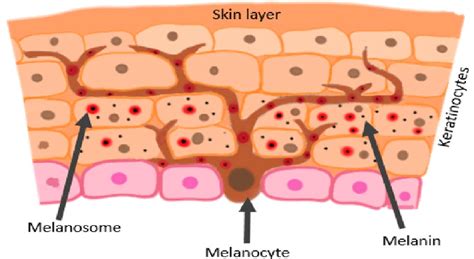
Your skin's color is determined by a pigment called melanin, which is produced by specialized cells known as melanocytes. Vitiligo is a skin condition characterized by the appearance of white patches on the skin, resulting from the absence of melanocytes in those specific areas. While the exact causes of vitiligo remain unknown, some dermatologists hypothesize that it may stem from an autoimmune disease where the immune system mistakenly attacks melanocytes. Melasma, on the other hand, presents as brown patches, primarily on the face. Dermatologists aim to treat pigment disorders by reversing or minimizing the differences in melanin production that lead to skin discoloration. For vitiligo, this might involve stimulating melanocyte regrowth, while for melasma, treatments focus on reducing pigment production by melanocytes. Various therapies, including light or laser treatments and bleaching creams, can be employed to manage these pigment disorders.
What is Vitiligo?
Vitiligo, pronounced "vit-il-EYE-go," is a skin condition that leads to a loss of skin color or pigment. This results in lighter-colored skin or complete white patches. Areas of skin that lose pigment are classified as macules if they are less than 1 centimeter wide, or patches if they are larger than 1 centimeter. If vitiligo affects areas with hair, such as on the scalp, the hair in those regions may turn white or silver.
The condition arises when the body's immune system destroys melanocytes, the skin cells responsible for producing melanin, the pigment that gives skin its color.
Who is Affected by Vitiligo?
Vitiligo affects all races and sexes equally, though it is more noticeable in individuals with darker skin tones. While vitiligo can manifest at any age, macules or patches typically become apparent before the age of 30. Individuals with certain autoimmune conditions may have a higher risk of developing vitiligo.
How Common is Vitiligo?
Vitiligo affects over 1% of the global population.
Progression and Onset of Vitiligo
Vitiligo typically begins with a few small white macules or patches that may gradually spread across the body. It commonly starts on the hands, forearms, feet, and face, but can appear anywhere, including mucous membranes (the moist linings of the mouth, nose, genital, and rectal areas), eyes, and inner ears.
While larger patches may continue to widen and spread, they often remain in the same location for years. The size and position of smaller macules can shift over time as areas of skin lose and regain pigment.

Vitiligo and the Risk of Skin Cancer
A common concern among vitiligo patients is an increased risk of skin cancer due to the lack of melanin, which normally provides protection against the sun's harmful rays. However, research studies have not consistently supported this warning.
While it seems logical that reduced pigmentation would increase skin cancer risk, some experts have observed a surprisingly low incidence of skin cancer in vitiligo patients. In fact, some studies suggest that vitiligo patients may even have a lower risk of skin cancer compared to healthy individuals. This phenomenon is not fully understood, but genetic research indicates that certain genes associated with an increased risk of vitiligo may simultaneously decrease the risk of melanoma, and vice versa.
One theory is that because vitiligo involves an overactive immune system that attacks normal melanocytes, it might also be effective at clearing abnormal melanocytes that could develop into melanoma. There are even reports of melanoma patients experiencing spontaneous remission of their cancer concurrently with the development of vitiligo. Furthermore, new melanoma treatments that boost the immune response against tumors can also trigger vitiligo, further suggesting a protective role for vitiligo against melanoma.
Despite these findings, it is crucial to emphasize that having vitiligo does not eliminate the possibility of developing skin cancer. Sun protection remains essential for all individuals, including those with vitiligo.
Vitiligo | Immunology | Fusion Animation
Melasma and Other Pigment Disorders
Melasma is a distinct pigment disorder characterized by brown patches on the face. Treatment for pigment disorders generally aims to reverse or minimize the factors causing skin discoloration. For melasma, this involves treatments designed to reduce the amount of pigment produced by melanocytes.
