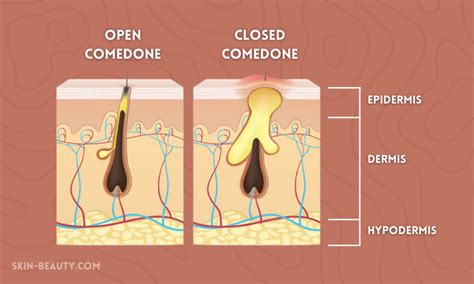
Closed comedones, often mistaken for tiny whiteheads or textural bumps, are a common form of acne that can be particularly frustrating. Unlike inflamed acne such as cysts or pustules, closed comedones are non-inflammatory. They form when pores become clogged with dead skin cells, oil, and debris, but remain sealed, preventing redness or swelling. This can lead to a collection of small, flesh-colored or slightly raised bumps that create an uneven skin texture.
The journey to understanding and managing closed comedones often involves detective work, as pinpointing the exact cause can be challenging. However, several factors are commonly implicated in their formation. One of the most frequent culprits, according to dermatologists, is skincare itself. While ingredients listed as comedogenic, such as cetyl alcohol and coconut oil, can be beneficial for some skin types, they may be overly moisturizing for others, triggering the development of closed comedones.
What are Closed Comedones?
Definition and Characteristics
Comedonal acne is a mild form of acne vulgaris characterized by the presence of comedones. These small, flesh-colored bumps develop when hair follicles become clogged with sebum and dead skin cells. Comedonal acne is primarily non-inflammatory, distinguishing it from other types of acne that involve inflammation, such as papules or pustules. When the hair follicle and pore are clogged, it can form small bumps filled with dead cells, bacteria, and excess oil. These are separated into two categories: open comedones (blackheads) and closed comedones (whiteheads).
Closed comedones, also known as whiteheads, occur when the follicle is blocked by sebum, dead skin, and bacteria, resulting in white or skin-colored bumps. These bumps are known as closed comedones and look like tiny whiteheads. While what we commonly refer to as whiteheads are pustules (filled with pus), closed comedones are NOT filled with pus and may be slightly hard to the touch, though they can still appear white in color. In some cases, larger comedones known as macrocomedones may develop, which can be more challenging to treat. Microcomedones are the earliest stage of acne lesions and are not visible to the naked eye.
Common Areas Affected
Comedonal acne commonly affects the forehead, nose, and chin, but can occur on other areas of the face and body as well. The T-zone, which includes the forehead, nose, and chin, is particularly prone to comedone formation due to its higher concentration of sebaceous glands. Closed comedones on the chin are very common and can often be due to hormonal changes. As hormone levels fluctuate, sebaceous glands can produce more or less oil, making hair follicles more likely to get plugged up. Closed comedones on the forehead are also common, and can sometimes be linked to sweat and hair products. If you have bangs, excess oil production can also contribute to their formation.
Causes of Comedonal Acne
Excess Sebum Production
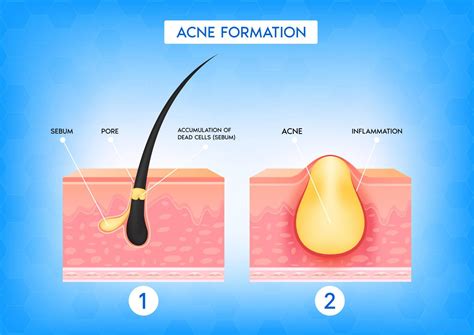
Overactive sebaceous glands can lead to increased oil production, clogging pores and contributing to the formation of comedones. This excess sebum can combine with dead skin cells to form a plug in the hair follicle, leading to comedone development. When excessive sebum, combined with dead skin cells, bacteria, and dirt, clogs pores, it results in a cluster of small, firm bumps close to the skin’s surface. These bumps, or comedones, can be closed or open, and are typically characterized as whiteheads and blackheads.
Hormonal Changes
Fluctuations in hormone levels, particularly during puberty, can stimulate sebum production. Androgens, such as testosterone, play a significant role in increasing sebum production, which can lead to the formation of comedones. Changes in androgen production can increase acne-causing bacteria, inflammation, and sebum production, leading to clogged pores. Cortisol, a stress hormone, can also cause increased inflammation and excess sebum, resulting in clogged pores.
Environmental Factors and Lifestyle Habits
High humidity, exposure to certain irritants, and the use of comedogenic skincare or makeup products can exacerbate comedonal acne. Additionally, certain foods and dietary habits may influence acne development in some individuals, although the relationship between diet and acne is complex and varies from person to person. Hair products like shampoos and conditioners, as well as oily or greasy hair products spread over the forehead and temple area, can contribute to comedones. Baseball hats or headbands that rub on the forehead skin can also be a factor. External factors that clog skin pores can also cause comedones. In some cases, over-exfoliating can also be a culprit, as drying out the skin too much can exacerbate existing breakouts.
Genetic Predisposition
Some individuals may be more prone to developing comedonal acne due to their genetic makeup. If your parents or siblings have a history of acne, you may be more likely to experience it as well. Familial tendency (genetics) is one of the main factors contributing to comedones.
Identifying Comedonal Acne
Visual Signs and Symptoms
Key characteristics of comedonal acne include small, flesh-colored or slightly raised bumps on the skin, blackheads appearing as dark spots on the skin’s surface, and whiteheads presenting as closed bumps beneath the skin. This results in a rough or uneven skin texture, predominantly with non-inflammatory lesions.
