A subconjunctival hemorrhage is a condition characterized by a bright red patch on the white of the eye, caused by a broken blood vessel in the conjunctiva. The conjunctiva is a thin, transparent membrane that covers the inner surface of the eyelids and the anterior part of the eyeball. This condition can appear alarming due to its sudden onset and noticeable appearance, but it is typically harmless and does not affect vision or cause pain.
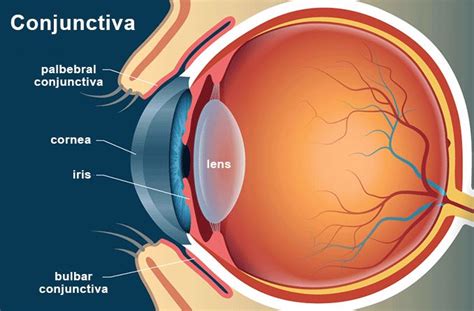
Understanding the Anatomy of the Eye
To understand a subconjunctival hemorrhage, it's important to know about the eye's structure. The sclera is the white, fibrous outer layer of the eyeball. Covering the sclera and lining the eyelids is the conjunctiva. This delicate membrane contains numerous tiny blood vessels responsible for supplying oxygen and nutrients to the eye. When one of these small vessels breaks and bleeds, the blood pools beneath the conjunctiva, creating a distinct red spot on the white of the eye.
What Causes a Subconjunctival Hemorrhage?
In many instances, the exact cause of a subconjunctival hemorrhage remains unknown. However, certain factors and health conditions can increase the likelihood of these blood vessels breaking:
Sudden Increases in Pressure
- Straining: Vigorous physical exertion, such as during strenuous exercise, lifting heavy objects, constipation, or even forceful bowel movements, can temporarily increase blood pressure and lead to vessel rupture.
- Coughing or Sneezing: Sudden, forceful coughing or sneezing can exert significant pressure on the delicate blood vessels in the eye.
- Vomiting: Similar to coughing and sneezing, vomiting can cause a rapid increase in intraocular pressure.
Eye Injury and Irritation
- Direct Trauma: Even minor trauma to the eye, such as rubbing it too vigorously, a slight poke, or an accidental bump, can cause a blood vessel to break.
- Contact Lens Use: The process of inserting or removing contact lenses can sometimes lead to irritation or minor injury that results in a hemorrhage.
- Foreign Bodies: The presence of dust, dirt, or other particles in the eye can cause irritation and lead to rubbing, potentially causing a vessel to break.
Underlying Medical Conditions
- High Blood Pressure (Hypertension): Chronically elevated blood pressure can weaken blood vessel walls throughout the body, including those in the eye, making them more prone to rupture.
- Diabetes: While not a direct cause, diabetes can affect blood vessels systemically. Diabetic retinopathy, a complication of diabetes, involves damage to the blood vessels in the retina, and systemic vascular changes may contribute to subconjunctival hemorrhages.
- Blood-Clotting Disorders: Conditions that affect the blood's ability to clot properly, such as hemophilia or certain other bleeding disorders, can increase the risk of bleeding from even minor vessel damage.
- Arteriosclerosis: The hardening and narrowing of arteries can affect blood flow and vessel integrity.
- Inflammation of the Conjunctiva (Conjunctivitis): While conjunctivitis itself typically causes redness due to inflammation, severe cases or associated rubbing could potentially lead to a hemorrhage.
- Tumors of the Conjunctiva: Though rare, growths on the conjunctiva can sometimes be associated with bleeding.
Medications
- Blood Thinners: Medications such as aspirin, warfarin (Coumadin), and other anticoagulants or antiplatelet drugs are designed to prevent blood clots. While beneficial for certain conditions, they can increase the risk of bleeding, including subconjunctival hemorrhages.
Other Factors
- Aging: As people age, blood vessel walls can naturally become more fragile, potentially increasing the risk of rupture.
- Childbirth: The intense straining involved during childbirth can cause increased pressure that leads to subconjunctival hemorrhages.
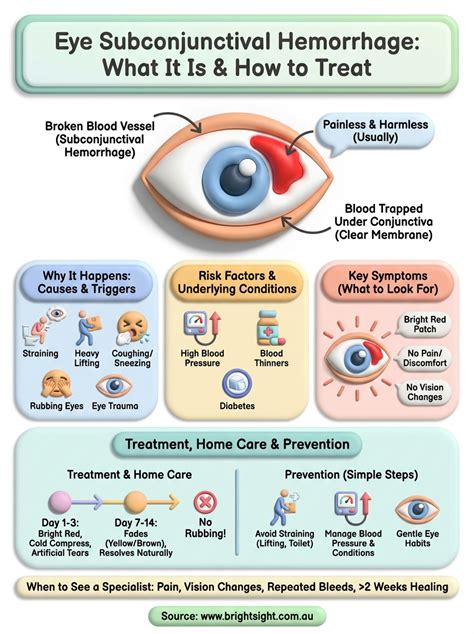
Symptoms of Subconjunctival Hemorrhage
The primary and often only symptom of a subconjunctival hemorrhage is the sudden appearance of a bright red patch on the white of the eye. This patch can vary in size, from a small speck to a larger area covering a significant portion of the sclera.Key characteristics of the symptoms include:
- Appearance: A distinct, flat, bright red area on the white part of the eye.
