While the primary symptoms of influenza, such as fever, body aches, cough, sore throat, and fatigue, are well-known, some individuals may also experience an unexpected skin rash. Although not a hallmark symptom, a rash can occasionally appear as a manifestation of the body's response to the viral infection, high fever, or even secondary infections or medications taken for symptom relief. Understanding the causes, appearance, and management of post-viral rashes, particularly those associated with influenza, is crucial for appropriate care and peace of mind.
The Connection Between Influenza and Rashes
The flu, a common respiratory infection, can present with a range of symptoms from mild to severe. While a rash is not a typical flu symptom, it can occur in certain circumstances. Some viruses, including influenza, can trigger a rash as the immune system actively fights the infection. This occurs due to the immune system's reaction to the virus, leading to inflammation or other responses that manifest on the skin.
Specifically, high fevers associated with the flu can lead to heat rashes, especially if significant sweating occurs during the illness. These heat rashes are generally benign and resolve once the fever subsides. Furthermore, it's important to consider that rashes might arise not from the flu itself, but as a reaction to medications used to alleviate flu symptoms. Common culprits can include antibiotics, if a secondary bacterial infection has developed, or pain relievers like ibuprofen or acetaminophen. If a medication is suspected of causing a rash, it is advisable to discontinue the medication and consult a healthcare provider.
Evidence suggests that certain strains of influenza might lead to rash formation in some individuals. In other instances, a concurrent condition might be the cause of a rash while a person has the flu. For example, a small 2014 case study involving school-aged children indicated that a rash is a possible, though uncommon, symptom of influenza type B. The researchers noted that factors other than the flu, such as a nearby measles outbreak, might have contributed to the rash's onset. An older article from 2011 reported that a rash occurs in approximately 2% of all influenza A cases, potentially among children with or without other accompanying infections or environmental factors.

Understanding Viral Rashes
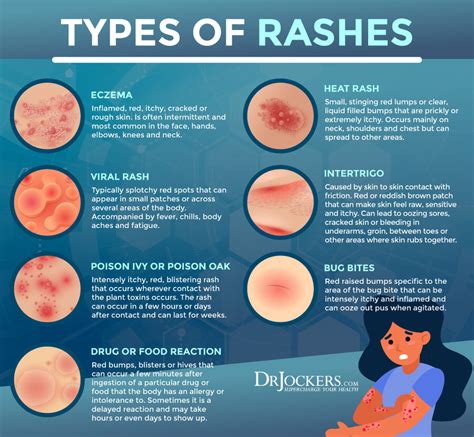
A viral rash, often referred to as a viral exanthem, is an eruption of spots, bumps, or splotches that can accompany various viral infections. The appearance of these rashes can vary significantly. They might present as welts, small bumps, or red, brown, or purple blotches, and can develop on one or multiple areas of the body. For instance, a rash associated with Respiratory Syncytial Virus (RSV) might appear as a maculopapular rash, characterized by a mix of flat and raised discolored spots on the skin.
When flu-like symptoms occur alongside a rash, it's often a sign of the body's generalized immune response to infection or inflammation. The immune system releases inflammatory chemicals called cytokines, which, while helping to fight infection, can also contribute to symptoms like fatigue, aches, and fever, and potentially trigger skin reactions. Red or pink spots that may merge into larger patches are a common presentation. These rashes often appear several days after the initial onset of fever, sore throat, or runny nose, and may begin on the face or chest before spreading.
Common Causes of Rashes with Flu-Like Symptoms
Red bumps appearing with flu-like symptoms can stem from various causes:
- Viral Infections: These are among the most frequent causes. The immune system's reaction to viral particles leads to inflammation in the skin's small blood vessels, resulting in reddish bumps or blotches. Most viral exanthems resolve naturally within a week.
- Bacterial Infections: These can cause localized redness, warmth, and swelling of the skin, often accompanied by fever and body aches. When bacteria enter through a break in the skin, they trigger inflammation. Examples include meningococcal infection, which can present with fever, headache, and purple non-blanching spots. Bacterial infections require antibiotic treatment prescribed by a doctor.
- Allergic Reactions: The immune system can overreact to harmless substances like food, pollen, or medication, leading to the release of histamine. This causes blood vessels in the skin to dilate and leak fluid, resulting in hives. Severe allergic reactions can involve swelling of the face, lips, or throat, and may be accompanied by dizziness or difficulty breathing.
- Medication Sensitivities: Certain medications can trigger immune-mediated skin reactions, sometimes weeks after starting a new drug. These reactions can range from mild rashes to severe, life-threatening conditions. It's crucial to stop the suspected medication and contact a doctor immediately.
