Oral papillomas, commonly known as oral squamous cell papillomas, are benign (non-cancerous) growths that originate from the stratified squamous epithelium, the protective tissue lining the inside of your mouth. These are essentially harmless overgrowths of the cells that form the surface of your mouth. Oral papillomas are typically diagnosed in individuals between the ages of 30 and 50 and account for 3-4% of biopsied soft tissue lesions in the oral cavity.
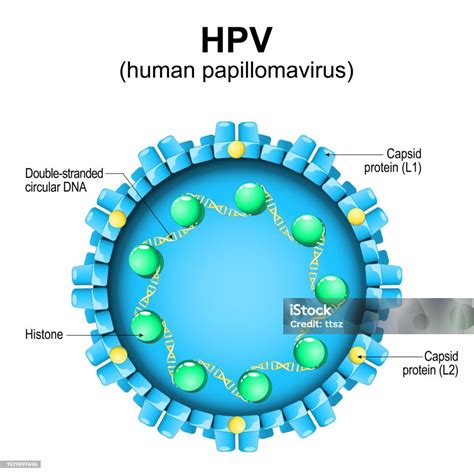
The primary cause of oral papillomas is infection with the Human Papillomavirus (HPV). This is the same virus responsible for warts on other parts of the body and is a common sexually transmitted infection. Oral papillomas are most commonly a result of infection with HPV types 6 and 11. Oral HPV is thought to spread mainly through oral sex and mouth-to-mouth contact. While not a direct cause, a compromised immune system can make an individual more susceptible to HPV infections and may allow them to persist longer.
Symptoms and Appearance of Oral Papillomas
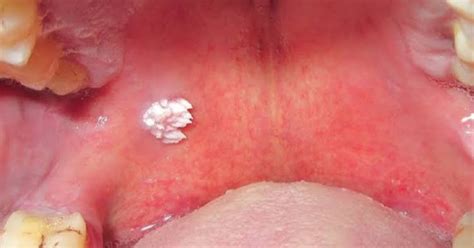
One of the most recognizable characteristics of an oral papilloma is its appearance. It often looks like a small, solitary cauliflower-like growth, or it might have numerous finger-like projections, giving it a rough, wart-like, or cobblestone surface. These growths can be pedunculated, meaning they are attached to the oral tissue by a narrow stalk, much like a mushroom. Less commonly, they can be sessile, which means they have a broader, flatter base.
The color of an oral papilloma can vary; it might appear white, pink, or even match the normal color of the surrounding oral mucosa. The whiteness often comes from a thickening of the keratin layer on the surface. Oral papillomas can appear almost anywhere inside the mouth, but certain areas are more common than others. Research indicates that oral squamous cell papillomas are most commonly found on the inside of the cheek, on the tongue, or inside the lips. Many people find oral papillomas during routine dental checkups because they often don’t cause any symptoms at all.
The most striking characteristic of oral papilloma symptoms is often the lack of them. However, just because they are often painless doesn’t mean they are always unnoticed. When discussing oral papilloma symptoms, the visual aspect is usually the primary indicator. Key characteristics include:
- Single, discrete growth: Typically, an oral papilloma appears as a single, well-defined lesion.
- Cauliflower or wart-like mass: This is the classic description.
- White, pink, or normal tissue color: The color can vary.
- Slow-growing: These growths tend to develop very slowly over time.
- Usually painless: This is a recurring theme.
- Sensation of a foreign body: Even if it doesn’t hurt, a growth in your mouth can feel strange.
- Interference with chewing: Depending on its size and location, a papilloma might get in the way when you are chewing food.
Oral papillomas are usually painless and are not treated unless they interfere with eating or are causing pain.
Types of Oral Warts and Their Causes
Warts are flesh-colored bumps caused by the human papillomavirus (HPV). Oral HPV can be transmitted from person to person. Common types of warts that can be found on the tongue include:
- Squamous papilloma: These cauliflower-like lesions are white and result from HPV strains 6 and 11. They are most commonly found on the tongue, inside of the lips, soft palate, or inside of the cheeks.
- Verruca vulgaris: These bumps are caused by HPV 2 and 4.
- Focal epithelial hyperplasia (Heck’s disease): These lesions are linked to HPV 13 and 32. They typically appear as papules of white or pink color, giving a cobblestone look, and mostly affect the oral mucosa, lips, and tongue in children, but can occur at any age.
- Condyloma acuminata: These lesions are typically found in the genital area but can spread to the tongue through sexual contact. They are associated with HPV 2, 6, and 11.
Tongue warts may develop after performing oral sex if the receptive partner has genital warts. If your partner has oral HPV, it may also be possible to contract the virus if you engage in open-mouth kissing. If you touch a wart with your hand and then put that part of your hand in your mouth, you could develop a wart on your tongue. For example, if you bite your nails, you could introduce a wart virus from your fingers to your mouth.
Certain factors can make you more susceptible. This includes having a weakened immune system, which makes it harder for your body to fight off viruses. If you have a cut or scrape, the virus can also enter your body through a break in the skin.
