Drug rashes, also known as drug eruptions or cutaneous drug reactions (CDRs), are skin reactions that occur when the body responds adversely to a medication. These reactions can range from mild discomfort to life-threatening conditions. While any medication can potentially cause a rash, certain classes are more commonly associated with these side effects.
What are Drug Rashes?
Drug rashes are the body's reaction to a certain medicine. The type of rash that happens depends on the medicine causing it and your individual response. Medicines have been linked to every type of rash, from mild to life-threatening. The timing of the rash can also vary, sometimes appearing hours after taking a drug, while in other cases, it may take weeks to develop. Even a small amount of a medicine can cause a significant reaction in the skin, and these reactions can occur even after a medication has been taken for a long time.
Drug hypersensitivity is an exaggerated immune response to a medication, which may not necessarily involve a true allergy. These reactions encompass a broad range of responses to medications. Drug rashes are typically symmetric, meaning they appear the same on both sides of the body. While some drug rashes may be accompanied by itching or tenderness, they often do not cause other systemic symptoms. However, if you develop a rash after starting a new drug, it's important to consider the medication as a potential cause.
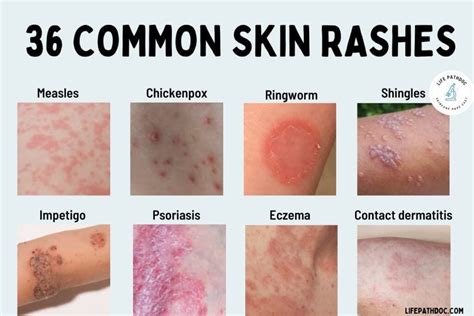
Causes of Drug Rashes
Drug rashes can occur for several reasons, including:
- An allergic reaction to a medication.
- A buildup of the drug in the body, leading to toxicity in the skin.
- A drug making the skin more sensitive to sunlight (photosensitivity).
- Interaction between two or more drugs.
In some cases, drug rashes can be idiopathic, meaning there is no known direct cause. Certain personal risk factors may increase the likelihood of developing a drug rash, such as being older, being female, having a viral infection concurrently with antibiotic use, or having a weakened immune system due to an underlying condition or other medications. Cancer can also be a contributing factor.
Common Types of Drug Rashes
There are several types of drug rashes, each with distinct characteristics:
Exanthematous Rashes
Considered the most common type, accounting for about 90 percent of cases. These rashes may present as small, raised or flat lesions on reddened skin. In some instances, the lesions can blister and fill with pus. Possible causes include penicillins, sulfa drugs, cephalosporins, antiseizure drugs, and allopurinol.
Urticarial Rashes (Hives)
The second most common type, characterized by small, pale red bumps that can merge to form larger, itchy patches. Medications known to cause urticarial rashes include NSAIDs, ACE inhibitors, antibiotics (especially penicillin), and general anesthetics.
Photosensitivity Reactions
These reactions are worsened by sun exposure. Certain drugs increase skin sensitivity to ultraviolet light, leading to an itchy sunburn if unprotected. Examples of such drugs include certain antibiotics (like tetracyclines), sulfa drugs, antifungals, antihistamines, retinoids (e.g., isotretinoin), statins, diuretics, and some NSAIDs.
Erythroderma
A potentially life-threatening condition where nearly the entire skin becomes itchy and red, potentially developing scales within days. Symptoms may include fever and hot-to-the-touch skin. Drugs like sulfa drugs, penicillins, antiseizure drugs, chloroquine, allopurinol, and isoniazid can cause erythroderma. This condition requires immediate medical attention.
Stevens-Johnson Syndrome (SJS) and Toxic Epidermal Necrolysis (TEN)
These are serious, potentially life-threatening reactions that can develop into each other. SJS involves less than 10% of the body's skin surface, while TEN affects more than 30%. Both are marked by large, painful blisters and can cause the top layer of skin to peel off, leaving raw, open sores. Potential drug-related causes include sulfa drugs, antiseizure drugs, some NSAIDs, and nevirapine. These conditions require immediate medical attention.
Anticoagulant-Induced Skin Necrosis
Certain blood thinners, such as warfarin, can lead to this condition, initially causing red and painful skin, progressing to tissue death beneath the skin. The risk is higher at the start of a high dose of a new blood thinner. This is a serious reaction requiring immediate medical attention.
