Rheumatoid arthritis (RA) is a chronic autoimmune disease primarily affecting the joints. However, the systemic inflammation associated with RA, as well as the medications used to treat it, can also lead to a variety of skin manifestations, including rashes. It is estimated that approximately 1 in 3 individuals with rheumatoid arthritis may experience RA-related skin issues. While not all skin manifestations are rashes, they can include nodules, sores, nerve problems, and other symptoms.
Types of Rheumatoid Arthritis Rashes and Their Symptoms
The appearance of a rheumatoid arthritis rash can vary significantly depending on the underlying cause. Several skin conditions are associated with RA that can present with rash-like symptoms:
Palmar Erythema (Red Palms)
Palmar erythema, commonly known as "red palms," is a condition that can stem from various health issues. In individuals with RA, it is often a result of an autoimmune response or a side effect of RA medications. Approximately 60% of people with RA experience this condition. Signs include redness of both palms that may extend to the fingers. This redness might be accompanied by a slight feeling of warmth. A characteristic feature is that the redness fades when pressure is applied to the skin. This condition typically develops in individuals who have had severe RA for at least 10 years.
Rheumatoid Vasculitis
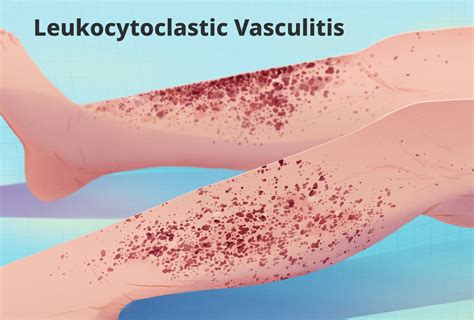
Rheumatoid vasculitis occurs when inflammation causes the small and medium-sized blood vessels to narrow, thereby interfering with blood flow to the skin. This condition affects the entire body, not just the skin. It usually appears as a purplish rash (purpura) on the skin and can manifest as small to large red, brown, or purple dots or patches. In more severe cases, skin ulcers may develop, often on the legs or lower body. The rash is frequently accompanied by a lack of sensation, numbness, or tingling in the affected area. Symptoms of rheumatoid vasculitis can also include enlarged liver or spleen and blood in the urine (hematuria). This condition is considered an emergency, and immediate consultation with a rheumatologist is advised if symptoms appear.
Rheumatoid vasculitis is often seen in individuals who have had RA for a long time (over 10 years) and typically have severe joint damage. Factors such as smoking cigarettes or using tobacco products can increase the risk of developing rheumatoid vasculitis due to blood vessel damage. Other risk factors include having an enlarged spleen and low white blood cell count (Felty syndrome) and the presence of rheumatoid nodules.
Rheumatoid Neutrophilic Dermatitis
Rheumatoid neutrophilic dermatitis is a rare skin condition associated with long-standing RA. It typically presents as raised red, blue, or purple rash-like lesions on both arms and/or legs, though it can also appear on a single limb or the torso. It causes red or skin-colored bumps or patches, usually on the chest, abdomen, or back, but sometimes on the limbs. These patches may change in size or shape over days or months. This condition is usually painless, though some individuals may experience itching or tenderness.
Eczema (Atopic Dermatitis)
Eczema, or atopic dermatitis, is a common skin condition characterized by an intensely itchy, red, or purple rash. While eczema can occur independently of rheumatoid arthritis, studies have indicated a higher prevalence of RA in individuals with atopic dermatitis. Researchers are investigating whether certain forms of eczema are autoimmune diseases.
Sweet's Syndrome and Pyoderma Gangrenosum
Although uncommon, Sweet's syndrome and pyoderma gangrenosum can also cause rashes in individuals with RA. Sweet's syndrome typically presents as a painful, blistering rash with mucosal lesions. Pyoderma gangrenosum causes an ulcerative skin rash with bluish borders and the development of new ulcers following minor skin damage. Both Sweet's syndrome and pyoderma gangrenosum are serious conditions requiring prompt medical intervention.
Cutaneous Vasculitis
A small percentage of individuals with rheumatoid arthritis may develop a specific complication known as cutaneous vasculitis, which is often referred to as rheumatoid vasculitis. This condition usually appears as a purplish rash (purpura) on the skin. In more severe instances, skin ulcers may develop on the legs, often accompanied by a lack of sensation, numbness, or tingling in the affected area.