- Onset: Often noticed upon waking up in the morning or after a straining event.
- Pain: Typically, there is no pain associated with a subconjunctival hemorrhage. If pain is present, it may indicate a different, more serious eye condition.
- Vision Changes: Vision is usually unaffected. A subconjunctival hemorrhage does not typically cause blurred vision, light sensitivity, or vision loss. If these symptoms occur, medical evaluation is necessary.
- Sensation: Some individuals may feel a sensation as if something is in their eye, or a feeling of fullness or grittiness, especially as the eyelid moves over the affected area. This is not always present.
- Discharge: There is usually no eye discharge.
- Unilateral: Most often, the hemorrhage occurs in only one eye.
Diagnosis of Subconjunctival Hemorrhage
A healthcare provider can typically diagnose a subconjunctival hemorrhage based on a visual examination of the eye. The characteristic red patch on the white of the eye is usually sufficient for diagnosis.
During the diagnostic process, a healthcare provider may:
- Ask about Health History: Inquire about recent activities, potential injuries, existing medical conditions (like high blood pressure or diabetes), and medications being taken, especially blood thinners.
- Perform a Physical Exam: This includes a basic eye examination to confirm the presence of the hemorrhage and rule out other causes of red eye.
- Use a Lighted Microscope (Slit Lamp): An ophthalmologist or optometrist may use a specialized microscope to examine the eye in greater detail, particularly if there was a significant eye injury or if the hemorrhage is recurrent. This helps determine if the injury involves deeper structures of the eye.
- Order Blood Tests: If subconjunctival hemorrhages occur repeatedly, or if there is suspicion of a bleeding disorder, blood tests may be ordered to check blood clotting factors.
It is important to differentiate a subconjunctival hemorrhage from other causes of red eye, such as infections (conjunctivitis), inflammation (uveitis), or more serious conditions like acute glaucoma or corneal ulcers, which may involve pain, discharge, or vision changes.
Treatment and Home Care
In the vast majority of cases, a subconjunctival hemorrhage requires no specific medical treatment. The condition is self-limiting and resolves on its own as the body gradually reabsorbs the pooled blood.
Expected Healing Process
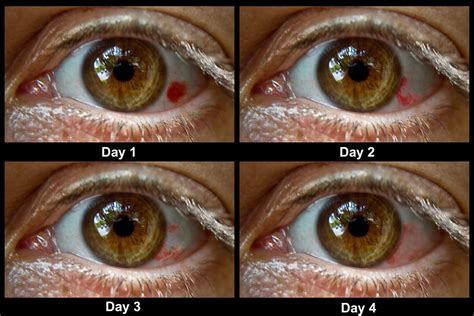
- Duration: The red patch typically disappears within 2 to 3 weeks.
- Color Changes: As the blood is reabsorbed, the red color will gradually change. This process is similar to how a bruise on the skin heals, progressing through shades of brown, purple, and eventually fading to yellow before disappearing completely.
- No Speeding Up: There are no medical treatments or interventions that can significantly speed up the absorption of the blood.
Home Care Recommendations
- Avoid Rubbing the Eyes: Refrain from rubbing the affected eye, as this can potentially worsen the bleeding or delay healing.
- Artificial Tears: Over-the-counter artificial tears eye drops can be used to help lubricate the eye and relieve any minor irritation or dryness. Ensure they are sterile and preservative-free if used frequently.
- Cold Compresses: Applying a clean, cool (not frozen) compress to the closed eye during the first 24-48 hours may help reduce any mild inflammation or discomfort, though this is not always necessary.
- Avoid Contact Lenses: If you wear contact lenses, it is advisable to discontinue their use until the hemorrhage has completely resolved to prevent further irritation.
- Pain Relief: If pain is present due to another reason, acetaminophen (Tylenol) can be used for relief. Avoid aspirin and products containing aspirin, as they can increase bleeding. Do not take multiple pain medications simultaneously without consulting a doctor.
When to Contact a Healthcare Provider
While usually harmless, there are specific circumstances when you should seek medical attention for a red spot on the eye:- Persistent Hemorrhage: If the red patch does not show signs of healing or disappear within 2 to 3 weeks.
- Recurrent Hemorrhages: Experiencing multiple subconjunctival hemorrhages, especially without a clear precipitating event, may indicate an underlying health issue that needs investigation.
- Eye Injury: If the hemorrhage occurred following a significant eye injury, it is crucial to have the eye examined by a healthcare professional to rule out deeper damage.
- Pain: The presence of eye pain, severe discomfort, or pain that worsens with eye movement is a red flag and warrants immediate medical evaluation.
- Vision Changes: Any alterations in vision, such as blurred vision, flashes of light, new floaters, shadows in peripheral vision, or loss of eyesight, require urgent medical attention.
- Signs of Infection: If there is any yellow or greenish discharge from the eye, increased sensitivity to light, or significant swelling.
- Systemic Symptoms: If the red eye is accompanied by other symptoms like headache, nausea, vomiting, or fever, it could indicate a more serious underlying condition.
- Taking Blood Thinners: If you are on anticoagulant or antiplatelet medication and experience a subconjunctival hemorrhage, it's advisable to inform your healthcare provider.
A healthcare provider's evaluation is essential to confirm the diagnosis, rule out more serious conditions, and address any underlying causes if necessary.