Eczema, a chronic skin condition affecting millions, can manifest in various parts of the body, including sensitive areas like the scrotum. Scrotal eczema, characterized by itching, redness, and dryness of the scrotal skin, is a distressing condition that requires understanding for effective management and treatment.
What is Scrotal Eczema?
Scrotal eczema is the inflammation of the skin on the scrotum, a highly sensitive area. This condition can be triggered by a combination of factors, including genetic predisposition, environmental influences, and the use of certain skincare products. The inherent sensitivity of the scrotal skin makes it more susceptible to irritation and discomfort when affected by eczema.
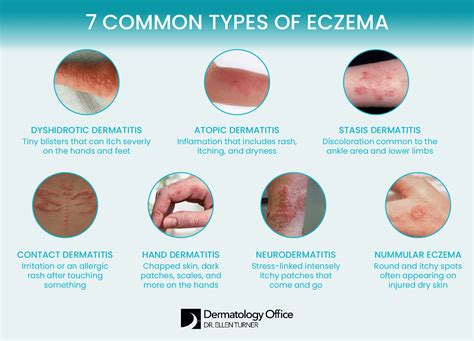
Types of Eczema and Their Manifestations
Eczema is an umbrella term for several distinct skin conditions, each with unique signs and causes. Understanding these types is crucial for accurate diagnosis and treatment:
Atopic Dermatitis
This is the most common form of eczema, characterized by itchy and inflamed skin. Management typically involves keeping the skin moisturized, identifying and avoiding triggers, and using creams to reduce inflammation.
Contact Dermatitis
This type occurs when the skin reacts to a substance it comes into contact with. Common culprits include soaps, detergents, and metals. There are two subtypes:
- Allergic Contact Dermatitis: An immune system reaction to an allergen.
- Irritant Contact Dermatitis: Caused by direct damage to the skin from an irritant substance.
Dyshidrotic Eczema
Characterized by small, itchy blisters that can also burn, this type typically affects the hands and feet. Management includes keeping the skin clean and dry, using appropriate creams, and applying cool compresses.
Seborrheic Dermatitis
This type of eczema is often an inflammatory response to the Malassezia yeast naturally found on the skin. While commonly affecting the scalp, it can also develop in the groin area.
Causes and Risk Factors of Scrotal Eczema
Several factors contribute to the development of scrotal eczema:
Genetics
A family history of eczema or allergies can increase an individual's likelihood of developing scrotal eczema. Specific gene mutations, such as those affecting the filaggrin protein responsible for skin barrier function, can lead to reduced skin moisture and increased susceptibility to irritants and bacteria.
Environmental Factors and Irritants
External factors play a significant role. These can include:
- Harsh Chemicals: Found in soaps, detergents, bubble baths, and personal care products.
- Fragrances and Dyes: Common in cosmetics, perfumes, and laundry detergents.
- Friction and Moisture: Tight clothing, sweating, and skin-to-skin friction can exacerbate irritation.
- Certain Materials: Latex in condoms, synthetic fabrics in underwear.
- Incontinence: Urine and feces are highly irritating to the skin.
- Topical Products: Aftershave, personal deodorants, hemorrhoid preparations, and antiseptics.
- Body Piercings and Tattoos: Can increase the risk of developing allergic contact dermatitis, particularly to metals like nickel or dyes like PPD.
Lifestyle Factors
Stress can also contribute to eczema flare-ups. Additionally, certain lifestyle choices, such as the use of harsh soaps or hot water for bathing, can dry out the skin and worsen symptoms.
Symptoms of Scrotal Eczema
The symptoms of scrotal eczema are similar to those experienced with eczema on other parts of the body, but they are localized to the scrotum and surrounding genital area. These can include:
- Intense itching, often described as severe and persistent.
- Redness or discoloration of the skin. On darker skin tones, this may appear as dark brown, purple, or ashen gray patches.
- Dry, sensitive, scaly, or leathery skin.
- Swelling.
- Oozing of fluid from the skin, potentially leading to blisters filled with clear fluid.
- Broken hairs.
- In severe cases due to scratching, the development of thickened, leathery skin known as lichenification.
Diagnosis of Scrotal Eczema
Diagnosing scrotal eczema involves a thorough evaluation by a healthcare professional. The process typically includes:
Medical History and Physical Examination
A doctor will examine the affected area and discuss the patient's symptoms, medical history, and potential triggers. This initial assessment is crucial for understanding the presentation of the condition.