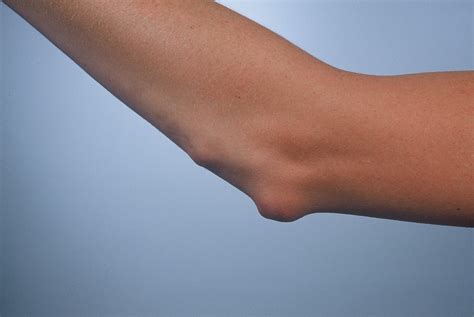
Rheumatoid Nodules
Rheumatoid nodules are not a rash but are hard lumps of tissue that form directly under the skin, typically over bony areas or pressure points such as the elbows, hands, or fingers. They can range in size from that of a pea to a golf ball. About 40% of people with RA will develop rheumatoid nodules at some point. While not a rash, they are a significant skin manifestation of RA and can sometimes be associated with rheumatoid vasculitis.
Livedo Reticularis
Livedo reticularis is a condition characterized by a net-like pattern of red-blue or purplish weblike lines on the skin, resulting from compromised blood flow in the blood vessels. This can appear brown, dark brown, or purple on medium to dark skin tones and may become more evident in colder weather. Livedo reticularis can also be associated with other autoimmune conditions like vasculitis, as well as clotting disorders, vasospasm, infections, drug reactions, cardiovascular disease, and cancer.
Palmar Erythema
Palmar erythema is a condition where the palms of the hands become red. This typically affects the lower part of the palms, and the fingertips may also redden. Inflammation of the small blood vessels in the hands is believed to play a role, although the exact cause is unknown. While it can occur in pregnancy due to hormonal and blood vessel changes, more than half of individuals with RA may experience palmar erythema. It is usually non-itchy and painless, and symptoms may resolve as RA inflammation is controlled. However, certain medications can also cause palmar erythema.
Rheumatoid Papules (Interstitial Granulomatous Dermatitis)
Interstitial granulomatous dermatitis, sometimes referred to as rheumatoid papules, can manifest as red plaques or bumps that closely resemble eczema. This condition is very rare in individuals with RA, tends to affect the trunk and skin folds, and is often asymptomatic, though it can be itchy and painful.
Hives (Urticaria)
Some individuals with RA may experience chronic or recurring hives. These can appear as pink or red patches on lighter skin tones, while on medium to dark skin tones, redness may be less apparent, and the skin may look irritated and inflamed. Skin welts from hives can be similar in color to a person's natural skin tone.
Causes of Rashes in Rheumatoid Arthritis
The development of rashes in individuals with rheumatoid arthritis can be attributed to several factors:
- Autoimmune Processes: In RA, the immune system mistakenly attacks the body's own tissues, leading to widespread inflammation. This dysregulated immune response can affect the skin, causing conditions like eczema, Sweet's syndrome, and pyoderma gangrenosum. These are often classified as neutrophilic dermatoses, where an overload of neutrophils (a type of white blood cell) contributes to inflammation.
- Inflammation of Blood Vessels (Vasculitis): Rheumatoid vasculitis is a direct consequence of RA-related inflammation affecting small and medium-sized blood vessels. This inflammation narrows the vessels, impeding blood flow and leading to skin damage, rashes, and potentially ulcers.
- Medication Side Effects: Many medications used to treat rheumatoid arthritis, such as methotrexate, Humira, celecoxib, sulfasalazine, and others, can cause skin rashes as a side effect. These reactions can range from mild localized rashes at the injection site of biologic medications to more generalized allergic-type reactions.
- Secondary Infections: Medications that suppress the immune system to control RA can leave the skin more vulnerable to infections. Rapidly spreading, bright red rashes accompanied by fever or malaise may indicate infections like cellulitis, a bacterial skin infection.
- Other Autoimmune Conditions: RA can coexist with or increase the risk of other autoimmune conditions that manifest with skin symptoms, such as psoriasis and psoriatic arthritis, which can cause scaly rashes, particularly on the elbows, knuckles, and scalp.
- Sun Sensitivity: Certain RA medications, like methotrexate and TNF inhibitors, can increase sun sensitivity, making the skin more prone to sunburn and rashes upon sun exposure.
- Reactivated Infections: Individuals with RA are at a higher risk of developing shingles (herpes zoster) due to a reactivated chickenpox virus, which can cause a painful rash.
