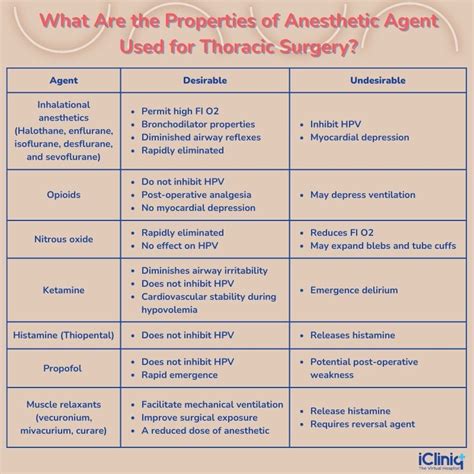
Topical anesthetics are extensively utilized in cosmetic dermatology, with a recent survey indicating that 97.5% of dermatology practices incorporate them for various procedures. These include laser and light-based treatments, ablative skin resurfacing, injectable fillers, and tissue tightening. While commercially available anesthetic combinations like EMLA (lidocaine 2.5%/prilocaine 2.5%) are frequently used, over half of surveyed practitioners reported using compounded anesthetics, with Benzocaine 20%, Lidocaine 6%, and Tetracaine 4% being the most common compounded options. This article aims to address common questions and concerns regarding the safety and efficacy of topical anesthetics.
How Topical Anesthetics Are Used
Topical anesthetic preparations, typically in cream or ointment form, are generally applied 30 to 90 minutes before a procedure. While surface layer numbing (approximately 1mm in depth) can occur relatively quickly, achieving deeper penetration (around 3mm) necessary for certain procedures may take about 60 minutes. A maximum depth of 5mm can be achieved after approximately 120 minutes of application. For instance, the package insert for commercially available lidocaine 2.5%/prilocaine 2.5% cream recommends at least 1 hour of exposure for minor dermal procedures and up to 2 hours for major dermal procedures. Similarly, lidocaine 7%/tetracaine 7% cream suggests application for 20-30 minutes before superficial dermatological procedures like non-ablative laser facial resurfacing, but recommends 60 minutes for procedures such as laser-assisted tattoo removal. After the designated exposure time, the remaining cream or ointment is usually wiped off with dry gauze, followed by cleaning the skin with wet gauze before the procedure commences. Some products have been applied under occlusion to accelerate the onset of action; however, this approach requires caution due to reported instances of death associated with the application of numbing creams for laser hair removal to the legs under occlusion.

Determining the Correct Application Amount
Compounded drugs, by their nature, are not FDA-approved and therefore do not undergo the same rigorous real-world patient testing for safety and efficacy as commercially available products. Determining the appropriate amount to apply per a given surface area to achieve adequate numbing while avoiding potential local or systemic adverse effects presents a challenge. Referencing commercially available products can assist in determining reasonable maximum application amounts for some anesthetics. For example, lidocaine 7%/tetracaine 7% cream recommends approximately 1mm thick application across the skin surface, with suggested amounts ranging from 1g for a 2-square-inch area up to a maximum of 53g (equivalent to 3,710mg lidocaine and 3,710mg tetracaine) for a 62-square-inch area. If a higher concentration lidocaine preparation, such as a 30% product used in some studies for intense pulsed light treatment, were applied, the equivalent of 3,710mg of lidocaine would be found in approximately 12g of that preparation. While direct comparison between compounded and FDA-approved products is difficult, using commercially available products as a guide can help in making decisions regarding the maximum appropriate dose per surface area. It is crucial to note that these parameters are for single doses prior to a procedure and not for repeated topical dosing, for which a much lower maximum would be expected. Furthermore, commercially recommended maximums are generally based on intact skin; significantly higher levels of anesthetic may be absorbed through inflamed, damaged, or compromised skin.
Adverse Effects of Topical Anesthetics
Topical anesthetics can be associated with both local and systemic adverse effects. A survey of practices revealed that 17.9% of respondents reported a history of adverse events, including lidocaine toxicity, contact dermatitis, allergic reactions, and corneal abrasion. Commercially available lidocaine 7%, tetracaine 7% cream lists common adverse effects as primarily localized, such as erythema (47%), skin discoloration (including blanching, ecchymosis, and purpura) (16%), and edema (14%). Systemic adverse effects were reported in approximately 1% of patients, mainly manifesting as headache, vomiting, dizziness, and fever. Less common but more serious adverse effects included syncope, hypotension, hyperventilation, and sweating. Following topical anesthetic application, initial blanching may occur within about 90 minutes, potentially followed by rebound vasodilation leading to skin erythema or redness. It is important to counsel patients about the likelihood of these cutaneous reactions, as they are fairly common with topical anesthetic application.
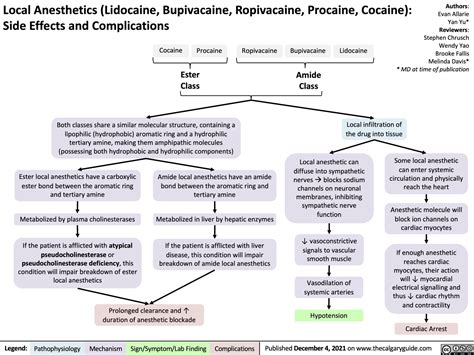
Local Adverse Effects
- Erythema (redness)
- Skin discoloration (blanching, ecchymosis, purpura)
- Edema (swelling)
Systemic Adverse Effects
- Headache
- Vomiting
- Dizziness
- Fever
- Syncope (fainting)
- Hypotension (low blood pressure)
- Hyperventilation
- Sweating
Anesthetics and Vasoconstrictors
Anesthetics are sometimes combined with vasoconstrictors, such as epinephrine or phenylephrine. Vasoconstrictors work by slowing the mobilization of the anesthetic, thereby prolonging its effect and reducing peak blood levels and systemic absorption. These agents are more commonly added to anesthetics intended for application to mucous membranes (e.g., in dental procedures) or for injected anesthetics. Vasoconstrictors may enhance the risk of skin blanching when combined with anesthetics. Studies involving common combinations like lidocaine/epinephrine/tetracaine gel or solution applied before minor procedures have noted skin blanching as a relatively common effect, similar to injectable combination products utilizing epinephrine.
HCl Salts vs. Base Forms of Anesthetics
Anesthetics are frequently available in both hydrochloride salt forms and non-salt or "base" forms. The chosen salt form can influence the API's behavior and its compatibility with various vehicles. While HCl salts exhibit greater solubility, the base forms, when combined, demonstrate a eutectic effect, meaning their melting point is lowered upon mixing. This can facilitate smooth incorporation into anhydrous systems without the need for a wetting agent but may also affect the integrity of some cream bases, leading to a thin or separated preparation. Although specific information comparing formulations applied to intact skin using HCl versus base forms is not widely available, the lower melting point of eutectic mixtures may enhance skin penetration. Conversely, HCl salts possess superior aqueous solubility compared to base forms. For applications where a penetration enhancer is generally not required, such as on mucous membranes for dental anesthetics or nasally before an ENT procedure, HCl salts offer the advantage of high solubility in the aqueous vehicles commonly used for these administration routes.
Formulation Notes
Anesthetics can pose challenges to thickening systems. Some quick notes on base compatibility with anesthetics are available, particularly concerning Fagron, Humco, and Letco branded bases. For further inquiries on the use of compounded anesthetics or for formulation support, reaching out to the Fagron Academy team via their FACTS Questions form is recommended.
How To Apply Topical Numbing Cream
tags: #topical #anesthetic #numbing #cream