Hydrocolloid blemish patches have emerged as a popular and effective solution for managing various types of blemishes. These small, adhesive stickers are designed to cover individual spots, utilizing a special gel called hydrocolloid to immediately improve their appearance upon application.
What Are Hydrocolloid Patches?
In essence, pimple patches are tiny, adhesive stickers formulated to target specific blemishes. Their primary function is to unclog pores and absorb excess fluid, accelerate wound healing, and crucially, prevent the user from picking at the skin. While pimple patches come in various formulations with different ingredients tailored for specific breakouts, hydrocolloid acne patches are among the most popular.
Hydrocolloid patches are a type of wound dressing that works by retaining moisture, thereby creating a moist healing environment ideal for pimples, burns, or other lesions. These patches are composed of a water-attracting material bonded to a very thin plastic film. When applied to an open pimple, for instance, they have the ability to draw out pus.
Although hydrocolloid dressings have been utilized in wound care since the 1960s (with their initial development dating back to the 1930s by a dentist), it was not until the early 2010s that pimple patches began appearing on skincare and beauty shelves.

How Do Hydrocolloid Patches Work?
When a hydrocolloid patch is applied to an inflamed pimple, typically one containing fluid, the warmth of the skin softens the patch's lining. This allows it to absorb impurities and fluid from the blemish. Simultaneously, the patch acts as a protective barrier, shielding the affected area from further irritation or the spread of bacteria.
The visible presence of an icky white substance on the underside of a removed patch is a combination of the hydrocolloid gel and the excess oils and fluids pulled from the skin. This reaction is a key indicator of the patch's effectiveness in drawing out impurities.
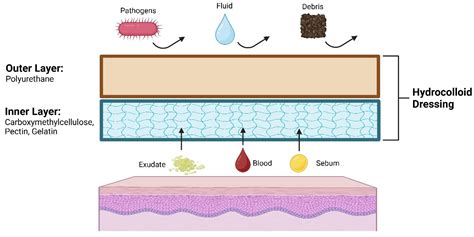
The core mechanism of a hydrocolloid dressing lies in its interaction with the skin environment. These dressings contain gel-forming agents, such as carboxymethylcellulose and pectin, integrated into an adhesive matrix. Upon application to a wound or acne lesion, the hydrocolloid material absorbs exudate or sebum, initiating a gel-forming reaction. This gel creates and maintains a moist environment, which is crucial for supporting autolytic debridement and promoting cellular regeneration. The healing benefits of hydrocolloid acne and wound dressings are directly linked to their moisture-controlling properties. A moist wound environment has been scientifically proven to accelerate healing compared to traditional dry dressings. This dual-action mechanism not only maintains optimal hydration at the wound surface but also prevents maceration of the surrounding skin.
Hydrocolloid dressings are employed in both clinical wound care and personal skincare routines. In healthcare settings, they are often chosen for wounds with low to moderate exudate, such as pressure ulcers, minor burns, and surgical sites. Within the skincare market, hydrocolloid acne dressings and hydrocolloid pimple dressings are increasingly favored for their discreet and effective treatment of blemishes.
Hydrocolloid acne dressings are typically clear, enabling users to wear them throughout the day. The performance of a hydrocolloid patch is significantly influenced by the choice of materials and design features. Usually, the hydrocolloid layer is supported by a polyurethane film, nonwoven material, or a thin foam. Compared to gauze or basic film dressings, hydrocolloid dressings offer superior moisture control, longer wear times, and reduced frequency of dressing changes. They also tend to be more comfortable and less likely to cause secondary damage upon removal. Unlike some film dressings that can dry out a wound or allow excessive vapor loss, hydrocolloid dressings actively modulate moisture levels. In acne management, hydrocolloid pimple dressings often outperform topical creams in terms of protecting the lesion and managing inflammation.
The Science Behind Hydrocolloid Patches
Hydrocolloids are fundamentally moisture-retentive dressings. They retain water to create an effective insulating environment that aids the wound-healing process. By doing so, they facilitate the action of the body's natural enzymes in healing the skin.
Typically, hydrocolloid bandages contain gel-forming agents like sodium carboxymethyl cellulose and gelatin. They may also include pectin and hydrophobic pressure-sensitive polymers such as polyisobutylene.
Hydrocolloid patches are available in various shapes and sizes to address different types of wounds, ranging from burns and scrapes to acne blemishes. These products are engineered to be more absorbent than other dressings, meaning they help absorb any discharge from uninfected wounds without drying them out, thus allowing for healing.
When applied to a wound, sticky-side down, the hydrocolloid gel absorbs any drainage and protects the wound from further trauma, such as picking, thereby supporting healing. The patches then remove impurities, leading to the gel-like substance that adheres to the dressing.
