Hair loss, or alopecia, can be a distressing condition with a significant impact on a person's quality of life. Patients often first consult their family physician for diffuse or patchy hair loss. While scarring alopecia is best evaluated by a dermatologist, nonscarring alopecias can frequently be diagnosed and treated in a primary care setting.
Understanding Hair Growth Cycles
Hair growth occurs in three phases: anagen (active growth, approximately 90% of hairs), catagen (degeneration, less than 10% of hairs), and telogen (resting, 5% to 10% of hairs). Understanding these cycles is crucial for diagnosing various forms of hair loss.
Common Causes of Alopecia
The pattern and type of hair loss can offer important clues to its etiology. It is convenient to categorize causes into focal (patchy) and diffuse patterns.
Focal (Patchy) Hair Loss
Patchy hair loss is often associated with several conditions:
- Alopecia Areata: This is an acute, patchy alopecia affecting up to 2% of the population, with no gender predilection. Approximately 20% of affected patients are children. The exact etiology is unknown, but it is likely autoimmune in nature. Patients may experience a single episode or periods of remission and recurrence. Hair loss can manifest in three patterns:
- Patchy alopecia: Circumscribed, oval-shaped, flesh-colored patches on any part of the body.
- Alopecia totalis: Involves the entire scalp.
- Alopecia universalis: Involves the entire body.
- Tinea Capitis: This is a dermatophyte infection of the hair shaft and follicles, primarily affecting children. Risk factors include household exposure and sharing contaminated items. Trichophyton tonsurans is the most common cause in North America. Patients typically present with patchy alopecia, which may be accompanied by scaling. Other findings can include adenopathy and pruritus. A painful, boggy plaque called a kerion may develop, often with purulent drainage and lymphadenopathy. If the diagnosis is unclear, a potassium hydroxide preparation of a skin scraping can reveal hyphae. Tinea capitis requires systemic treatment as topical agents do not penetrate hair follicles effectively.
- Trichotillomania: This is an impulse-control disorder characterized by the conscious or unconscious pulling, twisting, or twirling of hair. It commonly presents with frontoparietal patches of alopecia that can extend to the eyelashes and eyebrows. The hair may appear uneven, with twisted or broken-off hairs. This condition can lead to self-esteem issues and social avoidance. Treatment may involve cognitive behavioral therapy and selective serotonin reuptake inhibitors, though strong evidence for their efficacy is limited. Psychiatric referral is often indicated.
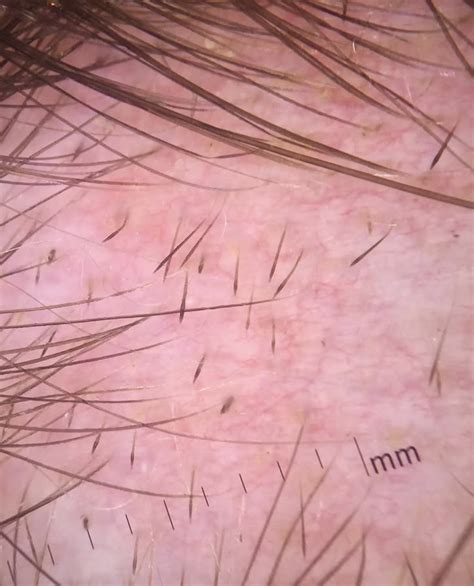
Evaluation of the scalp may reveal short vellus hairs, yellow or black dots, and broken hair shafts. Microscopic examination of hair follicles can show "exclamation mark hair," which is narrower near the scalp.
Diffuse Hair Loss
Diffuse hair loss is commonly due to effluvium:
- Telogen Effluvium: This is a nonscarring, noninflammatory alopecia of relatively sudden onset. It occurs when a large number of hairs enter the telogen phase and shed three to five months after a physiologic or emotional stressor. The list of inciting factors is extensive and includes severe chronic illnesses, pregnancy, surgery, high fever, malnutrition, severe infections, and endocrine disorders. Patients may notice clumps of hair in their shower or hairbrush. Examination of the scalp typically shows uniform hair thinning. Telogen effluvium is usually self-limited, resolving within two to six months. Treatment involves identifying and eliminating the underlying cause and providing reassurance. Potentially causative medications should be discontinued if possible.
