Annular lichenoid dermatitis of youth is a rare skin condition that was first described in 2003 by Annessi et al. It was initially identified in young, healthy individuals from the Mediterranean region.
Clinical Presentation
The mean age of patients affected by this skin condition is 10 years. The clinical presentation of this lichenoid dermatosis changes according to the duration of the lesions. Initially, sharply demarcated, 1-5 cm sized erythematous macules appear, which then enlarge to form annular, reddish-brown, non-scaling patches with hypopigmented centres and slightly raised borders. The lesions are typically asymptomatic and are found on the patient's trunk, groin, and less frequently, in the axillae. In a case study, a 15-year-old boy presented with a 1-year history of annular skin lesions that had begun as small macules and then slowly enlarged. These lesions had not responded to topical 0.1% mometasone furoate cream applied twice daily for a month. Dermatological examination revealed 4-5 cm sized reddish-brown, annular plaques with non-atrophic, clear centres and indurated borders on the left flank and right side of the abdomen.
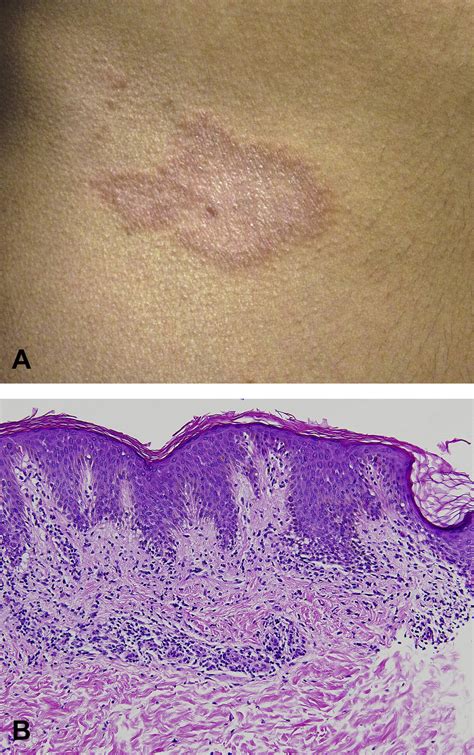
Histopathology
Annular lichenoid dermatitis of youth is diagnosed on histopathology, with the presence of specific hallmark features. A punch biopsy from the border of a plaque in one patient showed elongated rete ridges and hydropic degeneration in the basal layer with apoptotic keratinocytes and perivascular lympho-plasmacytic infiltrates in the superficial dermis. Histological features also vary with the stage of the lesions. In the early macular lesions, band-like lymphocytic infiltrates occur in the papillary dermis and dermo-epidermal junction where vacuolar alteration is also seen. Then, some of the lymphocytes move to the tips of the rete ridges, leading to massive keratinocyte necrosis/apoptosis. The epidermis shows quadrangular rete ridges, a basket-weave horny layer, and a normal thickness of the granular layer. Intense keratinocyte damage leads to rete ridge loss in late lesions. Some lymphocytic infiltration and melanophages in the papillary dermis are also seen at the late stages. In a study involving 23 patients, histology revealed a peculiar lichenoid dermatitis with massive necrosis/apoptosis of the keratinocytes limited to the tips of rete ridges, in the absence of dermal sclerosis and epidermotropism of atypical lymphocytes. The infiltrate was composed mainly of memory CD4(+) CD30(-) T cells with few B cells and macrophages. Analysis of T-cell receptor-gamma-chain gene rearrangement in skin biopsy specimens revealed polyclonality in all 15 cases studied.
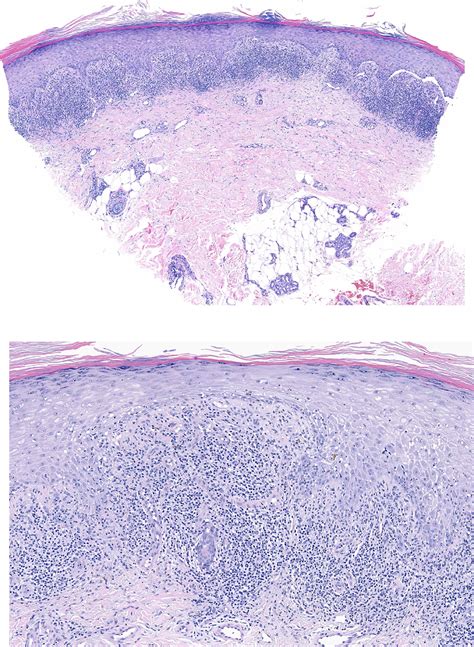
Etiology and Pathogenesis
An exact cause for annular lichenoid dermatitis of youth is yet to be discovered. It is believed to share pathogenic factors with other lichenoid dermatoses, like lichen planus, graft versus host disease, and lichenoid drug eruption, which involve a T-cell-mediated response and subsequent apoptosis of basal keratinocytes. Triggering factors described in lichenoid dermatoses include persistent viral reactions, immunological changes, neoplastic diseases, contact with chemicals, ultraviolet exposure, and drugs. Laboratory results in one patient were within normal limits, including complete blood counts, routine biochemistry, urinalysis, antistreptolysin titer, rheumatoid factor, erythrocyte sedimentation rate, and C-reactive protein. Indirect immunofluorescence for antinuclear antibody was weakly positive at 1:100 with a mottled pattern. An extensive infectious disease workup, including serological testing for Epstein-Barr virus, cytomegalovirus, Borrelia, hepatitis B and C, and stool examination for parasites and ova, was negative. Patch testing with standard series antigens to exclude contact hypersensitivity was also negative.
Differential Diagnosis
The characteristic histology helps to differentiate annular lichenoid dermatitis of youth from other clinical diagnoses such as erythema migrans, morphea, vitiligo, patch-type granuloma annulare, interstitial granulomatous dermatitis, annular erythemas, and mycosis fungoides.
Prognosis and Treatment
Annular lichenoid dermatitis of youth slowly progresses, with no serious complications being reported to date. The disease runs a chronic course. The duration of annular lichenoid dermatitis of youth varies. Treatment options include topical and/or systemic corticosteroids, photo(chemo)therapy, natural ultraviolet light exposure, and topical tacrolimus. However, relapses are common with discontinuation of treatment. Out of 21 cases described from 2005 to 2013, most lesions were successfully treated with topical corticosteroids, but these recurred once therapy was discontinued. In a reported case, considering the side effects of long-term potent steroid use, the patient was treated with topical tacrolimus 0.1% twice daily. The lesions faded in 1 week and completely resolved following 3 months of this therapy. Cessation of the treatment resulted in a recurrence of the lesions, but they again responded rapidly to topical tacrolimus (0.1%) twice daily. Tacrolimus likely worked in this case due to its suppressive effects on T lymphocytes.
Tacrolimus (Protopic) for Eczema: How It Works, How to Take It, and Side Effects | GoodRx
tags: #annular #lichenoid #dermatitis #of #youth