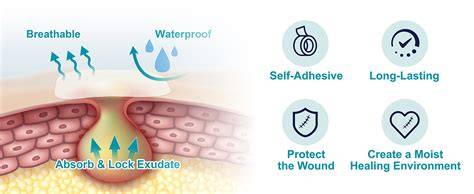
Hydrocolloid dressings for wounds and burns usually feature a backing of either a vapor-permeable film or a thin foam sheet. This backing has a gel-like layer on one side, composed of a mixture of sodium carboxymethyl cellulose, elastomers, adhesives, and gelling agents. Once the dressing is applied to an injury, the warmth of the skin softens the bandage's lining, creating a gel cover that helps absorb discharge or fluid from the wound. When the dressing reaches its saturation point, known as strike-through, it should be changed. Because strike-through can occur relatively quickly, hydrocolloid dressings are best suited for:
- Wounds with low to moderate fluid discharge
- Granular wounds (moist cuts or burns with red, bumpy skin)
- Minor burns
Most hydrocolloid dressings come in various shapes and often include an additional adhesive border to help prevent leakage or keep the dressing from sliding. It is important to note that hydrocolloid patches should not be used on infected wounds.
Do Pimple Patches Actually Work?
Yes, hydrocolloid patches are generally considered effective, particularly for certain types of blemishes. They work by absorbing drainage from pimples and covering the wound to prevent further trauma, making them effective at protecting open and active pimples.
However, they are not typically effective for treating cystic acne and blackheads. While they help treat surface-level blemishes like whiteheads, they do not prevent outbreaks of acne blemishes and are not suitable for cystic pimples or blackheads.
Studies have compared hydrocolloid pimple patches with surgical tape on individuals with mild to moderate acne. After changing their patch or tape every two days for a week, both groups showed a reduction in acne severity. However, the pimple patch group demonstrated superior results in making acne less severe, filtering out more UV radiation (which helps prevent skin cancer and melanoma), and controlling redness, oiliness, dark pigmentation, and sebum on specific days of the study. Researchers also found that hydrocolloid patches made with gelatin and cortex extracts aided in quicker skin cell healing due to their antibacterial properties, outperforming other commercial non-hydrocolloid acne patches.
Other over-the-counter acne patches may contain ingredients like tea tree oil and have a single layer. Unlike hydrocolloid patches, these cannot absorb fluid from the blemish, which could lead to the pimple reappearing.
Specific Product Features: CeraVe Blemish Barrier Patches
CeraVe Blemish Barrier Patches are highlighted as a unique offering in the market. They are the first and only hydrocolloid blemish patches formulated with three essential ceramides and niacinamide. Developed in collaboration with dermatologists, these patches aim to provide clinically proven results by soothing the skin and immediately reducing the appearance of all types of blemishes upon application.
These patches are designed to absorb oil in as little as 3 hours and help protect the delicate skin barrier, thereby decreasing the risk of developing post-blemish marks. The formula is described as ultra-thin, nearly invisible on all skin tones, and features a seamless tapered design for discreet and secure wear, whether day or night.
Consumer feedback indicates high satisfaction: 95% of users reported that their skin did not look irritated after patch removal, with no marks left behind, and 96% agreed the patch felt gentle on the skin.
Application and Best Practices
Correct application is crucial for the optimal performance of hydrocolloid dressings. Before applying a patch, it is essential to clean the affected area thoroughly. Hydrocolloids seal in whatever is beneath them, so starting with a clean surface is vital. The area should also be dried completely, as patches will not adhere effectively to damp skin.
While it is always best to avoid popping pimples, if a blemish does rupture, a hydrocolloid patch can assist in healing the open wound.
Some skincare products enhance their patches with acne-fighting ingredients like tea tree oil or niacinamide. It is advisable to be aware of these additions, especially if you have sensitive skin or known allergies.
To remove a hydrocolloid patch, gently peel it slowly from the edges, stretching it along the skin rather than pulling upwards, to minimize stress on the surrounding skin.
When Not to Use Hydrocolloid Patches
While generally safe and effective, there are situations where hydrocolloid patches may not be suitable. If you have oily skin, the patch might not adhere as well, although this is typically not a major issue. Additionally, individuals with more melanin-rich skin tones might consider avoiding daytime use, as UV exposure could potentially lead to hyperpigmentation where the patch was applied.
Hydrocolloid patches are not recommended for infected wounds. If you have sensitive skin, it is advisable to consult a healthcare professional before use, as the adhesives could potentially cause irritation for some individuals.
Furthermore, hydrocolloid patches are not effective for treating dirt from clogged pores, blackheads, or whiteheads. They are also not effective for cystic acne and cannot prevent future flare-ups.
Frequently Asked Questions
How Often Can You Use Pimple Patches?
According to most dermatologists, pimple patches can be used as needed. They can be worn during the day or overnight.
Do Pimple Patches Work on Unpopped Pimples?
Pimple patches are most effective on fluid-filled zits, such as papules and pustules. While they help treat surface-level blemishes like whiteheads, they do not prevent outbreaks of acne blemishes and do not treat cystic pimples or blackheads.
Can Pimple Patches Help Reduce Acne Scars?
If you have a habit of picking at your skin, pimple patches can help reduce acne scars by preventing further picking and promoting a better healing environment. Applying a patch to a blemish that has not been properly cleaned can trap bacteria and oil, potentially leading to scarring.
Can a Hydrocolloid Bandage Make Acne Blemishes Worse?
Pimple patches are designed to help heal blemishes and should not worsen your acne. However, if you have sensitive skin, it's wise to seek medical advice first, as the adhesives might irritate some individuals.
Can I Use a Hydrocolloid Bandage If Iâve Already Popped My Pimple?
While it is always best to avoid popping a pimple, a pimple patch can be beneficial if you do. The patch will help protect the open wound and promote healing.
tags: #hydrocolloid #blemish #patch