- Anagen Effluvium: This is abnormal, often abrupt, diffuse hair loss during the anagen (growth) phase. It is caused by an event that impairs the mitotic or metabolic activity of the hair follicle. Chemotherapy is the most common cause, with an incidence of approximately 65%. Certain medications like cyclophosphamide, nitrosoureas, and doxorubicin are frequently implicated. Other causative agents include tamoxifen, allopurinol, levodopa, and toxins. Anagen effluvium is usually reversible, with hair regrowth occurring one to three months after cessation of the offending agent. Permanent alopecia is rare. Physician support is especially important for patients undergoing chemotherapy.
Androgenetic Alopecia
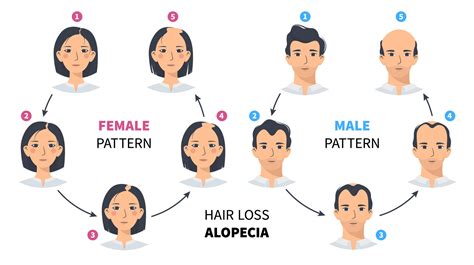
Androgenetic alopecia is the most common form of hair loss in both men and women and is considered a normal physiologic variant. It is most prevalent in white men, with increasing prevalence at 30, 40, and 50 years of age. While less common in women, it can affect a significant percentage of women over 70. The pattern of hair thinning differs between sexes: men typically present with bitemporal thinning, frontal and vertex thinning, or complete hair loss with residual hair at the occiput and temporal fringes. Women usually experience diffuse thinning of the vertex with sparing of the frontal hairline, though some may have thinning over the lateral scalp.
Treatment for Androgenetic Alopecia
Treatment is based on patient preference:
- Topical Minoxidil: Available as a 2% or 5% solution, it is approved for treating androgenetic alopecia in men. Hair regrowth is generally more robust at the vertex than in the frontal area and may take six to 12 months to show improvement. Treatment should be continued indefinitely, as hair loss recurs upon discontinuation.
- Finasteride: This oral medication (1 mg per day) is approved for men with androgenetic alopecia for whom topical minoxidil has been ineffective. Both minoxidil and finasteride can stimulate hair regrowth in some individuals and are more effective in preventing the progression of hair loss.
Dry Scalp and Its Impact on Hair Health
Healthy hair grows best from a scalp that is adequately nourished and moisturized. The outermost layer of the scalp, composed of skin cells, requires protection and hydration, similar to the rest of the body's skin.
The Role of Sebum
Sebum, the oil produced by glands throughout the body, is the scalp's natural moisturizer. It coats and protects hair strands and contributes to a healthy scalp microbiome. Insufficient sebum production can lead to a dry, itchy scalp.
Can a Dry Scalp Cause Hair Loss?
A dry scalp lacks sufficient moisture, creating an unfavorable environment for healthy hair growth. It can become sore, red, flaking, or itchy. Frequent scratching of an itchy scalp can damage the scalp and existing hairs. Furthermore, the underlying causes of a dry scalp, such as dehydration or poor diet, can also affect the quality of hair produced, potentially leading to hair loss.
Distinguishing Dry Scalp from Dandruff
Dandruff is a fungal condition resulting in the shedding of dead skin cells from the scalp. While it can sometimes be related to a dry scalp, they are not always experienced together. Individuals with oily or well-moisturized scalps can still have dandruff. A dry scalp may not always be accompanied by dandruff, but scratching can accelerate skin cell shedding. The scalp's dermis may appear red, sore, or irritated without excessive shedding.

Causes of Dry Scalp
Several factors can contribute to a dry scalp:
- Environmental Factors: Changes in weather (seasonal variations, travel), humidity levels, wind, heat, cold, and sun exposure can irritate the scalp.
- Dehydration and Diet: Insufficient intake of moisture and nutrients can impair sebum production.
- Harsh Hair Products: Sulfates, common in many shampoos for their foaming action, can strip the scalp of natural oils and exacerbate dryness or sensitive scalp conditions.