Differential Diagnosis
It is essential to differentiate scrotal eczema from other conditions that may present with similar symptoms. These include:
- Fungal Infections: Such as jock itch (tinea cruris) or yeast infections (thrush), which can cause redness, itching, and sometimes a ring-like rash.
- Psoriasis: A chronic autoimmune condition causing red, scaly patches.
- Intertrigo: An inflammatory rash in skin folds, often due to friction and moisture.
- Sexually Transmitted Infections (STIs): Including genital herpes, chlamydia, gonorrhea, and genital warts, which can cause discharge, sores, or other symptoms.
- Lichen Sclerosus: A chronic inflammatory skin condition that can affect the genital area.
- Scabies: A contagious skin infestation caused by mites.
Allergy Testing
In some cases, allergy testing, such as patch testing, may be recommended to identify specific allergens that could be triggering or exacerbating the eczema.
Skin Biopsy
A skin biopsy, where a small sample of skin is taken for laboratory analysis, may be performed if the diagnosis is uncertain.
Treatment and Management of Scrotal Eczema
Managing scrotal eczema focuses on alleviating symptoms, reducing inflammation, preventing flare-ups, and improving the quality of life. Treatment approaches vary depending on the severity of the condition.
Over-the-Counter (OTC) Treatments
For mild cases, OTC options can provide relief:
- Hydrocortisone Cream: A common choice for reducing inflammation and itching. It should be used as directed, typically for no more than seven days without medical advice.
- Emollients: Fragrance-free and hypoallergenic moisturizers help keep the skin hydrated and protect the skin barrier.
- Anti-itch Preparations: Some emollients with anti-itch properties may help relieve severe itching.
- OTC Antihistamines: Medications like diphenhydramine or cetirizine can help manage itching, particularly in cases of allergic dermatitis.
Prescription Medications
More severe cases often require prescription treatments:
- Topical Corticosteroids: Stronger formulations than OTC options, prescribed to reduce inflammation and itching. These should be used cautiously in the genital area due to increased absorption.
- Topical Calcineurin Inhibitors (TCIs): Medications like pimecrolimus and tacrolimus can modulate the immune response and are suitable for sensitive areas like the groin, as they do not typically thin the skin.
- Oral Corticosteroids: Such as prednisone, may be prescribed for severe inflammation.
- Antibiotics or Antifungal Medications: Prescribed if a secondary bacterial or fungal infection develops.
- Injectable Medications: For severe eczema unresponsive to other treatments, biologics like dupilumab and tralokinumab may be considered.
- Phototherapy: In severe cases, exposure to ultraviolet light under medical supervision may be used.
How to use topical steroids
Lifestyle and Skincare Modifications
These changes are crucial for long-term management and prevention:
- Gentle Skincare Routine: Use mild, fragrance-free cleansers and moisturizers specifically designed for sensitive skin. Avoid harsh soaps and excessive washing.
- Clothing Choices: Wear loose-fitting, breathable clothing made from natural fibers like cotton, bamboo, or silk. Avoid tight trousers and thongs.
- Laundry Practices: Use non-biological laundry detergents and ensure clothes are thoroughly rinsed.
- Avoid Triggers: Identify and avoid personal triggers, which can include certain fabrics, chemicals, fragrances, and stress.
- Hydration: Keep the skin well-moisturized with emollients, especially after bathing.
- Cool Compresses: Applying a cool, wet cloth can help soothe itching and inflammation.
- Oatmeal Baths: Adding colloidal oatmeal to a warm bath can help reduce itching.
- Stress Management: Techniques like mindfulness, meditation, or yoga can help manage stress, a common eczema trigger.
When to See a Doctor
It is important to seek medical attention if:
- Symptoms do not improve with self-care or OTC treatments within a week.
- Symptoms worsen significantly.
- There are signs of infection, such as increased redness, swelling, pus, fever, or pain.
- The condition significantly impacts daily life, mood, or sleep.
- Unusual discharge, bleeding, or other symptoms suggestive of an STI are present.
- Pain or swelling in the testicles occurs.

Living with Scrotal Eczema
Scrotal eczema can be a chronic condition that requires ongoing management. While there is no cure, consistent adherence to treatment plans, lifestyle modifications, and regular consultation with healthcare providers can effectively control symptoms and prevent flare-ups. Support groups and online resources can also provide valuable information and emotional support for individuals managing eczema.
tags: #contact #dermatitis #scrotum