What is Ringworm?
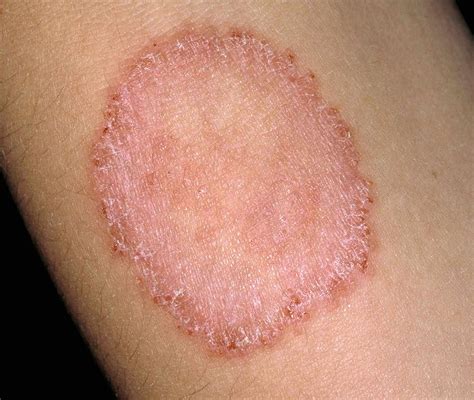
Ringworm, also known as dermatophytosis, is a highly contagious fungal skin disease that affects the superficial layers of the skin, hair, and nails. Despite its name, there are no worms involved. The name originates from the ring-like appearance of the lesions that manifest on an infected animal. This common skin infection can be particularly frustrating to treat, especially in breeding or rescue animal populations or pets with long hair coats. While relatively harmless to the animal, ringworm can spread to humans, particularly those who are young, old, or immunocompromised.
Causes and Common Species
Ringworm is caused by a fungus known as dermatophytosis. Different species of ringworm exist, with Microsporum canis (M.canis) being the most common culprit affecting dogs and cats. Ringworm infections are frequently observed in cats, dogs, horses, and cattle. The most common species of dermatophytes isolated according to animal species include:
- Cats: Microsporum canis, Trichophyton mentagrophytes, M. gyspeum
- Dogs: Microsporum canis
- Horses: Trichophyton equinum, Microsporum canis, Trichophyton veruccosum
- Cattle: T. veruccosum
Ringworm often occurs in the very young, the very old, and the immunocompromised. It is crucial to note that ringworm is not a bacterial infection, and therefore, the use of antibiotics in its treatment is not indicated.
Signs and Symptoms of Ringworm
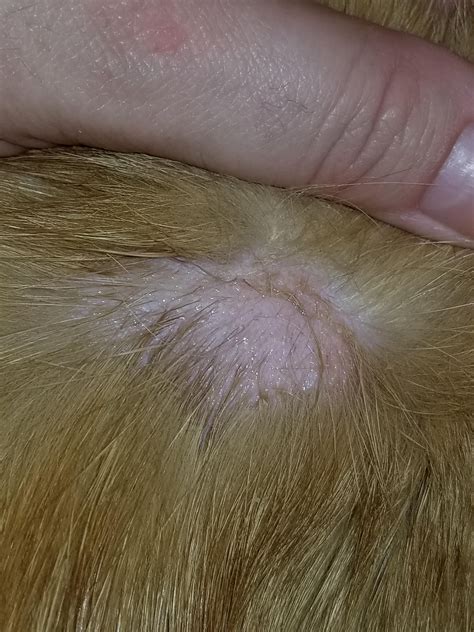
Ringworm is often diagnosed by the telltale clinical signs of bald circular patches of hair loss on an animal’s coat. The affected area may be crusty and have scaly skin with broken hairs, but generally, it is not itchy or painful, just unsightly. Initial ringworm symptoms include an area on the coat with raised hair, which can be easily plucked out, leaving a bald (alopecia) area. Sometimes these areas of skin are red and inflamed, although this usually resolves quickly.
Some animals can harbor ringworm and show relatively few signs, effectively acting as asymptomatic carriers of the infection. This is particularly common in cats, and if an infected cat enters a colony, it can result in massive environmental contamination with fungal spores.
Diagnosis of Ringworm
The initial diagnosis of ringworm is not particularly tricky, although the scaly patches can mimic some bacterial infections and parasitic diseases like Demodex. A formal diagnosis is worthwhile due to the zoonotic nature of ringworm, meaning it can be passed on to humans. In breeding operations and animal rescue centers, especially those housing cats, it is imperative that a formal diagnosis of any suspicious lesion is performed. This is because the skin disease can lead to unmanageable outbreaks, excessive costs, and potentially euthanasia due to its potential to spread to people.
The initial test most veterinarians perform is the examination of skin lesions with a special ultraviolet light called a Wood’s Lamp in a dark room. On close examination of plucked infected hair and skin cells, a positive result will appear as a fluorescent ‘blue’ color. However, it should be noted that environmental contaminants and some topical medications can also fluoresce. Although not a perfect diagnostic test due to the relatively high frequency of false-negative results, examination of hair and skin under a Wood’s lamp, when correctly used, can be a helpful and cost-effective screening tool to determine if ringworm spores are present. A negative Wood’s lamp examination does not rule out an infection, as only around 50% of M.canis infections will fluoresce. Therefore, suspicious lesions should undergo additional testing, such as microscopic examination of a sample of hair shaft including the hair follicles, and/or fungal culture.
Treatment of Ringworm
Treatment of animals and environmental management of ringworm must go hand in hand, especially during an outbreak. The principles of treatment are the same across different species. It is essential to remember that ringworm can infect humans, particularly those who are immunocompromised. Therefore, it is vital to treat any animals showing signs of infection and to use personal protective clothing when handling them. Practicing excellent disease control with quarantine and isolation of infected animals is also crucial to prevent further spread.