Diagnosis of Oral Papillomas
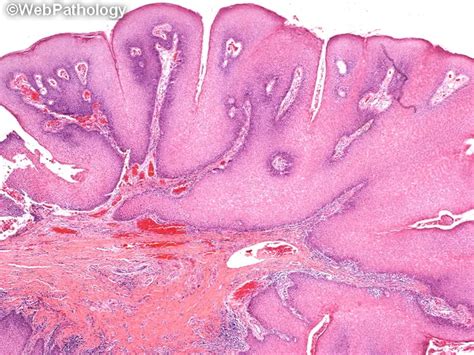
The diagnostic process typically begins with a visual inspection by a dental professional. However, a biopsy is often needed to confirm the nature of the growth. This tissue sample is then sent for histopathological examination, where a pathologist examines it under a microscope.
- Visual Inspection: Your dentist will carefully examine the growth, noting its size, shape, color, texture, and location.
- Differential Diagnosis: Based on the visual inspection, your dentist will consider several possibilities.
- Biopsy for Confirmation: The definitive diagnosis of an oral papilloma usually requires a biopsy. This is a simple procedure performed in-office, often under local anesthesia, where a small piece of the growth is removed and sent to a lab for microscopic analysis. This is crucial to confirm it is indeed a benign papilloma and rule out anything more serious.
Treatment Options for Oral Papillomas
Because oral papillomas are benign and typically harmless, treatment options vary. If the lesion is small, painless, and not interfering with any oral functions, observation may be recommended. Spontaneous regression has even been described in some cases.
When treatment is necessary, common options include:
- Surgical Excision: This is the most common and definitive treatment. The papilloma is carefully cut away from the surrounding tissue, often with a small margin of healthy tissue to ensure complete removal. This procedure is done in-office, usually with local anesthesia, and has a very low recurrence rate.
- Laser Ablation: Using a specialized laser, the growth can be precisely removed or vaporized.
- Cryotherapy: This involves freezing the papilloma with liquid nitrogen, causing it to slough off.
- Trichloroacetic acid: This chemical treatment has shown effectiveness in removing oral warts.
- Imiquimod: While often used for external warts, this topical cream has also been found to be effective and well-tolerated in the mouth.
Some warts will go away on their own without treatment, but this can take months or even years. While waiting for a wart to disappear, try eating on the side of your mouth opposite the wart to reduce irritation and the chance of biting it. If a wart doesn't improve or you wish to have it removed, consulting a healthcare professional is advised.
Prevention of Oral HPV and Papillomas
Preventing oral papillomas largely comes down to preventing HPV infection. Key prevention strategies include:
- HPV Vaccine (Gardasil 9): The HPV vaccine is highly effective at preventing infection from the HPV types it covers, including HPV-6 and HPV-11, which are the main culprits behind oral papillomas. While primarily known for preventing cervical and other cancers, it also significantly reduces the risk of oral HPV infections. The CDC recommends routine HPV vaccination for 11- to 12-year-olds, and for everyone through age 26 if not already vaccinated.
- Safe Sex Practices: Since oral HPV is primarily transmitted through oral sex and mouth-to-mouth contact, practicing safe sex can reduce your risk. This includes limiting sexual partners and consistently and correctly using barrier methods like condoms and dental dams during oral sex.
- Regular Dental Check-ups for Early Detection: While not a prevention method, regular visits to your dentist are crucial. Any new or unusual growth in your mouth warrants a professional evaluation.
Generally speaking, it’s best to avoid open-mouth kissing and oral sex if you or a partner have a wart on your tongue. Using a condom, dental dam, or other barrier can help reduce the risk of transmission. Getting the HPV vaccine-and encouraging partners to do so-can also help reduce the risk of infection.
HPV Vaccine and Cancer Prevention
Oral Papilloma vs. Oral Cancer
It is important to differentiate between a benign oral papilloma and other, more serious oral lesions that might be caused by different strains of HPV, particularly high-risk types like HPV-16, which are linked to oropharyngeal cancers. While oral papillomas themselves are not cancerous, persistent high-risk oral HPV infections can lead to oropharyngeal cancer. HPV-positive oropharyngeal cancers usually start as a tiny lump in your tonsils or on the base of your tongue, making them hard to see in the early stages. As the disease progresses, signs can include a lump in your neck or cheek, a white or red patch on your tonsils, coughing up blood, earaches, hoarseness, jaw pain or swelling, sore throat and trouble swallowing, and unexplained weight loss.
While warts on the tongue are typically not a sign of oral cancer, it's crucial to have any unusual or persistent lesions in the mouth examined by a dentist or dermatologist. Strains of HPV that cause common warts are considered "lower risk" and rarely cause cancer.
Key differences to note:
- Oral Papilloma: Small, cauliflower-like, often white/pink, usually painless, benign.
- Oral Cancer (HPV-related): Can present as a persistent sore, lump, or discoloration; may be painful; associated with high-risk HPV strains (e.g., HPV-16).
This table underscores why professional diagnosis is so important. If you’ve noticed any unusual growth in your mouth, your dentist is your first and best resource.
Other Causes of Tongue Bumps
It's important to remember that not every bump on the tongue is a wart. Other possibilities include:
- Irritation from sour or acidic foods and beverages
- Injury from biting your tongue or burning it on hot liquid or food
- Transient lingual papillitis (lie bumps)
- Canker sore
- Cold sore
- Oral syphilis
- Oral thrush
See a dentist or dermatologist to diagnose any unusual lesion or bump that appears in your mouth.