How Rashes Affect Individuals with Rheumatoid Arthritis
RA-related skin rashes can cause significant discomfort and distress. MyRAteam members have reported various issues, including rashes that are painful, itchy, burning, or blistering. The severity of the rash can fluctuate, often worsening during RA flares. The sun can also exacerbate some RA rashes.
Beyond the discomfort, rashes can sometimes be indicative of more serious underlying issues. For instance, rheumatoid vasculitis, if left untreated, can lead to severe skin damage, ulcers, and even gangrene due to compromised blood flow. Systemic vasculitis can affect blood flow to vital organs like the brain or heart, increasing the risk of heart attack or stroke. Therefore, any concerning rash should be promptly evaluated by a healthcare professional.
Treatment for Rheumatoid Arthritis Rashes
The treatment approach for RA-related rashes depends heavily on the specific type of rash, its severity, and the underlying cause. Management often involves addressing the underlying RA condition and directly treating the skin symptoms.
Managing the Underlying RA
For many RA-related rashes, the primary treatment strategy involves effectively managing the rheumatoid arthritis itself. This may include:
- Disease-Modifying Antirheumatic Drugs (DMARDs) and Biologics: These medications help to control the autoimmune response and reduce inflammation, which can, in turn, alleviate skin symptoms.
- Corticosteroids: Oral or topical corticosteroids may be used to reduce inflammation and calm flare-ups, including those affecting the skin. However, long-term use is generally not recommended due to potential side effects.
- Janus Kinase (JAK) Inhibitors: These are often considered when other immunosuppressant drugs are not effective in managing RA symptoms.
Direct Treatment of Rashes
Specific treatments for different types of rashes include:
- Palmar Erythema: If not causing distress, palmar erythema may not require specific treatment. If medication-induced, the doctor might suggest stopping or changing the medication.
- Rheumatoid Vasculitis: Treatment typically focuses on managing the underlying RA. For localized cases affecting fingertips, antibiotic creams and pain control may be prescribed. If the vasculitis is severe or systemic, more aggressive immunosuppressive therapy is usually required.
- Eczema: Minor cases may be treated with topical ointments, while more severe cases might require immunosuppressant drugs and biologics.
- Sweet's Syndrome: Often treated with oral corticosteroids, with topical corticosteroids used in some instances.
- Pyoderma Gangrenosum: Treatment varies based on the rash's advancement, often involving topical corticosteroid ointments, oral anti-inflammatory antibiotics, steroids like prednisone, and in severe cases, surgery.
- Medication Rashes: If a rash is a side effect of medication, the doctor may adjust the dosage or switch to a different drug. Antihistamines or steroids might be prescribed to manage the reaction.
- Ulcers or Slow Wound Healing: Treatment depends on the wound's size, location, and severity, and may include keeping the area clean, using sterile bandages, good nutrition, anti-inflammatory drugs, immunosuppressants, or steroids. Severe cases may require specialized wound care or, rarely, surgery.
2. Vascular events of Acute Inflammation ( Animation )
Over-the-Counter and Prescription Pain Relief
For pain associated with RA rashes, over-the-counter medications like acetaminophen (Tylenol) may be recommended. However, nonsteroidal anti-inflammatory drugs (NSAIDs) such as ibuprofen and naproxen are generally not advised for RA rashes as they can be organ-threatening. For severe pain, prescription pain relievers, including opioids in extreme cases, may be considered.
Preventative Measures and Lifestyle
While there are no permanent solutions to completely prevent RA rashes, several lifestyle measures can be beneficial:
- Sun Protection: Using sunscreen with a high SPF and wearing protective clothing is crucial, especially if taking medications that increase sun sensitivity.
- Healthy Lifestyle: Getting adequate rest, exercising regularly, managing stress through techniques like meditation, and maintaining a balanced diet rich in fruits, vegetables, whole grains, and lean proteins can help manage overall inflammation and support the immune system.
- Smoking Cessation: Quitting smoking is vital, as it is a significant risk factor for developing rheumatoid vasculitis.
- Vaccinations: Discussing vaccination options, such as the shingles vaccine, with a rheumatologist is important for preventing certain infections.
It is crucial for individuals experiencing RA-related rashes to consult with their rheumatologist or dermatologist. Accurate diagnosis is key, and sometimes skin biopsies, blood tests, or allergy tests may be necessary. Open communication with healthcare providers about any new or changing symptoms is essential for effective management and to prevent potential complications.
tags: #rheumatoid #arthritis #and #face #rash