Topical Antifungal Treatment
A key component of the treatment strategy for ringworm infections involves topical antifungal therapies, such as shampoos and creams. Lime Sulphur (8% topical therapy) is a highly useful topical treatment with residual activity that can assist in clearing infection from the environment. It is safe for kittens and puppies (ensure they are kept warm after application) and can be applied twice weekly to cats and dogs. For horses, it can be applied daily initially, then twice weekly in the second week. The application involves applying powder, then spraying with water (do not pre-wet), and wiping paste over facial areas, avoiding the eyes. The treatment should be left to soak into the skin and hair without rinsing. Treatment should continue until two consecutive negative fungal cultures, taken a week apart, are obtained, as it is common for animals, especially cats, to appear cured while still being highly contagious. Spot application on affected areas is recommended.
Iodine, while sometimes considered, does not work as effectively as lime sulfur and is often ineffective. Chlorhexidine-medicated shampoo is not effective against fungal spores. Useful topical creams contain ingredients such as clotrimazole, terbinafine, or Miconazole.
Systemic Treatment of Ringworm
Oral antifungal medication is often used when it is difficult to wash infected animals, topical treatments are not working, or if the animal is severely affected and deeper areas of the hair follicle, where spores are often found, are difficult to reach. Oral antifungal drugs work by directly killing fungal cells or preventing their growth. It is important to note that these prescription veterinary medicines cannot be used in pregnant animals due to the risk of fetal toxicity and may need to be compounded to achieve the small doses required for kittens and puppies. Many of these oral antifungal drugs are more effectively absorbed when given with fat. Systemic therapy with oral medications often requires six weeks of treatment, followed by testing and potentially another two weeks of treatment to ensure all skin scrapings are negative.
Drugs that have shown effectiveness for ringworm treatment include Itraconazole (relatively safe with a long half-life in the skin), Fluconazole, Terbinafine, and Griseofulvin (though it has more toxic side effects than itraconazole). Ketoconazole should be avoided in cats due to hepatotoxicity (toxicity to the liver).
Clinical Trial Results
Clinical trials were carried out on 3 groups of 30 Friesian cattle naturally infected with Trichophyton verrucosum. One group was treated with 3.75% thiabendazole in glycerine, another with 5% tincture of iodine, and the last served as the control group without any treatment. Both preparations were applied locally on the ringworm lesions at 3-day intervals, with a total of 4 applications. The percentage of animals cured was 86.7% by thiabendazole and 46.7% by tincture of iodine.
Environmental Contamination Management
Because ringworm spores can survive in the environment for many years, environmental cleaning is a crucial part of the management strategy. Keeping infected animals in a single room (quarantining them) helps limit contamination and simplifies decontamination. Any bedding, baskets, collars, leads, and grooming equipment can be sources of potential contamination.
Removal of fungal spores from the environment can be achieved by first vacuum cleaning to remove as much dirt, debris, and spores as possible, followed by surface disinfection. The vacuum bag should be destroyed (burned) as it can be a future source of spores. Hypochlorite (bleach), glutaraldehyde solutions, or accelerated hydrogen peroxide are most efficacious against fungal spores. Always check with a veterinarian regarding product safety around pets. It is important to thoroughly follow label instructions to ensure product effectiveness against spores. Bleach solution (1:32 dilution) requires a prolonged contact period of at least 10 minutes before being thoroughly washed down with fresh water. Grooming equipment should either be cleaned multiple times with bleach or discarded and burned. Food bowls can also be a source of infection if not cleaned regularly in a high-heat dishwasher. Bedding, blankets, and toys can play a significant role in maintaining infection and should be washed regularly, preferably on days when topical treatments are applied. Items that cannot be easily washed should be discarded.
Prevention of Ringworm
Ringworm most often affects malnourished animals, those with concurrent diseases, internal or external parasites, or those living in crowded conditions. Practicing good husbandry and ensuring animals receive preventative health care and optimal nutrition can go a long way in preventing this skin problem. As there are no reliable screening tests or vaccines against ringworm, it is wise to avoid mixing young and adult animals from different families. All newcomers should receive a careful visual examination, and any animals with suspicious lesions must be quarantined in an isolation area.
Ringworm in Humans
In most cases, ringworm in humans can be treated at home with over-the-counter (OTC) antifungal treatments. Effective medications include miconazole (Cruex), clotrimazole (Desenex), and terbinafine (Lamisil). After cleaning the rash, apply a thin layer of antifungal cream to the affected area twice a day or as directed by the packaging, extending the treatment beyond the border of the rash. Keeping the area dry is important; wearing comfortable, breathable clothing like loose-fitting, long-sleeve shirts and pants can speed healing and prevent spreading. Daily washing of clothes and sheets in hot water with detergent is recommended to eliminate the infection faster, as fungal spores can transfer to bedding. Some people add borax or bleach to their wash to kill fungal spores. If ringworm develops on the feet or groin area, keep these areas dry and consider bathing with an antifungal wash and reapplying antifungal powder or lotion, ensuring the area is completely dry before dressing.
Tinea Capitis (Scalp Ringworm)
Ringworm on the scalp, known as tinea capitis, can present with symptoms such as severe itching, patches of hair loss, scalp boils, and severe dandruff. Scalp fungus almost always requires oral medications. Washing hair with an OTC medicated antifungal shampoo containing active ingredients like selenium sulfide and ketoconazole can also help kill fungi and reduce inflammation. If symptoms do not respond to home remedies or OTC treatments, a doctor may recommend prescription antifungal medications, which may need to be taken for weeks or months depending on the severity of the infection.