The MMR vaccine is a crucial component of childhood immunization, offering protection against three highly contagious diseases: measles, mumps, and rubella. These infections can lead to serious health complications, including meningitis, blindness, and hearing loss. For pregnant individuals, contracting measles can result in premature birth, miscarriage, or stillbirth. The MMR vaccine is administered as part of the NHS vaccination schedule.
MMRV Vaccine: Enhanced Protection
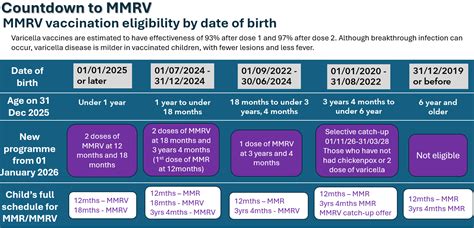
In recent years, children are typically offered the MMRV vaccine, which provides protection against measles, mumps, rubella, and chickenpox (varicella). This combined vaccine is given in two doses, usually at 12 and 18 months of age. The MMRV vaccine has been used for many years in countries such as Australia, Canada, and New Zealand, and has a good safety record.
How the MMR Vaccine Works
The MMR vaccine is a live vaccine, meaning it contains weakened forms of the measles, mumps, and rubella viruses. Your immune system responds by developing cells that recognize and remember these viruses. Should you encounter these diseases in the future, these cells will activate your body to produce antibodies, providing protection.
Two doses of the MMR vaccine are recommended for full protection. After the first dose, most, but not all, individuals develop immunity. Following the second dose, over 99% of people are fully protected against measles and rubella, and approximately 88% are protected against mumps. Immunity gained from two doses is generally considered lifelong.
Potential Side Effects of the MMR Vaccine
Like all medicines, the MMR vaccine can cause side effects, though not everyone experiences them. These are typically mild and short-lived.
Common Side Effects
- Rash: A raised, blotchy rash, similar to a measles rash, may appear around 7 to 11 days after vaccination. This is a common and expected side effect and does not mean your baby has measles. Another type of rash, a spotty rash resembling chickenpox, may appear around the injection site 3 to 4 weeks after the MMRV vaccine. This rash may contain infectious virus and should be covered.
- Fever: A high temperature (fever) can occur, usually around 7 to 11 days after the vaccination, and may last for 2 to 3 days.
- General Malaise: Feeling unwell is another common side effect.
- Swollen Glands: Swollen glands around the cheeks, neck, and jaw, or aching in the joints, similar to a mild form of mumps, can occur around 2 to 3 weeks after the vaccination.
- Injection Site Reactions: Redness, swelling, or soreness at the injection site are also common and usually last for 2 to 3 days.
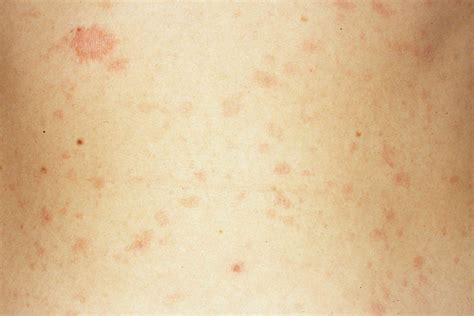
It is important to note that any rash appearing after the MMR vaccine is typically mild and occurs at predictable times. If you are unsure whether a rash is related to the vaccine, it is advisable to consult your doctor or call 111 for advice.
More Serious Side Effects (Rare)
More serious side effects, such as a severe allergic reaction (anaphylaxis), are rare. Fits (seizures) can occur in children with a high temperature, which can be caused by common childhood illnesses, including those following vaccination. These fits are usually brief and do not cause long-term health problems. Swelling in the brain (encephalitis) has been reported extremely rarely after the MMRV vaccination (less than one child in a million). Anaphylactic reactions, which cause breathing difficulties and may lead to collapse, are also extremely rare, affecting less than one in a million people.
If your child develops a fever and feels unwell after vaccination, paracetamol can be administered. It is important to encourage fluid intake, especially breastmilk or water if formula feeding, and avoid over-bundling the child.
Timing of MMR Vaccine Rashes
A rash related to the measles component of the vaccine typically appears about a week to 10 days after immunisation. A rash from the rubella component may appear around 12 to 14 days after vaccination, though rarely, it can appear as late as six weeks later. For the MMRV vaccine, a spotty rash at the injection site may appear 3 to 4 weeks after vaccination.
MMR Vaccine and Specific Concerns
Pregnancy and Breastfeeding
As the MMR vaccine is a live vaccine, it is generally not advised during pregnancy. However, data suggests there are no safety concerns if pregnancy is discovered after vaccination. Breastfeeding mothers can receive the MMR vaccine without harm to themselves or their baby.
Allergies
The MMR vaccine can be safely given to children with a severe allergy to eggs, as it is grown on chick cells, not egg white or yolk. If you have concerns about a severe allergic reaction to gelatine (used in some vaccines) or the antibiotic neomycin (an ingredient in the MMR vaccine), you can request the gelatine-free version of the MMR vaccine from your GP.
Religious Concerns
For individuals who do not consume pork products due to religious beliefs, specific MMR vaccines that do not contain pork gelatine are available. Please consult your health visitor, practice nurse, or GP surgery.
Autism
There is overwhelming scientific evidence that the MMR vaccine does not cause autism. Extensive research has consistently found no link between the MMR vaccine and autism. Past studies that suggested a link have been discredited and retracted.
Measles Vaccine Myths Debunked: What the Science Actually Shows
Catching Up on Missed Vaccinations
If you or your child has missed any MMR-containing vaccinations, it is important to catch up as soon as possible. Your GP surgery can check your vaccination records and arrange for any necessary doses. Catch-up doses can be given at any age. Measles is currently experiencing a significant outbreak in the UK, highlighting the importance of maintaining high vaccination rates.
When to Seek Medical Advice
While most side effects are mild, it is important to seek medical help immediately if:
- Symptoms worsen.
- You are concerned about any side effects.
- You suspect a severe allergic reaction (anaphylaxis).
- Your child develops a rash with red or purple spots that do not fade under pressure (test by pressing a glass against the rash).
- Your child has a high temperature (fever) above 38.5°C, it is advisable to wait until they have recovered before vaccination.
In case of concerns, call NHS 111 or your GP surgery. If you cannot attend a vaccination appointment, please cancel and reschedule as soon as possible. Minor illnesses like a cold are not usually a reason to delay vaccination.