Drug Reaction with Eosinophilia and Systemic Symptoms (DRESS)
A rare but potentially life-threatening drug rash that may not appear for 2 to 6 weeks after starting a new drug. The rash is typically red, often starting on the face and upper body, and is accompanied by severe symptoms affecting internal organs, such as fever, swollen lymph nodes, facial swelling, burning pain, itchy skin, flu-like symptoms, and organ damage. Possible culprits include anticonvulsants, allopurinol, abacavir, minocycline, sulfasalazine, and proton pump inhibitors. DRESS requires immediate medical attention.
Adderall and Skin Reactions
Adderall, a prescription medication for ADHD and narcolepsy, is a central nervous system stimulant containing amphetamine salts. While effective for its intended uses, Adderall can cause various side effects, including those affecting the skin. These can manifest as:
- Acne: A common skin condition characterized by pimples, blackheads, and whiteheads, which may be exacerbated in some individuals taking Adderall.
- Skin Dryness: Stimulant medications can lead to dehydration, causing the skin to feel rough, flaky, or tight. Staying hydrated and using moisturizers can help.
- Skin Rash: Rashes, varying from small red bumps to larger raised patches, can be a sign of a potential allergic reaction to Adderall.
- Skin Sensitivity: Some individuals may experience increased skin sensitivity, making their skin more prone to discomfort or irritation.
- Stevens-Johnson Syndrome (SJS): As mentioned earlier, SJS is a rare but severe reaction reported with Adderall use.
Skin sores, though less common, have also been reported with Adderall use, potentially linked to SJS or secondary factors like nutritional deficiencies due to decreased appetite. Pruritus, or itching, is another reported side effect, which can be caused by skin dryness, allergic reactions, or psychological factors.
Your Brain On Adderall
Diagnosis of Drug Rashes
Diagnosing a drug rash can be complicated. A healthcare provider will typically start with a thorough review of all prescription and over-the-counter medications the patient is taking. The timing of the rash in relation to starting a new medication is a crucial factor. If a specific medication is suspected, the provider may advise the patient to stop taking it to see if the reaction subsides. In some cases, a substitute medication may be prescribed. If the drug is essential for life, the provider might suggest continuing it to see if the rash resolves on its own or with treatment.
Figuring out the exact cause isn't always easy, as symptoms can mimic other conditions. Diagnostic tests may include:
- Skin Biopsy: A small sample of affected skin is examined under a microscope, especially for severe or unusual reactions.
- Skin Tests: Small amounts of potential allergens are applied to the skin to check for reactions like swelling or redness.
- Blood Tests: These can check for specific antibodies, such as IgE, that indicate an allergic response.
If a medication is identified as the cause, it's crucial to avoid it in the future. If the patient has had a severe reaction, a doctor might advise against reintroducing the medication, as it could be hazardous.
Treatment of Drug Rashes
The primary treatment for a drug rash is to stop taking the medication that is causing the reaction. The condition usually clears up once the offending drug is discontinued. However, the timeline for resolution can vary depending on the type and severity of the rash, often taking one to two weeks to disappear completely.
For mild reactions, treatments may include:
- Antihistamines: To help alleviate itching and reduce the severity of the rash.
- Topical Corticosteroids: Creams or ointments like hydrocortisone can reduce inflammation and itching.
For more serious drug rashes, additional treatments might be necessary:
- Anti-inflammatory Drugs: May be prescribed to control symptoms.
- Corticosteroids (Oral or Intravenous): Used for more severe reactions to reduce inflammation and suppress the immune response.
- Epinephrine (Adrenaline): Administered in emergency situations like anaphylaxis to counteract severe allergic reactions.
- Immunomodulators: These drugs suppress the immune response causing the allergic reaction.
- Supportive Care: For severe conditions like SJS/TEN, treatment may involve managing wounds as if they were extensive burns, including pain management and skin grafts. Hospitalization is often required.
Cool showers can provide temporary relief from itching. Avoiding scratching is important to prevent further skin damage or infection. Wearing loose-fitting clothing made from breathable materials can minimize irritation.

If you suspect you have a drug rash, it is essential to consult your doctor right away. Never stop taking prescribed drugs without discussing it with a healthcare professional first, especially if you are taking multiple medications. For severe reactions, seek immediate emergency medical attention at an urgent care clinic or hospital.