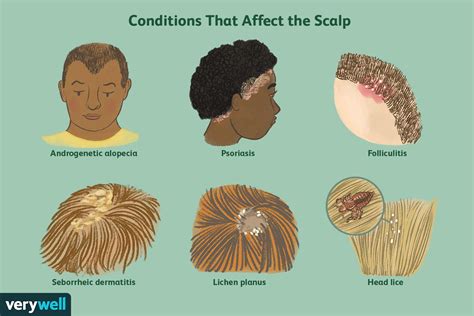
Seborrhoeic dermatitis is a prevalent scaly rash that commonly affects the scalp, face, and chest, though it can extend to other body areas. The term 'dermatitis' is synonymous with 'eczema,' and 'seborrhoeic' indicates its presence in areas rich in sebaceous (oil-producing) glands, such as the scalp and the sides of the nose. This information specifically addresses seborrhoeic dermatitis in adults, a condition affecting approximately 4% of the adult population, with a higher prevalence in men than women.
Despite its association with oily skin areas and the development of greasy-looking scales, seborrhoeic dermatitis is not caused by oily skin. Similar to other forms of eczema, the skin in individuals with seborrhoeic dermatitis is typically dry. The prevailing theory is that adult seborrhoeic dermatitis results from an inflammatory response to an overgrowth of normal skin inhabitants, specifically Malassezia yeasts (such as Malassezia furfur, also known as Pityrosporum ovale).
This condition is neither contagious nor related to diet. However, it can be exacerbated by factors such as illness, stress, fatigue, seasonal changes, and a general decline in health. It's also worth noting that psoriasis, another common skin condition, frequently coexists with seborrhoeic dermatitis. Psoriasis often leads to a very scaly scalp, with an estimated 80% of sufferers experiencing some scalp involvement. The irritation caused by seborrhoeic dermatitis can worsen psoriasis, creating a challenging condition that may not resolve until the seborrhoeic dermatitis component is managed. This combination is sometimes referred to as 'sebo-psoriasis'.
Once the skin becomes inflamed due to any form of eczema, exposure to detergents, soaps, shampoos, and similar products can further aggravate the condition. This exposure can significantly contribute to the worsening and persistence of seborrhoeic dermatitis. Many common skin irritants can exacerbate the condition.
Common Sites and Appearance of Seborrheic Dermatitis
The most frequent locations for seborrhoeic dermatitis include the scalp, eyebrows, forehead, the creases around the nose and cheeks, ears, the front of the chest, the area between the shoulder blades, and skin flexures (folds). In individuals with lighter skin tones, the affected skin appears scaly and faintly red. For people of color, the affected areas are scaly and may be lighter or darker than the surrounding skin, potentially without any redness. In darker skin tones, the scaling can sometimes form a flower-like pattern.
Dandruff is also a common accompanying symptom, with its severity varying. In flexural areas like the armpits or groin, scaling may be absent, and the skin might appear slightly more glazed. On more exposed areas, the scale can become quite pronounced and yellowish. Seborrhoeic dermatitis may or may not be itchy, and its intensity can fluctuate daily.
Specific Areas Affected:
- Scalp: Can range from mild flaking (dandruff) to inflamed, scaly patches that may occasionally weep.
- Face: Typically affects the skin around the sides of the nose and in the creases, sometimes extending to the cheeks. The skin may appear red, or lighter or darker than the surrounding skin (depending on skin tone), and will be scaly. The inner half of the eyebrows can develop 'dandruff'.
- Ears: Seborrhoeic dermatitis can manifest around the ears. Eczema may also occur within the ear canal (otitis externa), on the earlobe, or behind the ears.
Diagnosis and Management of Seborrheic Dermatitis
The diagnosis of seborrhoeic dermatitis is typically made based on the patient's history and the visual appearance of the affected skin. Usually, no specific tests are required unless a doctor suspects a fungal infection, in which case skin scrapings may be taken for mycology testing.
Seborrhoeic dermatitis cannot be cured because individuals may develop a sensitivity to Malassezia on the skin, leading to recurring issues upon exposure. The primary method for managing the condition is through anti-yeast treatments, which help suppress symptoms without eradicating the underlying cause. Fortunately, seborrhoeic dermatitis is usually manageable with topical treatments that are safe for long-term use under the guidance of a healthcare professional.
