Dry skin in the ears, characterized by flakiness, can be a source of discomfort and irritation. This condition can manifest in various ways, from mild dryness of the outer ear to more severe issues like skin loss, soreness, and even infection of both the external and internal parts of the ear. The affected areas can include the earlobes, the conchal bowl (the bowl-shaped area of the outer ear), the ear opening (meatus), the ear canal (external auditory canal), and even the eardrum (tympanic membrane).
Understanding the underlying causes is crucial for effective treatment and prevention of flare-ups. It is always advisable to consult a doctor if you suspect you have a condition affecting your ear skin.
Common Causes of Dry and Flaky Ear Skin
Several factors can contribute to dry, flaky skin in and around the ears. These range from environmental influences and lifestyle choices to specific skin conditions.
Skin Conditions
Various dermatological conditions can lead to dryness and flakiness in the ears:
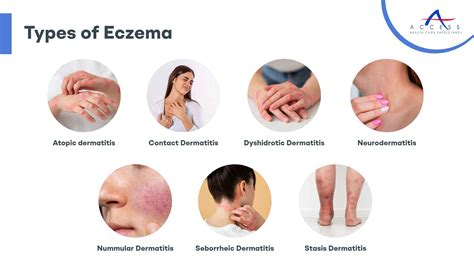
- Eczema (Atopic Dermatitis): This is a common cause of dry, itchy, and red or darker-than-usual skin, particularly in people with a history of eczema. It frequently affects the ears and the skin behind them. A common site is the junction between the earlobe and the face, which can develop painful cracks (fissures) that are prone to infection. Ear eczema can also affect the ear canal and extend to the eardrum.
- Asteatotic Eczema: This form of eczema tends to affect older individuals. The exposed ear is vulnerable to weather and temperature changes, leading to dry, scaly, and itchy skin.
- Seborrhoeic Dermatitis: This condition is thought to be an overreaction of the skin's immune system to an overgrowth of a common yeast called malassezia. Around the ears, it often manifests as inflammation of the ear canal and the area behind the ear (post-auricular area), potentially causing painful cracks. Treatment typically involves reducing yeast overgrowth with antifungal shampoos and anti-inflammatory creams.
- Contact Dermatitis: This can be either irritant or allergic.
- Irritant Contact Dermatitis: Occurs when the skin's surface is irritated by substances like shampoos, hair gels, hair sprays, perm solutions, hair colorants, and perfumes, leading to dry, itchy, and red or darkened skin.
- Allergic Contact Dermatitis: Develops when the body reacts to a specific allergen. Products used for hair and scalp care, as well as materials in hair accessories like hairpins and grips, can be culprits.
- Psoriasis: This chronic autoimmune disorder causes skin cells to grow too rapidly, leading to thick, discolored patches (plaques) with white or silvery scales. It can affect the outer ear, scalp, and neck, causing dryness and itchiness.
Environmental and Lifestyle Factors
External factors also play a significant role in ear skin health:
- Weather and Temperature: Both hot and cold weather, as well as low humidity, can strip moisture from the skin. Central heating and air conditioning can exacerbate this.
- Sun Exposure: Excessive sun exposure can damage the skin, leading to dryness and scaling.
- Over-cleaning: The ears are self-cleaning and do not require intensive manual cleaning. Over-cleaning can remove essential earwax and natural oils that maintain skin health.
- Harsh Soaps and Cleansers: Products containing alcohol, strong perfumes, or harsh chemicals can strip natural oils, leading to dryness.
- Age: As people age, their skin produces less sebum, making it more susceptible to dryness.
- Heating and Hot Baths/Showers: High temperatures from heating systems or excessive hot water can dry out the skin.
- Wearing Hearing Aids: The material of hearing aids or the friction they cause can irritate sensitive ear skin, leading to dryness.
- Ear Piercings: While ear piercing itself doesn't cause eczema, subsequent reactions to earrings, especially those made of nickel, can lead to dry, crusty skin.
Infections
Otitis Externa (Swimmer's Ear): This is an inflammatory condition of the ear canal, often caused or worsened by moisture. It can be linked to primary skin problems like eczema or bacterial/fungal infections. Symptoms include earache, redness, swelling, itching, and discharge.
