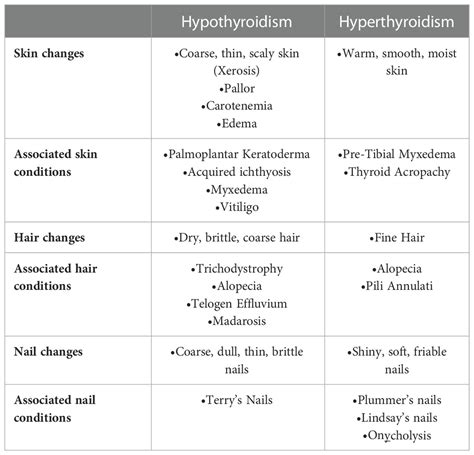
Thyroid disorders, encompassing both hypothyroidism (an underactive thyroid) and hyperthyroidism (an overactive thyroid), can significantly impact skin health. Imbalances in thyroid hormones affect metabolism, energy levels, temperature control, and the rate of cell regeneration, including skin cells. These disruptions can manifest in various ways, altering the skin's texture, color, moisture, and overall appearance. The skin's responsiveness to hormonal fluctuations makes it an early indicator of thyroid dysfunction, sometimes revealing symptoms before more systemic issues become apparent.
The Role of the Thyroid Gland
The thyroid gland, a butterfly-shaped organ located at the base of the neck, produces thyroid hormones, primarily thyroxine (T4) and triiodothyronine (T3). These hormones are crucial for regulating numerous bodily functions. When their levels are too low (hypothyroidism) or too high (hyperthyroidism), these natural processes, including skin cell turnover and hydration, become disrupted.
Hypothyroidism and Its Effects on Skin
Hypothyroidism occurs when the thyroid gland does not produce sufficient thyroid hormones, leading to a general slowing of bodily systems. This condition commonly affects the skin in several ways:
Dry and Itchy Skin
One of the most prevalent symptoms of hypothyroidism is dry, rough, or scaly skin. This can occur due to decreased thyroid hormone levels reducing the production of the skin's protective barrier and potentially leading to hyperkeratosis (thickening of the outer skin layer). Reduced sweat secretion also contributes to the skin's inability to cool itself effectively, exacerbating dryness.
Managing dry skin often involves regular moisturizing with rich, hydrating products containing ingredients like ceramides or hyaluronic acid. Opting for lukewarm showers and gentle, moisturizing body washes can also help prevent further dryness and irritation.
Brittle Hair and Nails
The health of hair and nails is also affected by hypothyroidism. Hair may become coarse, dry, brittle, and prone to breakage. Similarly, nails can become weak and prone to splitting. This is often due to insufficient nutrient utilization for maintaining healthy hair and nail growth.
Skin Coloring Changes
Hypothyroidism can lead to changes in skin pigmentation. A common manifestation is pallor, or a pale appearance, resulting from narrowed blood vessels that reduce blood flow to the skin to maintain core body temperature. Anemia, often associated with hypothyroidism, can also contribute to this paleness.
Other skin coloring changes associated with hypothyroidism include:
- Vitiligo: This is an autoimmune disorder where pigment-producing cells (melanocytes) are destroyed, leading to lighter patches on the skin. Approximately 25% of individuals with subclinical or overt hypothyroidism also experience vitiligo.
- Carotenemia: A deficiency in thyroid hormone can impair the conversion of carotene to vitamin A, leading to a buildup of carotene and a yellowish hue to the skin.
- Myxedema: In about 10% of hypothyroidism cases, the skin can become waxy, swollen, or doughy. This can also affect facial features, causing swollen lips, puffy eyelids, and tongue enlargement.
Puffy Face and Swelling
In some instances, hypothyroidism can cause fluid retention, leading to a puffy appearance, particularly around the eyes. This can contribute to a tired or bloated look.
Hyperpigmentation and Its Causes
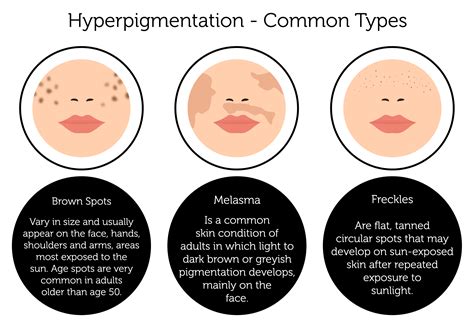
Hyperpigmentation refers to the darkening of the skin in areas that are lighter than the natural complexion. This can occur due to various factors, including genetics, medical conditions, medications, and environmental influences. The body darkens the skin as a protective mechanism against harmful ultraviolet (UV) radiation from the sun, which is a primary cause of hyperpigmentation.
Common Types of Hyperpigmentation:
- Freckles (Ephelides): Small, tan or brown spots typically appearing on sun-exposed skin during childhood.
- Age Spots (Solar Lentigines): Larger, tan to dark brown spots that develop with age due to sun exposure.
