include prescription topical or oral antifungal medications.
How to help knock out Athlete's Foot
tags: #control #athletes #moisture #wicking #prevention