Differentiating Comedonal Acne from Other Types of Acne
Comedonal acne is primarily non-inflammatory, unlike other forms of acne such as inflammatory acne, which may include red, swollen lesions like papules or pustules. Comedonal acne focuses on the presence of comedones, while other types may involve more severe lesions or widespread inflammation. Unlike your standard zit or pimple, comedonal acne isn’t inflammatory, so it doesn’t come with the redness, pain, and swelling typically associated with cystic acne. If you try to squeeze a comedone, there’s a good possibility nothing will come out, and you’ll risk aggravating it, turning it into a full-blown zit.
Treating Closed Comedones
Over-the-Counter Topical Treatments
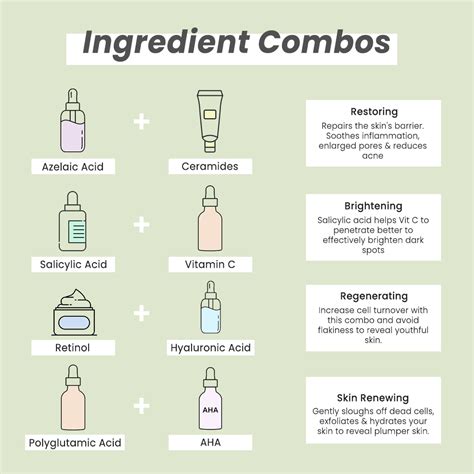
Several effective over-the-counter options can help manage comedonal acne. Salicylic acid, a beta-hydroxy acid (BHA), helps exfoliate the skin and unclog pores. Benzoyl peroxide, while primarily known for its antibacterial properties, can also help reduce comedones. Retinol, a vitamin A derivative, promotes cell turnover and helps prevent the formation of microcomedones. These ingredients are effective in treating closed comedones by increasing cell turnover and reducing the "stickiness" of sloughed-off skin cells.
Key Ingredients for Treatment:
- Salicylic Acid: This oil-soluble BHA penetrates deep into pores to break up clogged sebum and debris, and exfoliate the skin. It is considered the single best medical-grade ingredient for the treatment of clogged pores.
- Retinoids: Derivatives of vitamin A, such as retinol, adapalene, and tretinoin, are highly effective in treating comedonal acne. They promote cell turnover, prevent pore blockage, and improve the overall appearance of the skin. Over-the-counter products often contain retinol, while stronger versions like tretinoin and adapalene may require a prescription.
- Niacinamide: This ingredient offers gentle exfoliating properties, helps control excess sebum production, and can reduce dryness and redness associated with retinol. It is recommended for individuals with sensitive skin.
- Mandelic Acid: A gentle AHA, mandelic acid is suitable for sensitive skin. It exfoliates, helps unclog pores, and has anti-bacterial properties.
- Glycolic Acid: A stronger AHA, glycolic acid effectively loosens dead skin cells on the surface. It requires patch testing.
- Lactic Acid: Another gentle AHA, lactic acid loosens the "glue" holding skin cells together, allowing dead skin cells to be cleared and stimulating cell growth.
Prescription Medications and Their Benefits
For more severe or persistent cases, a dermatologist may prescribe stronger topical retinoids like tretinoin or adapalene. Topical antibiotics are not typically the first choice for comedonal acne but may be used if there is a risk of bacterial infection. In some cases, oral antibiotics or hormonal treatments may be recommended to address underlying causes and reduce acne severity.
Professional Treatments
Chemical Peels and Extractions:
In-office procedures can provide additional benefits. Chemical peels using acids like glycolic or salicylic acid exfoliate the skin and unclog pores. Microdermabrasion physically exfoliates the skin to remove dead skin cells and unclog pores. Comedone extraction is a procedure performed by a skincare professional to manually remove comedones. Microdermabrasion can reduce the appearance of closed comedones and create a smooth complexion, but caution is advised with at-home treatments.
Chemical Peel Demonstration
Establishing a Consistent Skincare Routine
Consistency is key when managing comedonal acne. Establishing a regular routine of cleansing, treating, and moisturizing is crucial for keeping skin clear and healthy. It is important to use oil-free, non-comedogenic makeup and skincare products to avoid clogging pores. Tailoring your skincare routine to your individual needs is crucial for achieving effective results. Remember that clear skin rarely happens overnight; improvement can take several months.
Recommended Skincare Routine Steps:
- Cleansing: Use a gentle cleanser to remove excess oil, impurities, and dead skin cells without over-drying the skin. Products with salicylic acid are beneficial.
- Toning: A toner can refine pores and help balance oil production.
- Treating: Apply a serum or treatment containing active ingredients like salicylic acid or retinoids to target comedones and prevent new formations.
- Moisturizing: Use an oil-free, non-comedogenic moisturizer to hydrate the skin without clogging pores. Niacinamide-based moisturizers can also help.
- Exfoliation: Gentle daily exfoliation with ingredients like mandelic acid is often more successful than strong, infrequent exfoliation.
Natural Remedies
For those seeking natural alternatives, options include Tea Tree Oil, known for its antibacterial properties, and Witch Hazel, a natural astringent that helps open clogged pores. Charcoal and clay masks are also beneficial for absorbing trapped sebum and exfoliating the skin.
Important Precautions
Do not squeeze your bumps! Unlike pustules or blackheads, closed comedones occur when a plug in the hair follicle causes a bump to form under the skin. Squeezing them can lead to inflammation, infection, and scarring. If you are struggling to see results or feel overwhelmed, talk to a dermatologist. They can provide expert feedback and recommend appropriate treatments based on your specific skin type and acne severity.