Winter weather can be tough on the skin, and your lips are no exception. The combination of cold air outside and dry indoor heating can strip moisture from your lips, leaving them cracked, peeling, and irritated. Unlike the rest of your skin, lips lack oil glands, making them more vulnerable to dehydration and environmental damage. If you’ve ever experienced chronic dry lips, you’re not alone. While many people reach for lip balm as a quick fix, understanding the root causes of chapped lips and how to properly treat them can help you achieve long-term relief.
What Are Chapped Lips?
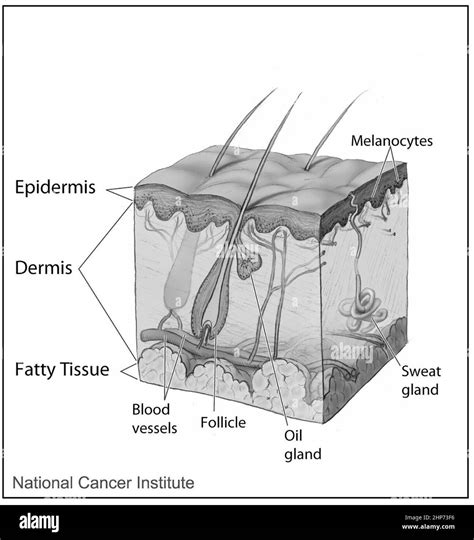
Chapped lips, also known as cheilitis, refer to lips that are dry, cracked, or peeling due to moisture loss. This condition is especially common in colder months but can also occur due to dehydration, sun exposure, or irritating lip products. Because the skin on your lips is thinner and more delicate than other areas, it is more prone to environmental damage. Unlike other parts of your body, lips do not contain sebaceous (oil) glands, meaning they cannot produce their own moisture. This is why external hydration and protection are crucial for maintaining smooth, healthy lips.
Symptoms of Chapped Lips
- Dryness or tightness
- Visible cracks or fissures
- Flaking or peeling skin
- Tenderness or irritation
- In severe cases, bleeding or sores
If left untreated, chapped lips can worsen, leading to painful cracks that may even increase the risk of infection.
Major Causes of Chapped Lips
Chapped lips can develop for several reasons, often due to a combination of environmental, lifestyle, and health-related factors. Understanding the root causes can help you prevent and effectively treat this common concern.
Environmental Factors
Cold Weather & Dry Air
During winter, the humidity levels drop both outdoors and indoors due to heating systems. This lack of moisture in the air leads to increased evaporation from the skin, including the lips, making them dry, flaky, and more prone to cracking. Freezing temperatures, increased wind speeds, and indoor heating are all culprits.
Sun Exposure
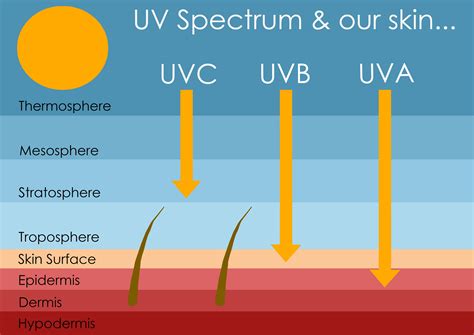
Many people associate sunburn with summer, but UV rays can damage your lips even in winter. Lips lack melanin (the pigment that protects the skin from sun damage), making them more vulnerable to sunburn, which can cause peeling, inflammation, and long-term dryness. Chronic sun exposure can lead to a precancerous condition called actinic cheilitis, which typically presents as dry, flaky patches on the lower lip.
Lifestyle and Habits
Frequent Lip Licking
It’s common to lick your lips when they feel dry, but this habit actually worsens the problem. Saliva evaporates quickly, leaving lips drier than before. Additionally, the digestive enzymes in saliva can break down the delicate skin on the lips, leading to irritation and peeling. Experts advise against excessive licking and picking at the lips.
Dehydration
If your body is not getting enough water, your lips are often one of the first places to show signs of dehydration. Lack of adequate hydration reduces the body’s ability to maintain moisture, leading to persistent dryness. Drinking enough water is essential for overall skin hydration.
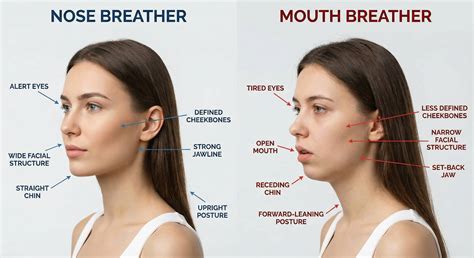
Breathing Through Your Mouth
Chronic mouth breathing, often due to nasal congestion, allergies, or sleep apnea, can dry out the lips quickly. This is especially common at night when airflow continuously passes over the lips, leading to morning dryness and peeling. Using a humidifier can help mitigate this effect.
Irritating Products and Ingredients
Irritating Lip Products
Certain lip balms, lipsticks, or matte liquid lip products may contain drying or irritating ingredients. These can include:
- Menthol, camphor, and eucalyptus - These may feel soothing initially but can irritate the skin over time.
- Fragrances and artificial flavors - Some scented lip products can cause an allergic reaction or further dryness.
- Matte lipsticks - These often have a drying formula that pulls moisture away from the lips.
It's also important to be aware of potential irritation from everyday skincare products, especially those containing acids or strong active ingredients, which can inadvertently get on the lips and cause dryness.
Allergies and Contact Dermatitis
Irritation can also stem from an allergy to pigments in lipsticks, fragrances, or flavoring agents found in foods. This is known as contact cheilitis. Women are more often affected due to the frequent use of lip cosmetics. If you suspect an allergy, a dermatologist can perform patch testing to identify the culprit.
Health-Related Factors
Vitamin Deficiencies
Lack of certain vitamins, particularly B vitamins (B2, B6, B12) and iron, can lead to dry, cracked lips. Vitamin B2 (riboflavin) deficiency is especially linked to cheilitis, a condition where lips become inflamed and cracked at the corners.
Certain Medications
Some medications contribute to dryness as a side effect. These include:
- Accutane (Isotretinoin) - A common acne medication that severely reduces oil production.
- Antihistamines - Used for allergies, but they dry out mucous membranes, including the lips.
- Diuretics - Prescribed for high blood pressure, these medications reduce water retention and can contribute to dehydration.