- Autoimmune Diseases: In these conditions, the immune system mistakenly attacks the body's own tissues, which can manifest as rashes. Autoimmune rashes typically require long-term management by a healthcare professional.
Recognizing Flu Symptoms
The flu typically presents with several recognizable symptoms. According to the Centers for Disease Control and Prevention (CDC), these include:
- Cough
- Chills
- Fever
- Body aches
- Sore throat
- Fatigue
- Stuffy or runny nose
- Headaches
- Vomiting or diarrhea (more common in children)
In some cases, individuals may develop serious health complications as a result of the flu, such as pneumonia, which can be life-threatening. Other potential complications include worsened asthma symptoms, swelling of heart, brain, or muscle tissues, heart or kidney failure, and extreme inflammatory responses in the body.
Diagnosis and Treatment of Post-Viral Rashes
When flu-like symptoms occur alongside a rash, consulting a doctor is recommended. A healthcare provider will typically conduct a physical examination and inquire about the patient's symptoms. During periods of widespread flu activity, a specific test for the virus may not be necessary. However, if flu is not prevalent, the doctor might test for the type of virus. The doctor can also examine the rash to determine if it is caused by a different condition.
The primary treatment for the flu generally involves rest and adequate fluid intake. For individuals with severe infections or those at risk of complications, antiviral medications prescribed by a doctor may be beneficial. These medications, such as oseltamivir (Tamiflu), baloxavir (Xofluza), zanamivir (Relenza), and peramivir (Rapivab), can help speed recovery and prevent further complications.
If a person has a confirmed case of the flu and a rash, the rash itself may not require direct treatment. It should typically clear as the body successfully fights off the virus. For symptom relief from itching and irritation associated with a rash, using a gentle, fragrance-free moisturizer can help calm dry or irritated skin. Over-the-counter hydrocortisone cream or colloidal oatmeal baths can also provide relief.
Most post-viral rashes are harmless and fade on their own. However, some can be itchy, uncomfortable, or persist. If a rash covers a large area, causes significant discomfort, or is accompanied by a high fever, it is important to seek medical attention. Early care can help reduce the risk of complications and promote a speedier recovery.
Are All Medication Rashes Serious Side Effects?
When to Seek Medical Attention
While most flu-related rashes are not serious and resolve independently, certain signs warrant medical evaluation. Individuals should consult a doctor if their rash covers a significant portion of their body, causes discomfort, or is accompanied by a high fever. Getting care early can help reduce the risk of complications and promote a speedier recovery.
Certain groups are at a higher risk of developing complications from the flu. These include older adults, children under the age of two, pregnant women, and individuals with chronic illnesses such as asthma, diabetes, or heart disease. While most flu cases resolve with rest and fluids, those at risk of complications should seek medical advice.
Immediate medical attention is necessary if experiencing any of the following severe flu symptoms:
- Persistent pain or pressure in the chest or abdomen
- Difficulty breathing or shortness of breath
- Seizures
- Severe muscle pain
- A fever or cough that improves but then returns or worsens
- Persistent confusion or dizziness
- Worsening of chronic medical conditions
- Lack of urination
- Severe weakness or unsteadiness
Parents or caregivers should seek emergency care for a child exhibiting any of the following:
- Bluish lips or face
- Severe muscle pain
- Fast breathing or trouble breathing
- Seizures
- Ribs pulling in with each breath
- Chest pain
- A fever or cough that improves before returning or worsening
- Dehydration (signs include little urine, no tears, and a dry mouth)
- Lack of alertness or inability to interact when awake
- A fever above 104°F (40°C) or any fever in infants under 12 weeks old
- Worsening symptoms of chronic medical conditions
It is important to remember that rashes are rare in lymphoma patients, but if they occur, they are worth discussing with a medical professional. Hodgkin lymphoma, for instance, can sometimes cause a skin rash or itching sensation, appearing in up to 25% of patients at initial diagnosis. This type of rash, or pruritus, may be related to the disease's rapid proliferation and the release of inflammatory markers in the skin. If a rash occurs with lymphoma, it typically appears at the base of the neck, elbows, under the arms, or in the groin area. In some cases, affected skin may thicken, harden, and form itchy, ulcerated plaques, or raised areas of skin (papules) may appear as the lymphoma progresses.
Even after treatment for Hodgkin lymphoma, patients can experience itching or a rash as an early sign of relapse. Medications used in the treatment of Hodgkin lymphoma, such as nivolumab or pembrolizumab, can also sometimes cause skin reactions.
The information provided in this article is for general informational purposes only and does not substitute for professional medical advice, diagnosis, or treatment. Always seek the advice of your physician or other qualified health provider with any questions you may have regarding a medical condition.