Tinea manuum, also known as ringworm of the hand, is a contagious fungal infection that primarily affects the palms and can spread to the fingers or the back of the hand. The term "tinea" is the technical name for ringworm, a fungal infection characterized by a round or oval rash, while "manuum" refers to the hands.
Understanding Tinea Manuum
Ringworm is a common fungal infection of the skin caused by dermatophyte fungi that have adapted to live on keratin, the hard fibrous protein found in skin and hair. Tinea manuum is one of the many forms of ringworm, which can affect various parts of the body, including the feet (tinea pedis, or athlete's foot), groin (tinea cruris, or jock itch), and scalp (tinea capitis).
Globally, fungal skin infections are estimated to affect more than 650 million people at any time, with ringworm accounting for over half of these cases. Tinea manuum, while less common than athlete's foot, is a significant concern due to its potential for transmission and the discomfort it causes.
Symptoms of Tinea Manuum
The symptoms of tinea manuum can vary depending on the specific fungus causing the infection and the affected area of the hand. Common signs include:
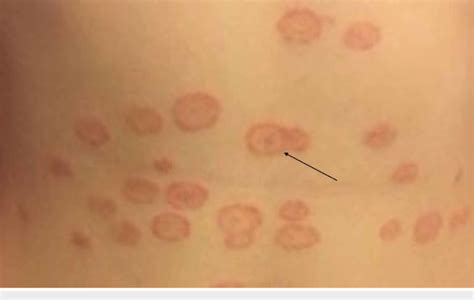
- Itchy, Round Patches: The most common symptom is the appearance of itchy, round patches, often on the back of the hands. On lighter skin tones, these patches may appear red or pink, while on darker skin, they can look brown or gray.
- Ring-like Appearance: These patches can develop into a series of rings or circles with central clearings, a characteristic feature that gives ringworm its name. The rings may have raised, scaly borders.
- Palm Involvement: The skin on the palm of the hands may thicken, leading to intensely dry skin. Deep cracks can form on the palms, sometimes revealing white scaling within them. Itching on the palms may or may not be present, and some individuals may experience pain and swelling.
- Blisters and Pimples: Red patches with blisters and pimples can appear on the skin around the fingers.
- Nail Involvement: Frequently, the infection can spread to the fingernails of the affected hand, causing them to become thick, discolored, and brittle.
- Dry, Peeling, or Scaly Skin: In cases caused by human fungi, a patch of dry, peeling, or scaly skin with mild itching may appear and gradually spread.
- Tiny Blisters: A cluster of tiny blisters might form on the sides of the fingers or on the palm, which may ooze a sticky, clear fluid.
- Itching or Burning: The rash can be mild to moderately itchy, causing discomfort.
- Skin Discoloration: If the rash persists for a long time, the skin may become discolored. This change in color can also occur as the tinea heals.
Causes of Tinea Manuum
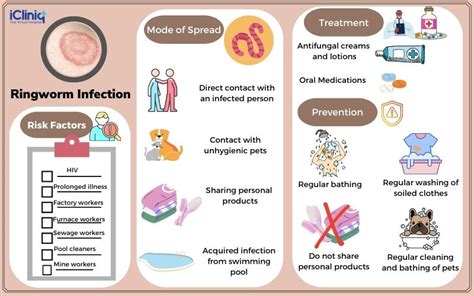
Tinea manuum is caused by a type of fungus known as dermatophytes. These fungi thrive in warm, humid environments and are commonly found in tropical regions. Moist areas like locker rooms and public showers also harbor these fungi. The infection spreads very easily through several means:
- Direct Contact with Infected Individuals: Coming into direct bodily contact with someone who has the infection can transmit tinea manuum. The infected person may or may not show symptoms but can still be a carrier.
- Contact with Infected Animals: Touching an animal that has the infection can spread tinea manuum. Various animals, including pets like dogs and cats (especially puppies and kittens), and farm animals such as cows, horses, pigs, and goats, can carry the fungus.
- Contact with Fomites: Fomites are objects or materials that can carry an infection. Tinea manuum can spread through indirect contact with fomites by sharing clothes, towels, and bedding. The fungus can also survive on hard surfaces in moist environments, such as locker rooms and public showers.
- Environmental Contact: Touching soil and other objects in the environment infected by the fungus can also lead to transmission.
- Self-Inoculation: Many people develop athlete's foot (tinea pedis) before tinea manuum. Because the fungus is so spreadable, it can be transferred from the feet to the hands after scratching the infected area.
The skin becomes infected when it comes into contact with dermatophytes. These fungi produce enzymes called keratinases, which digest the keratin protein in the skin, allowing the fungi to grow and spread, causing a rash.
Risk Factors for Tinea Manuum
Certain factors can increase an individual's susceptibility to developing tinea manuum:
- Environmental Factors: Living in or visiting tropical environments or areas with hot, humid weather. Using public showers, locker rooms, indoor pools, and sports facilities.
- Close Living Quarters: Living in close proximity to others, such as in dormitories.
