Do you have patches of thick, hard skin on your feet? If so, you may be experiencing hyperkeratosis. This is a common condition characterized by the excessive thickening of the outer layer of the skin. The overgrowth of keratin, a tough, fibrous protein essential for skin protection, can lead to various foot problems.
Keratin overgrowth most frequently affects the bottom of the foot, known as the plantar surface. When this excess keratin builds up, it can result in plantar hyperkeratosis, a condition where the thickened skin becomes hard and cracked. This can be painful and may impede walking.
To prevent plantar hyperkeratosis, it is important to manage any excessive keratin growth. Regular exfoliation and consistent moisturizing of the feet can help.
Understanding Hyperkeratosis
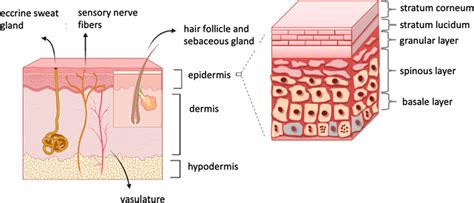
Hyperkeratosis is essentially the hardening and thickening of the skin in response to stimuli such as pressure, friction, or other irritants. This is the skin’s natural defense mechanism to protect itself from further damage. While the skin is your body’s primary protection, excessively thick areas can cause significant problems, particularly for your feet.
Causes of Hyperkeratosis
Hyperkeratosis typically occurs when the skin is subjected to excessive pressure, rubbing, or irritation. Common causes include:
- Wearing tight or ill-fitting shoes that rub and pinch the feet.
- Walking barefoot on hard surfaces.
- Standing for extended periods.
- Foot conditions such as flat feet or bunions that alter weight distribution and create pressure points.
- Dry skin.
- Certain health conditions, including diabetes, eczema, psoriasis, arthritis, or obesity, which can increase the skin's susceptibility to thickening.
- In some cases, hyperkeratosis can have a genetic predisposition.
Abnormal mechanical stresses on the skin can result from intrinsic factors like bony prominences or deformities such as hammertoes, or extrinsic factors like tight shoes or irregularities within footwear. These stresses lead to the accumulation of multiple layers in the horny layer of the epidermis, a process known as hyperkeratosis.
Non-pressure-related hyperkeratosis occurs when the skin thickens due to a medical condition that damages the skin, such as autoimmune disorders or genetic diseases.
Types of Hyperkeratosis
Hyperkeratosis can manifest in various ways depending on the cause and location. Some common types include:
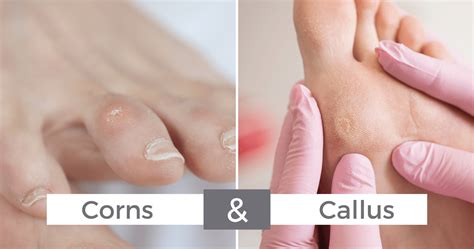
Calluses and Corns
Plantar hyperkeratosis can lead to the development of calluses and corns, which often appear on pressure points.
- Calluses are hardened, thickened areas of skin that lack a well-defined border and are typically yellowish or brown. They form on areas of the body experiencing repeated friction or pressure, commonly on the hands and feet.
- Corns are smaller, more concentrated outgrowths of hard skin, often featuring a tough keratin plug at the center. They can appear on the soles of the feet (seed corns) or on the tops or sides of the toes. Corns can be painful, especially when shoes exert pressure on them.
Plantar hyperkeratotic lesions like calluses and corns are particularly common among mature adults. The aging process reduces skin suppleness and cushioning, making it more prone to these lesions. It is estimated that 30-65% of people over 65 are affected by them.
Women frequently develop calluses and corns from wearing high heels or other constrictive footwear, which can be quite painful. Choosing comfortable footwear that does not place unnecessary strain on the feet is advisable.
Other Forms of Hyperkeratosis
- Clavus: A painful, localized form of hyperkeratosis resembling a small bump or lesion, often caused by pressure from tight shoes or bony areas of the foot.
- Epidermolytic Hyperkeratosis: A very rare, genetic form causing scaly, thick skin across various body parts, including the feet, typically appearing at birth or in early childhood.
- Lichen Simplex Chronicus: Resulting from frequent scratching or rubbing, this leads to thick, itchy patches of skin, often linked to ongoing skin irritation or stress.
- Actinic Keratosis (Solar Keratosis): Caused by skin damage from the sun, this is a common type that can become cancerous if left untreated.
- Hyperkeratosis of the Nipple and Areola: Causes thickening of the skin in these areas, resembling warts, most often affecting teenage girls. The cause is unknown.
- Keratosis Pilaris (Follicular Hyperkeratosis): Small, scaly plugs of keratin block hair follicles, causing bumpy or rough skin, commonly on the upper arms, thighs, and buttocks. It is believed to be genetic.
- Lichen Planus: An autoimmune disorder, believed to be genetic, causing purplish, itchy, flat bumps on the skin.
- Psoriasis: An autoimmune skin disease characterized by thick, silvery, itchy, and uncomfortable plaques on the skin.
- Retention Hyperkeratosis: Skin cells that normally shed do not, remaining on the skin and sticking together, leading to acne.
- Seborrheic Keratosis: Common, harmless skin growths that typically appear in people over 50. Sudden, rapid appearance may indicate a more serious underlying issue.