Treatments and Prevention for Chapped Lips
Treating chapped lips is important, but prevention is the key to keeping them soft, smooth, and hydrated year-round. By making simple adjustments to your daily routine, you can protect your lips from common irritants and avoid the discomfort of dryness and cracking.
Daily Care and Protection
Apply a Protective Lip Balm Daily
Using a moisturizing, ointment-based lip balm throughout the day helps create a barrier against environmental damage. Look for formulas containing petrolatum, shea butter, and ceramides to keep moisture locked in. For added protection, choose a lip balm with SPF 30 or higher to shield against UV rays, which can cause sunburn and long-term dryness. Apply lip balm before going outdoors as a preventative measure.
Stay Hydrated Throughout the Day
Drinking enough water is essential for skin hydration, including your lips. When the body is dehydrated, the lips are often one of the first areas to show signs of dryness. Aim for at least eight glasses of water per day, and include hydrating foods like watermelon, cucumbers, and oranges in your diet.
Protect Your Lips in Harsh Weather
Cold wind and dry indoor heating can strip moisture from the lips. To minimize exposure:
- Wear a scarf or mask in cold weather to cover your lips.
- Use a humidifier indoors to add moisture back into the air.
- Apply a thick lip ointment before going outdoors to prevent moisture loss.
Apply Lip Balm Before Bed
Overnight moisture loss is common, especially for those who breathe through their mouths while sleeping. Applying a thick layer of lip balm or petroleum jelly before bed helps keep lips hydrated and prevents them from drying out overnight. Using a lip ointment at night will keep your lips hydrated throughout the night.

Gentle Exfoliation
Gentle exfoliation helps remove dead skin cells and improve moisture absorption. However, only exfoliate when lips are mildly dry, never when they are cracked or bleeding. Use a sugar and honey scrub or a soft toothbrush to buff away flakes, then follow up with a nourishing lip balm. If you see flakes, the first recommendation is to give the skin what it's asking for, which is hydration. After moisturizing the lips, if there are still flakes, you can use gentle sugar scrubs.
Avoid Irritating Ingredients
Certain lip balms and lip products contain ingredients that can actually make chapped lips worse. Avoid those with:
- Menthol, eucalyptus, and camphor
- Artificial fragrances and flavors
- Lanolin
- Waxes
Matte lipsticks also tend to be drying; if wearing lipstick, apply a hydrating balm underneath.
Layering Lip Products
For intense hydration, consider layering your lip products. Start with a formula containing ingredients like hyaluronic acid (to hydrate) and peptides (to strengthen skin), followed by a layer of Vaseline or a thick occlusive balm to seal in the moisture. This technique is sometimes referred to as "slugging" your lips.
Home Remedies for Chapped Lips
If you're looking for natural ways to heal and prevent dry, cracked lips, several home remedies can be very effective by locking in moisture, reducing inflammation, and promoting healing.
1. Honey
Honey is a powerful humectant, meaning it draws moisture into the skin while also providing antibacterial properties to prevent infection. It helps soften dry lips and speeds up healing. Apply a thin layer of raw honey to your lips and let it sit for 10-15 minutes before rinsing or gently dabbing it off.
2. Coconut Oil
Coconut oil is rich in fatty acids that deeply nourish dry lips and reduce inflammation. It acts as a natural emollient, sealing in moisture to prevent further dryness. Dab a small amount onto your lips several times a day, especially before bed.
3. Aloe Vera Gel
Aloe vera is known for its cooling and soothing properties, making it an excellent remedy for irritated or cracked lips. It helps heal minor wounds and reduces redness. Extract fresh aloe vera gel from a leaf and apply a thin layer to your lips, letting it absorb naturally.
4. Shea Butter
Shea butter acts as a moisture barrier, keeping lips soft while also providing anti-inflammatory benefits. It is particularly useful in cold weather, protecting lips from environmental damage. Apply a small amount before going outside or before bed for overnight hydration.
5. Green Tea Bag Compress
Green tea contains antioxidants and polyphenols that help reduce inflammation and promote healing. This remedy is especially beneficial if your lips feel sore or irritated. Steep a green tea bag in warm water, let it cool slightly, then press it gently against your lips for a few minutes.

When to See a Doctor
If dryness persists despite proper care and home remedies, it may be a sign of an underlying issue such as nutrient deficiencies, allergies, or medication side effects. Severely chapped lips that are bleeding frequently or not improving after a week or two of consistent self-care should be evaluated by a healthcare provider or dermatologist. They can provide further investigation or prescribe more advanced treatment options.