- Melasma: Irregular dark patches, often on the face, commonly affecting females in their 20s and 30s.
- Maturational Hyperpigmentation: Gradual darkening of sun-exposed skin, particularly on the sides of the face, in individuals with darker skin complexions.
- Periorbital Hyperpigmentation: Darkening around the eyes.
- Acanthosis Nigricans: Darkening of the skin in areas prone to friction, such as the armpits, groin, and neck.
- Post-inflammatory Hyperpigmentation (PIH): Discoloration resulting from skin inflammation or injury, such as acne, burns, or rashes.
Hyperthyroidism and Its Effects on Skin
In contrast to hypothyroidism, hyperthyroidism is characterized by an overproduction of thyroid hormones, leading to an acceleration of bodily processes. This can also manifest on the skin:
- Increased Skin Sensitivity: The skin may become more reactive, leading to redness, rashes, or hives.
- Moist and Smooth Skin: Individuals with hyperthyroidism might experience skin that is smoother, flushed, or more moist than usual.
- Hair Changes: Hair may become thinner and softer.
- Excessive Sweating: Increased metabolic rate can lead to increased perspiration.
The Connection Between Vitiligo and Autoimmune Thyroid Disease
There is a recognized autoimmune link between certain types of vitiligo, particularly non-segmental vitiligo, and Autoimmune Thyroid Disease (AITD). While the exact mechanisms are still being investigated, a shared genetic susceptibility is a leading theory. Research has identified genes associated with vitiligo, and a family history of thyroid disease is a known risk factor for AITD, suggesting a potential genetic predisposition linking the two conditions.
Estimates vary, but studies indicate that individuals with vitiligo are more likely to have a thyroid disorder. For example, one study found that 12.9% of participants with vitiligo had thyroid disease, with hypothyroidism, subclinical hypothyroidism, hyperthyroidism, and Hashimoto's thyroiditis being the most common forms.
Diagnosis of Vitiligo and Thyroid Disorders
Diagnosing these conditions involves different approaches:
- Vitiligo: Diagnosis is typically made through a visual examination of the skin. Doctors may inquire about family history, skin sensitivity, and changes in pigmentation.
- Thyroid Disorders: Diagnosis often relies on specific laboratory tests, including thyroid antibody tests, thyroid-stimulating hormone (TSH) tests, and free T3 and T4 tests. Medical imaging of the thyroid gland may also be used. A physical examination might reveal thyroid swelling or inflammation.
Treatment Approaches
While vitiligo and AITD can share underlying autoimmune mechanisms, their treatments are distinct:
- Vitiligo Treatments: Options include phototherapy, topical corticosteroids, topical and oral immunosuppressants (to suppress immune system activity), and skin grafts to improve pigmentation.
- AITD Treatments: The primary treatment for hypothyroidism is levothyroxine, a synthetic thyroid hormone that replaces lost hormones. In certain cases of AITD, particularly when the eyes are affected (as in Graves' disease), doctors may prescribe immune-suppressing drugs or high-dose steroids.
Currently, there is no evidence to suggest that medications used to treat one condition will effectively treat the other simultaneously. Furthermore, immunosuppressants carry significant side effects and are typically considered only when other treatments are insufficient.
When Your Body Attacks Itself – Autoimmune
Managing Thyroid-Related Skin Changes
Managing skin changes associated with thyroid disorders involves a multi-faceted approach:
- Moisturize Regularly: Use rich, hydrating moisturizers to combat dryness.
- Lukewarm Showers: Avoid hot water, which can strip the skin of its natural oils.
- Balanced Diet: Consume nutrient-rich foods to support thyroid function and skin health.
- Gentle Skincare: Opt for mild, fragrance-free, and hypoallergenic skincare products.
- Stay Hydrated: Drink plenty of water to maintain skin moisture.
- Sun Protection: Use sunscreen daily to protect the skin from UV damage, which can worsen hyperpigmentation and sensitivity.
- Consult a Doctor: Seek professional medical advice for diagnosis and treatment of any significant skin changes or suspected thyroid issues.
Frequently Asked Questions
I have vitiligo. Do I also have a thyroid disease?
No. While thyroid disease and other autoimmune disorders are more common in people with vitiligo, it is not a certainty that everyone with vitiligo will develop them. Many individuals with vitiligo do not have thyroid disease.
Can thyroid disease also cause changes in skin?
Yes. Hypothyroidism can cause the skin to become dry, paler than usual, cold, and scaly. Hair may also become dry and break easily. Hyperthyroidism may cause skin to become smooth, flushed, or moist, and hair to grow thinner and softer.
Will treating thyroid disease help with vitiligo?
The primary treatment for thyroid disease focuses on restoring normal hormone levels, which can help alleviate skin symptoms related to the thyroid condition itself. However, it will not directly impact or treat vitiligo.
tags: #hypothyroidism #and #hyperpigmentation #of #skin