- Occupational Exposure: People who work with their hands are at higher risk. This includes masseurs, barbers, farmworkers, veterinarians, car mechanics, and machine operators who have close contact with people, animals, or chemicals.
- Contact Sports: Engaging in contact sports like wrestling or football.
- Sharing Personal Items: Sharing objects and materials such as clothing, towels, bedding, hairbrushes, and sports equipment.
- Weakened Immune System: Conditions like HIV/AIDS, cancer, and diabetes can weaken the immune system, making individuals more susceptible to fungal infections.
- Other Health Conditions: High blood pressure (hypertension), atherosclerosis, obesity, and excessive sweating (hyperhidrosis) are also considered risk factors.
- Pre-existing Fungal Infections: Having another fungal infection on the body, such as athlete's foot or jock itch, increases the risk of spreading it to the hands.
Diagnosis of Tinea Manuum
A healthcare provider can diagnose tinea manuum based on its characteristic appearance and symptoms. To confirm the diagnosis, they may employ several methods:
- Visual Examination: The doctor will examine the rash for the typical ring-like appearance, raised borders, scaling, and any blisters or cracks.
- Wood's Lamp Examination: This ultraviolet light can cause certain fungal infections to fluoresce, aiding in diagnosis.
- Microscopic Examination: A skin scraping or nail clipping may be taken and examined under a microscope to identify fungal elements.
- Fungal Culture: Samples collected from the affected skin or nails can be sent to a laboratory for fungal culture to identify the specific type of fungus.
It is important to differentiate tinea manuum from other skin conditions that affect the hands, such as hand dermatitis, psoriasis, and exfoliative keratolysis, as the treatments differ significantly.
Treatment for Tinea Manuum
Tinea manuum is typically treated with antifungal medications. The type of medication and duration of treatment depend on the severity and extent of the infection.
Topical Antifungal Medications
For mild to moderate cases, topical (applied to the skin) antifungal medications are usually effective. These are available in various forms, including creams, gels, lotions, and powders.
- Over-the-Counter (OTC) Options: Many effective OTC antifungal products are available, such as clotrimazole (Lotrimin®, Mycelex®), miconazole (Desenex®), terbinafine (Lamisil AT®), and tolnaftate (Tinactin®). These should be applied as directed for the full treatment period, typically 2 to 4 weeks.
- Prescription Topical Medications: For more persistent infections, a healthcare provider may prescribe stronger topical antifungals like naftifine.
Oral Antifungal Medications
Oral antifungal medications may be prescribed for severe, widespread, or persistent infections that do not respond to topical treatments. These medications work from within the body to clear the infection.
- Common oral antifungal medications include fluconazole (Diflucan®), griseofulvin (Griasctin®), itraconazole (Sporanox®), and terbinafine (Lamisil®).
- Treatment with oral antifungals typically lasts from one to three months, depending on the medication and the severity of the infection.
What Causes Ringworms? | Skin Infection | The Dr Binocs Show | Peekaboo Kidz
Antifungal Shampoos
While not a primary treatment for tinea manuum, antifungal shampoos, such as ketoconazole shampoo (Nizoral A-D®), may be recommended to help prevent the spread of infection if other areas of the body, like the scalp, are also affected.
Important Considerations During Treatment
- Keep the Area Clean and Dry: Maintaining good hygiene and keeping the affected area clean and dry can help promote healing and prevent the spread of the fungus.
- Complete the Full Course of Treatment: It is crucial to use antifungal medications for the entire prescribed duration, even if symptoms improve, to ensure the infection is fully eradicated.
- Avoid Steroid Creams: Corticosteroid creams may reduce inflammation but should not be used to treat ringworm, as they can worsen the infection by suppressing the immune response and allowing the fungus to spread.
- Prevent Re-infection: Wash clothing, sheets, and towels in hot water and detergent. Disinfect surfaces in the home, especially in moist areas like bathrooms, using disinfectant sprays or bleach.
- Wash Hands Frequently: Wash hands thoroughly after touching the infected area or any other part of the body.
Home Remedies
Home remedies like apple cider vinegar or tea tree oil have limited scientific evidence of effectiveness for treating tinea manuum and may even cause irritation or inflammation. It is best to rely on proven antifungal treatments.
Prevention of Tinea Manuum
Preventing tinea manuum involves taking precautions to minimize exposure to the fungus:
- Keep hands clean and dry.
- Avoid touching or scratching other areas of the body that may have a fungal infection.
- Wear disposable gloves when treating any infected skin.
- Avoid skin-to-skin contact with individuals who have a fungal infection.
- Wear breathable footwear and change socks regularly, especially if you sweat excessively.
- Avoid sharing personal items like towels, clothing, and sports equipment.
- Shower immediately after participating in sports or using public facilities.
- Keep shared areas, especially in gyms and locker rooms, clean.
- If you have pets, ensure they are checked for ringworm by a veterinarian.
The outlook for tinea manuum is generally good, as fungal infections are usually treatable. However, prompt diagnosis and adherence to the prescribed treatment plan are essential for a full recovery and to prevent complications or spread.