- Over-washing Hair: Frequent washing removes protective sebum, leaving the scalp more vulnerable.
- Product Residue: Improper rinsing or excessive use of hair products can irritate the scalp.
- Hormonal Changes: Fluctuations due to pregnancy or aging can affect sebum levels and the scalp microbiome.
- Skin Conditions: Conditions like Seborrheic Dermatitis (SD) or psoriasis can lead to a dry scalp. Other medical conditions or medications may also impact sebum production, hormone levels, or hair production, contributing to dryness.
Treatment and Prevention of Dry Scalp
Understanding the cause is the first step in treating a dry scalp. Lifestyle adjustments and specially formulated scalp products can help:
- Reduce Washing Frequency: Allow sebum to build up by not washing hair daily.
- Stay Hydrated: Drink plenty of water.
- Use Gentle Products: Opt for shampoos designed for sensitive scalps or those without sulfates.
- Avoid Harsh Treatments: Minimize high heat styling and chemical treatments. Use lower heat settings on hairdryers and heat protectants.
- Moisturize: Use scalp masks or nourishing treatments.
- Sun Protection: Protect the scalp from UV rays with sunscreen designed for hair and scalp.
- Nutrient-Rich Diet: Consume foods rich in omega-3 fatty acids (e.g., oily fish) to stimulate sebum glands and vitamin A (e.g., root vegetables) crucial for sebum production.
Monitoring your scalp's condition weekly and adjusting dietary intake as its natural balance is restored can be beneficial.
When Flakes Indicate a Medical Condition
While mild flaking can be attributed to dry skin or common dandruff, persistent or severe symptoms may signal underlying medical skin conditions:
- Scalp Psoriasis: Characterized by thicker, silver scales and red patches, potentially extending beyond the hairline.
- Seborrheic Dermatitis: An eczema that affects the scalp, causing oily patches, inflammation, and thick, yellowish flakes.
- Contact Dermatitis: An adverse reaction to hair products like shampoos, dyes, or styling gels, leading to itching and flaking.
- Tinea Capitis (Scalp Ringworm): A fungal infection causing hair loss, scaly patches, and itching.
- Folliculitis: Inflammation of hair follicles due to infection, resulting in itchy, red, and scaly patches.
If flaking persists despite standard dandruff treatments, consulting a dermatologist is recommended for accurate diagnosis and appropriate management.
Key Symptoms Signaling More Than Dandruff
While ordinary dandruff is often manageable with over-the-counter shampoos, certain signs suggest a more serious condition:
- Redness, swelling, or oozing.
- Well-defined patches or thick scales, which may be itchy or painful.
- Significant hair loss or pain associated with scalp issues.
- No improvement after weeks of using medicated OTC shampoos.
These symptoms may warrant professional evaluation to prevent worsening of the condition and potential complications.
Available Treatments for Scalp Conditions
Treatment options for persistent scalp flaking vary depending on the underlying cause:
- Over-the-Counter (OTC) Options: Shampoos containing zinc pyrithione or selenium disulfide can help manage itching and redness associated with seborrheic dermatitis.
- Antifungal and Steroid Shampoos: Prescription-strength shampoos may be recommended for chronic or resistant conditions. Antifungal agents combat yeast growth, while steroid shampoos reduce inflammation.
- Dermatologist-Administered Treatments: For severe cases, treatments like ultraviolet (UV) phototherapy for psoriasis or injectable medications for eczema may be considered.
- Scalp Exams and Biopsies: A dermatologist may perform a scalp examination or biopsy to precisely diagnose the cause and tailor a treatment plan.
When to See a Dermatologist for Scalp Issues
While mild dandruff can often be managed at home, persistent shedding that lasts for weeks or worsens is a clear indicator to consult a scalp expert. Conditions like seborrheic dermatitis, scalp psoriasis, eczema, or fungal infections require professional evaluation and specialized care to prevent excessive hair loss, infection, and other complications. Early intervention by a dermatologist can lead to a personalized treatment plan, often including prescription medications and in-clinic therapies, to restore scalp health.