Skin tears are acute wounds that occur suddenly and typically heal within an expected timeframe. However, for some individuals, these tears can become complex, chronic wounds that present challenges in healing. While often healing on their own, proper care is essential to promote healing and reduce the risk of infection.
What are Skin Tears?
Skin tears are wounds that may resemble large cuts or scrapes. They are classified as acute wounds, meaning they occur suddenly and usually heal predictably over time. However, some skin tears can develop into chronic wounds, indicating difficulty in healing.
Types of Skin Tears
Skin tears can be:
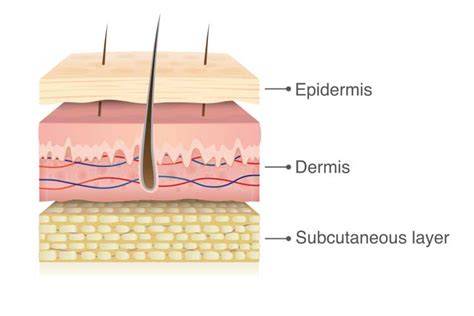
- Partial thickness: The top layer of skin (epidermis) separates from the underlying layer (dermis).
- Full thickness: Both the epidermis and dermis separate from the underlying tissues. This type commonly occurs on thinner skin areas like the arms, back of hands, and elbows.
Causes of Skin Tears
Trauma is the primary cause of skin tears. Common examples of traumatic events include:
- Blunt force impact
- Shearing forces (cuts or scrapes)
- Friction from skin rubbing against surfaces
While these traumas might cause minor cuts or bruising in most individuals, they can lead to skin tears more easily when the skin is thin or fragile.
Risk Factors for Skin Tears
Skin tears are most prevalent in older adults due to age-related thinning and fragility of the skin. However, other risk factors include:
- Being female
- Having a chronic illness
- Immobility
- Problems with blood vessels, heart, or lungs
- A history of previous skin tears
- Long-term corticosteroid use
- Malnutrition
- A history of falls
- Dry skin
Newborns and highly active individuals are also considered at risk.
Recognizing Signs of Infection
Once a skin tear occurs, it's crucial to prevent infection. Signs of infection that warrant immediate medical attention include:
- Fever
- Chills
- Pus
- Foul odor
- Redness
- Swelling
- Worsening pain
Home Care for Minor Skin Tears
Minor skin tears can often be managed at home. The recommended approach includes:
- Gentle Cleaning: Clean the skin tear with sterile water or an isotonic saline solution. For smaller, superficial tears, gentle soap and water may be used.
- Covering the Wound: Cover the tear completely. Avoid applying adhesive bandages directly to the wound. Instead, use gauze with petrolatum and then cover with dry gauze.
- Managing Skin Flaps: If there is a skin flap, gently reposition it over the tear before covering. This can aid in faster skin healing and regrowth.
While waiting for treatment or healing, managing pain can be achieved using a warm compress on the affected area. Using an inflatable seat or mattress may also alleviate discomfort.

When to Seek Medical Advice
It is advisable to consult a healthcare provider if you experience any of the following:
- Signs of infection (fever, chills, aches, foul-smelling drainage, pus, worsening pain)
- A large or full-thickness tear where both skin layers have separated from underlying tissue
- Bleeding that does not stop
- Other health concerns, such as a weakened immune system
A healthcare provider may apply special dressings to promote healing and use skin glue for skin flaps, as stitches are generally not suitable for fragile skin. Antibiotics may be prescribed for infections, and a tetanus shot might be administered depending on the cause of the tear and vaccination status. They can also help identify strategies to prevent future skin tears.
Pilonidal Disease: A Related Condition
Pilonidal disease is a condition that primarily affects teenagers and young adults, occurring at the base of the spine near or at the top of the buttock crease. It typically begins with an entrapped hair around the area of the buttocks crease, which can lead to the formation of a cyst. This cyst may resemble a large, hard pimple or boil.
Symptoms of Pilonidal Disease
A key indicator of an infected pilonidal cyst is a foul odor emanating from the cyst or its drainage. If infected, the cyst can develop into an abscess, and the affected area may exhibit multiple openings to the skin, known as pilonidal sinuses.
Pilonidal Disease Treatment and Prevention
Even if a pilonidal cyst resolves on its own, it can recur, especially if pilonidal sinuses have developed. To reduce the risk of recurrence, keeping the area hair-free and maintaining excellent hygiene is recommended. Thorough wiping after defecation is also advised.
Pilonidal Cyst Disease Explained — Why It Keeps Coming Back
Treatment for pilonidal cysts is individualized and depends on factors such as previous occurrences, presence of other skin issues like abscesses or sinuses, and recovery speed. Options range from non-surgical treatments to surgical intervention.
Non-Surgical Treatment Methods:
- Draining the cyst: A minor incision allows for the drainage of fluid from an infected cyst, often performed in a provider's office.
- Injections: Phenol injections can treat mild to moderate pilonidal cysts.
- Antibiotics: While antibiotics can manage skin inflammation, they are not sufficient to heal pilonidal cysts alone.
- Laser therapy: This method targets hair removal to prevent ingrown hairs that can lead to recurrent cysts.
Surgical Treatment:
For chronic or worsening pilonidal cysts that have formed sinus cavities, surgical removal (excision) of the cyst may be necessary. Post-surgery, the wound might be left open for packing or closed with sutures or a skin flap. Deroofing and curettage is a common treatment for simple pilonidal abscesses and sinuses, often performed under local anesthesia.
Minimally invasive surgery involves removing and cleaning sinus tracts, leaving the area open for drainage, with a gauze dressing applied. For complicated or recurrent pilonidal disease, more extensive surgical procedures may be recommended to remove or clean all sinus tracts.
To help prevent recurrence, maintaining the area's cleanliness and dryness is crucial. Daily bathing, thorough washing and drying of the intergluteal cleft, and avoiding hair and lint accumulation are important. Removing hair every other week or considering laser hair removal can also be beneficial. Showering immediately after exercise or sweating is also advised.
Managing Recurrent Skin Tears in the Gluteal Crease
Recurrent skin tears in the buttock crease, particularly in individuals with conditions like diabetes, can be exacerbated by friction and moisture. The presence of diabetes can affect skin health and healing. Maintaining a clean and dry area is paramount. Gentle cleansing products should be used, and harsh chemicals like boric acid should be avoided without medical guidance. Barrier creams can help protect the skin from irritation. It is essential to monitor for signs of infection, such as increased redness or pain, and consult a healthcare provider for appropriate wound care and diabetes management to promote healing and prevent recurrence.