Moisturizing and Treating the Scalp with Seborrheic Dermatitis
Maintaining a healthy scalp is crucial for healthy hair, much like soil is essential for flowers. Dryness, irritation, itching, and scaling are common symptoms that indicate a compromised scalp. Several factors can contribute to a dry scalp, including environmental influences like indoor heating and cold weather, overwashing, and the use of hot hair tools, all of which can strip the skin of its natural oils. Medical conditions such as psoriasis, eczema, fungal infections, and seborrheic dermatitis are also significant contributors to scalp dryness. Allergies, dehydration, and malnutrition can further exacerbate these issues.
The tell-tale signs of a dry scalp include itching, irritation, and scaling. Differentiating a dry scalp from dandruff is important; a dry scalp typically presents with smaller flakes and may be accompanied by oiliness on the skin or within the hair. Feelings of tightness and redness can also indicate scalp dryness.

Key Strategies for Moisturizing and Managing a Dry Scalp:
1. Adjusting Your Shampoo Schedule
The optimal frequency for washing hair varies depending on hair thickness and texture, the amount of styling products used, physical activity levels, sweat production, scalp oil production, and the surrounding environment. Daily washing is often unnecessary. The recommended frequency can range from every other day for thinner hair or those with excessive oil production to weekly for thicker, coarser hair types. This can be adjusted based on individual needs.
It is also advisable to avoid using hot water during hair washing, as high temperatures can dry out the hair. Lukewarm to cool water is recommended.
2. Avoiding Drying Ingredients in Hair Products
Certain cleansing agents can strip the scalp of its natural moisture. It is recommended to avoid sulfates and harsh surfactants in shampoos. Sodium chloride and fragrances can also dry out the skin and sensitize the scalp. Short-chain alcohols, such as isopropyl and ethanol, can dry out the scalp by evaporating quickly and drawing moisture away from the skin. These are often found in dry shampoos and hairsprays and should be used sparingly.
3. Opting for Moisturizing Ingredients
Using products with moisturizing ingredients is a direct way to combat scalp dryness. Look for humectants that attract and retain water, such as glycerin, niacinamide, hyaluronic acid, and panthenol. These ingredients help the scalp lock in moisture.
Some recommended products include Dove Scalp + Hair Hydrating Shampoo and Conditioner, which contain vitamin B3 and vitamin E to balance sebum production and hydrate the skin, and Head and Shoulders Daily Moisture Scalp Cream, which contains coconut oil for scalp nourishment. JooY Soothing Scalp Serum is also recommended for its hydrating ingredients like algae, aloe vera, and tea tree oil, along with fermented blueberry for inflammation.
4. Utilizing Hydrating Oils
Oils can be rich in vitamins and nutrients to address dryness. Jojoba oil, with its high vitamin E concentration, can protect against oxidative damage. Argan oil, containing fatty acids, squalene, and vitamin E, adds moisture to the scalp and hair. Rose water oil may offer soothing and anti-inflammatory properties. Coconut oil, rich in essential fatty acids, hydrates and restores the scalp's barrier.
Important Consideration: If you have scalp conditions like dandruff or seborrheic dermatitis, oils might exacerbate these issues. It is crucial to consult with a dermatologist before using oils on your scalp.
5. Massage and Exfoliation
Massaging the scalp can significantly contribute to scalp moisturization by improving blood flow, which is beneficial for healthy skin and hair growth. Gentle scalp exfoliation can also help remove buildup that contributes to dryness. Tools like scalp massagers can be used during shampooing for this purpose.

6. Exploring Scalp Treatments
Specialized scalp treatments are available at salons and spas, including steam treatments and intensive conditioning options. The Hydrafacial Keravive is an intensive in-office treatment that uses suction to remove dead skin cells and buildup, followed by the infusion of nourishing ingredients.
Specific Treatments for Seborrheic Dermatitis
For seborrhoeic dermatitis affecting the scalp, the primary treatments involve medicated shampoos, creams, and lotions. Anti-yeast or antifungal medications, such as ciclopirox or ketoconazole shampoos, are often prescribed. These shampoos are typically used two to three times a week, left on the scalp for 5 to 10 minutes, and then followed by a regular shampoo and conditioner.
Over-the-counter (OTC) shampoos containing antifungal ingredients like zinc pyrithione and selenium sulfide can help combat Malassezia overgrowth. It is important to avoid using prescription and OTC dandruff shampoos simultaneously, as this can lead to excessive dryness.