Say Goodbye to Swimmer's Ear: Effective Treatment Options
Symptoms of Dry Ear Skin
The symptoms of dry, flaky skin in the ears can vary but commonly include:
- Dryness and flakiness
- Itching, which can be intense
- Redness or a change in skin tone (darker or lighter than usual)
- Soreness or tenderness
- Painful cracks or fissures, especially behind the ear or at the earlobe junction
- Crusting or oozing of fluid (pus) in cases of infection
- Temporary hearing loss due to wax and scale buildup
- A feeling of fullness or blockage in the ear
If dry patches develop crusts, start oozing blood, fluid, or pus, become red, or start hurting, it is important to seek medical advice.
Treatment and Management Strategies
Treatment for dry, flaky ear skin depends on the underlying cause. The primary goals are to relieve itching, restore moisture balance, reduce inflammation, and prevent infection.
General Care and Home Remedies
- Moisturizing: Regular application of emollients, creams, lotions, or ointments is essential to restore and maintain skin moisture. Apply immediately after bathing or showering to lock in hydration. Ointments generally provide a more protective barrier than creams or lotions.
- Gentle Cleansing: Wash the outer ear gently with warm water or an emollient wash. Use a damp cotton bud very gently on the bowl area of the ear, but avoid inserting it into the ear canal.
- Drying: Thoroughly dry the ears after washing, using a warm (not hot) hairdryer on a low setting can be effective.
- Avoiding Irritants: Use mild, fragrance-free soaps and cleansers. Avoid harsh chemicals, perfumes, and alcohol-based products.
- Protecting from Environmental Factors: Wear a hat in cold weather and use sunscreen on exposed ear areas in the sun. Consider using a humidifier in dry indoor environments.
- Managing Scratching: If itching is severe, use a cool compress or an over-the-counter hydrocortisone cream (at least 1%) to reduce inflammation.
- Diet and Hydration: Drink plenty of water to maintain overall skin hydration.
- Earwax Management: For softening earwax, refined petroleum oil (unfragranced baby oil) or sunflower oil can be used after consulting a healthcare professional. Olive oil is not recommended as it can damage the skin barrier.
Medical Treatments
- Topical Steroids: Prescription or over-the-counter steroid creams or ear drops can help reduce inflammation, itching, and swelling. These are usually for short-term use.
- Antifungal Treatments: For seborrhoeic dermatitis, antifungal shampoos and creams may be prescribed to reduce yeast overgrowth.
- Antibiotics: If a bacterial infection is present, antibiotic ear drops or oral medications may be necessary.
- Antifungal and Steroid Combinations: For mixed infections or severe inflammation, a combination preparation may be prescribed.
- Allergen Avoidance: If allergic contact dermatitis is suspected, patch testing may be performed to identify allergens, allowing for avoidance. Hypoallergenic jewelry (made from materials like 18-carat gold, sterling silver, platinum, or surgical stainless steel) should be worn if nickel allergy is confirmed.
- Aural Toilet: This is a procedure performed by healthcare professionals to manually clean the ear canal of debris, wax, and scales, which is particularly helpful for individuals with ear eczema.
- Microsuction: This is a recommended method for removing impacted earwax, considered safer than water-based methods, especially for those with ear eczema.
- Prescription Medications: For severe or persistent conditions like psoriasis or eczema, stronger prescription creams, ointments, or other medications may be required.
It is important to consult a healthcare professional for a proper diagnosis and treatment plan, especially if home remedies are ineffective or if symptoms worsen.
Preventing Dry and Flaky Ear Skin
Preventative measures focus on maintaining skin hydration and avoiding triggers:
- Incorporate ears into your daily moisturizing routine.
- Protect your ears from extreme temperatures and harsh weather.
- Use a humidifier in dry environments.
- Opt for mild, moisturizing soaps and cleansers.
- Avoid hot showers and baths; opt for lukewarm water.
- Consider bathing less frequently to preserve natural oils.
- Wear cotton or silk clothing that is less likely to irritate sensitive skin.
- If you have sensitive skin or allergies, be mindful of the materials in jewelry and personal care products.
- Use earplugs when swimming to prevent water from entering the ear canal.