- Subungual Hyperkeratosis (Hyperkeratosis of the Nail): A symptom of nail psoriasis, resulting in a chalky substance under the nails.
- Warts: Caused by a virus, leading to skin thickening and bump formation. Warts are contagious.
Symptoms of Hyperkeratosis
The symptoms of hyperkeratosis are generally straightforward, and most do not cause pain. However, corns and calluses can become painful due to their location, often on the feet. Noticeable symptoms include:
- Rough patches of skin.
- Bumps.
- Changes in skin color (yellowish, brownish, or sometimes purplish bruising under a callus indicating a blood blister).
The appearance of hyperkeratosis varies greatly depending on the specific form, location, and skin tone. It can present as a rash, small bumps, pimples, or larger raised lesions. For individuals with lighter skin, rashes might appear as reddened areas, while darker skin tones may show noticeable differences in color (darker, lighter, purple, or gray).
Severe hyperkeratosis can be debilitating. Feet may appear covered in corns and calluses with deep cracks, making the skin susceptible to infection. In such cases, walking can become uncomfortable, potentially leading to a limp. Individuals with excessively thick skin may also experience difficulties sensing changes in temperature and terrain and might take longer to notice foot injuries or infections.
Diagnosis and When to See a Doctor
Diagnosing hyperkeratosis involves a medical history, physical examination, and sometimes a biopsy. Your doctor will inquire about your symptoms, their duration, family history, medications, allergies, and any other medical conditions. A thorough physical examination of the entire skin surface may be necessary.
You should consult a doctor if:
- Thickened skin becomes painful, cracked, or starts bleeding.
- Home care treatments do not improve the condition.
- The affected area appears red, swollen, or infected.
- Walking becomes difficult.
- You suspect an underlying health issue like diabetes, poor circulation, or foot structure problems.
A foot specialist can accurately identify the cause of hyperkeratosis and recommend the most appropriate treatment plan.
Treatment Options for Hyperkeratosis
Treatment for hyperkeratosis depends on the severity and the underlying cause. Options range from home remedies to clinical interventions.
Home Remedies
For mild cases of hyperkeratosis, home care can be effective:
- Soak your feet: Immerse your feet in warm water to soften the thickened skin.
- Exfoliate gently: Use a pumice stone or a gentle exfoliant to remove dead skin cells. Avoid aggressive scrubbing that could break the skin.
- Moisturize regularly: Apply a good moisturizer, especially one containing ingredients like salicylic acid or urea, to keep the skin smooth and hydrated.
- Wear comfortable footwear: Choose shoes that fit well, provide adequate support, and have a roomy toe box.
- Use protective padding: Soft pads or insoles can reduce pressure on sensitive areas.
Clinical Treatment
If home remedies are insufficient, a healthcare professional can offer more advanced treatments:
- Prescription creams: Stronger topical medications can help soften and reduce thick skin.
- Custom shoe inserts (orthotics): These can redistribute pressure and correct underlying biomechanical issues.
- Medicated patches and gels: Available for corns and calluses, but should be used with caution, especially by individuals with diabetes.
- Sharp debridement: A podiatrist or foot specialist can safely shave away thick skin using a scalpel or rotary file to provide immediate relief. This is often a temporary solution if the underlying cause is not addressed.
- Chemical treatments: Acids or other medications may be applied to lesions to help remove them.
- Surgical procedures: In severe or persistent cases, surgery may be considered to correct underlying deformities or remove problematic lesions.
- Oral medications: For certain types of hyperkeratosis, oral medications like retinoids, methotrexate, or immunosuppressants may be prescribed.
- Injected medications: Steroids or biologics may be used for aggressive inflammatory conditions like psoriasis.
- Dermatologic treatments: These can include laser therapy, LED light therapy, shave removal, chemical peels, cryotherapy (freezing), and trimming of excess skin by trained professionals.
A biopsy may be performed to help health professionals reach an accurate diagnosis, especially if the cause is unclear or if severe hyperkeratosis is suspected.
Preventing Hyperkeratosis
Preventing hyperkeratosis involves consistent foot care and making informed choices about footwear:
- Wear well-fitting shoes: Opt for low-heeled shoes with soft uppers and a roomy toe box. For deformities like hammertoes, shoes with extra depth may be necessary.
- Protect your feet: Avoid walking barefoot on hard surfaces, especially in public areas like gyms or locker rooms.
- Moisturize daily: Keep your feet hydrated, particularly after bathing or showering.
- Use protective padding: Apply soft pads to areas that experience increased pressure.
- Trim toenails properly: Incorrect trimming can lead to added stress on the feet.
- Check your feet regularly: Early detection of thick skin or other changes allows for timely intervention.
- Protect from the sun: Use sunscreen (SPF 30 or higher) when exposed to the sun to reduce the risk of actinic keratosis.
- Manage underlying conditions: Effectively treating conditions like diabetes, eczema, or psoriasis can help prevent related hyperkeratosis.
Prognosis
The outcome for hyperkeratosis depends on the specific type and its underlying cause. Warts, corns, and calluses can often be treated successfully and may not return, though recurrence is possible. Actinic keratosis can progress to squamous cell carcinoma if untreated. Psoriasis and eczema are chronic conditions that can be managed with treatment but may not be curable. Genetic or autoimmune forms of hyperkeratosis may not be preventable and can be progressive.
tags: #hyperkeratosis #of #the #foot