Exfoliating ingredients like salicylic acid can aid in removing scales, but they should not be the sole treatment. For facial seborrhoeic dermatitis, topical medications like ketoconazole or steroid creams may be prescribed and should be applied to clean, dry skin. It's advisable to simplify your skincare routine to avoid irritating sensitive skin and interfering with medication effectiveness.
Mild topical steroids can be used for short-term bursts to address inflammation, but once irritation subsides, relying on anti-yeast agents is recommended. For severe or extensive cases, oral anti-yeast treatments may be necessary.
Medicated Shampoos and Scalp Applications:
- Anti-yeast shampoos: Contain active ingredients like ketoconazole, ciclopirox, zinc pyrithione, or selenium sulfide. Examples include shampoos with 5% tea tree oil.
- Tar-based shampoos: Can help manage flaking and scaling symptoms.
- De-scaling agents: Such as salicylic acid, may be used in conjunction with shampoos for very scaly scalps.
- Scalp applications/lotions: Containing steroids and salicylic acid may be prescribed for severe cases.
Topical Treatments for Other Areas:
- Anti-yeast creams or ointments: Such as clotrimazole, miconazole, and nystatin, are generally effective and safe for long-term use on areas other than the scalp.
- Mild topical steroids: For short-term use on the face and other affected areas.

Oils and Their Role in Seborrheic Dermatitis Management
Some individuals find that topical oils can provide relief from symptoms like itchy, dry, flaky skin, and inflamed scalps. However, it's crucial to understand that while some oils may be beneficial, others can aggravate the condition and should be avoided on sensitive skin.
Potentially Beneficial Oils:
- Tea Tree Oil: Known for its antifungal properties, it can help control Malassezia yeast overgrowth. It should be used in a diluted form, as it can irritate sensitive skin. Shampoos with 5% tea tree oil can be applied to the scalp.
- CBD Oil: Research suggests it may reduce scalp inflammation by interacting with the body's endocannabinoid system, potentially regulating the skin barrier, immune response, and sebaceous glands.
- Mineral Oil: Effective in retaining moisture and can be used to loosen scales, particularly in cases of cradle cap.
- Coconut Oil: Contains lipids with anti-inflammatory and antimicrobial properties. However, some research indicates it might promote the growth of Malassezia yeast, so caution and patch testing are advised.
- Jojoba Oil: Rich in vitamin E, it can protect against oxidative damage.
- Argan Oil: Contains fatty acids, squalene, and vitamin E to moisturize the scalp.
Oils to Avoid with Seborrheic Dermatitis:
- Olive Oil: Some studies suggest it may damage the skin barrier when applied directly to the skin.
- Oils with Synthetic Fragrance: Lab-made compounds can irritate sensitive skin or cause allergic reactions.
- Oils with Preservatives: Chemicals like parabens and formaldehyde can aggravate sensitive skin and worsen symptoms.
When considering any new oil or product, a patch test on a small area of affected skin is recommended. If an adverse reaction occurs, discontinue use immediately and consult a doctor.
Lifestyle and Home Remedies
Lifestyle changes and home remedies can play a role in managing seborrhoeic dermatitis. Regular scalp washing with appropriate shampoos is essential. If regular shampoos are ineffective for dandruff, try nonprescription dandruff shampoos. Medicated shampoos can be used daily or several times a week initially, then reduced to weekly or bi-weekly for maintenance. Alternating between different types of shampoos may be necessary if one loses effectiveness.
Softening and removing scales can be achieved by applying mineral oil, peanut oil, or olive oil to the scalp for a few hours before washing. Washing the skin regularly with warm, gentle soap or a non-soap cleanser is also important. Applying a medicated cream, such as a mild corticosteroid, to affected areas (avoiding the eyes) can help. Avoid styling products and skin/hair products containing alcohol.
For facial hair, shampooing regularly with a product like 1% ketoconazole shampoo can be beneficial, especially under mustaches and beards. Gentle cleaning of inflamed or scaly eyelids with diluted baby shampoo and a cotton swab may also be necessary.
For infants with mild cradle cap, washing the scalp daily with a mild baby shampoo and gently loosening scales is recommended. If scaling persists, applying mineral or olive oil for a period before washing can help.
While alternative therapies like tea tree oil and aloe vera gel have been reported to help some individuals, scientific evidence for their effectiveness is not always conclusive. It is always best to consult with a healthcare provider or dermatologist for personalized advice and treatment plans.
Dermatologist Explains Dandruff: What Causes it & Best Dandruff Treatments! | Dr. Sam Ellis
tags: #how #to #moisturize #scalp #with #seborrheic