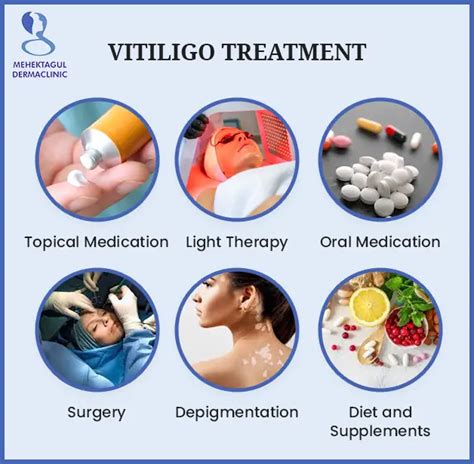
Treatments for Pigment Disorders
A variety of therapeutic approaches can address pigment disorders. These include:
- Light or Laser Therapies: These treatments use specific wavelengths of light or lasers to target pigment-producing cells.
- Bleaching Creams: Topical agents that help to lighten the skin by reducing melanin production.
Treating Vitiligo
For vitiligo, dermatologists may employ treatments aimed at stimulating melanocyte regrowth. Current treatment options focus on managing symptoms and improving cosmetic appearance. These include:
- Topical Corticosteroids: Creams applied to affected skin can help restore color, particularly in the early stages of vitiligo. Side effects may include skin thinning.
- Calcineurin Inhibitors: Ointments like tacrolimus or pimecrolimus can be effective for depigmentation, especially on the face and neck. However, there is a potential warning regarding a link to lymphoma and skin cancer.
- Janus Kinase (JAK) Inhibitors: Medications like ruxolitinib block specific enzymes in the immune system that attack melanocytes. This class of drugs has been approved to help restore skin color.
- Light Therapy (Phototherapy): Narrowband ultraviolet B (UVB) phototherapy can help stop or slow the progression of active vitiligo and may be more effective when combined with corticosteroids or calcineurin inhibitors. Treatments are typically administered two to three times a week, with visible results taking several months. Portable devices are also available for home use.
- Psoralen Plus Light Therapy (Photochemotherapy): This involves taking psoralen (a plant-derived substance) orally or applying it topically, followed by exposure to ultraviolet A (UVA) light. While effective, it is often more complex to administer and has been largely replaced by narrowband UVB therapy.
- Depigmentation Therapy: For widespread vitiligo where other treatments have failed, a depigmenting agent can be applied to unaffected skin to gradually lighten it, blending it with the discolored areas. This is a permanent treatment.
Surgical Options for Vitiligo
For individuals with stable vitiligo that has not responded to other treatments, surgical options may be considered:
- Skin Grafting: Small sections of healthy, pigmented skin are transferred to depigmented areas. This is often used for smaller patches.
- Blister Grafting: Blisters are created on pigmented skin, and the tops of these blisters are transplanted to discolored areas.
- Cellular Suspension Transplant: Pigmented skin cells are harvested, suspended in a solution, and then transplanted onto the prepared affected area. Repigmentation can be observed within four weeks.
Emerging Treatments
Research is ongoing for new treatments, including:
- Afamelanotide: A potential treatment implanted under the skin to promote melanocyte growth.
- Prostaglandin E2: Being tested as a topical gel to restore skin color, particularly for non-widespread or non-spreading vitiligo.
Managing Vitiligo: Sun Protection and Concealment
Due to the loss of pigment, skin affected by vitiligo is particularly susceptible to sunburn. Therefore, it is essential to:
- Protect Skin from the Sun: Seek shade, use broad-spectrum sunscreen with an SPF of at least 30, and wear protective clothing, including hats. Avoid tanning beds and sunlamps.
- Conceal Affected Skin: Makeup and self-tanning products can help minimize the appearance of skin color differences.
It is important to note that damage to the skin, such as from a tattoo, may trigger the appearance of new vitiligo patches.
Coping with Vitiligo
The changes in appearance caused by vitiligo can significantly impact a person's self-esteem, leading to feelings of stress, self-consciousness, and frustration. Seeking support and understanding is crucial:
- Connect with Healthcare Providers: Find a dermatologist experienced in managing skin pigmentation disorders and openly discuss concerns about how vitiligo affects your life.
- Educate Yourself: Learn as much as possible about vitiligo and available treatment options to actively participate in decision-making.
- Communicate Feelings: Inform your healthcare provider if you experience depression or emotional distress. A referral to a mental health professional specializing in dermatology-related issues may be beneficial.
- Seek Support Groups: Connect with others who have vitiligo through support groups or psychotherapy.
- Confide in Loved Ones: Share your feelings and experiences with family and friends to gain understanding and support.