Skin rashes are a common manifestation of lupus, an autoimmune condition where the immune system mistakenly attacks the body's own tissues, primarily targeting skin cells in cutaneous lupus erythematosus (CLE). These rashes present as inflamed, itchy, bumpy, and discolored patches that can appear anywhere on the body, frequently on sun-exposed areas. While some individuals with lupus may not develop rashes, they tend to be intermittent, flaring up unexpectedly. Sensitivity to light or the sun's ultraviolet (UV) rays can trigger or exacerbate these rashes.
A healthcare provider can offer management strategies for lupus rashes and address their underlying cause. Lupus rashes vary depending on the specific type of lupus, with cutaneous lupus causing chronic skin inflammation. Different subtypes of CLE lead to distinct rash symptoms.
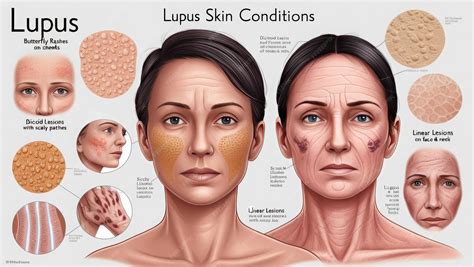
Types of Lupus Rashes
Lupus rashes are broadly categorized into specific types associated with different forms of the disease, as well as non-specific rashes that can occur in other inflammatory conditions.
Specific Cutaneous Lupus Rashes
These rashes are characteristic of lupus and are primarily confined to the skin. They can be further classified into chronic, subacute, and acute forms.
Chronic Cutaneous Lupus Erythematosus (CCLE)
CCLE, also known as chronic cutaneous lupus, results in ongoing skin problems that can persist for years. While symptoms may fluctuate, they rarely disappear completely. Lesions from CCLE can lead to permanent scarring or changes in skin color.
Discoid Lupus Erythematosus (DLE)
Discoid lupus is the most common form of CCLE. It typically affects the face and scalp but can appear anywhere on the body. Discoid lesions on the scalp may cause temporary or permanent hair loss. These rashes are often circular, coin- or disk-shaped, thick, and scaly. They may not itch or cause pain but can leave scars or discolorations (lighter, darker, or red to purple) upon healing. Chronic discoid rashes or sores increase the risk of skin cancer, particularly squamous cell carcinoma, especially if present on the lips or inside the mouth.
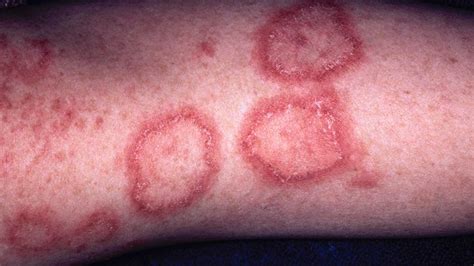
Lupus Profundus (Lupus Panniculitis)
This type of lupus affects the deeper layers of the skin, leading to ulcers that can result in permanent skin indentations upon healing.
Chilblain Lupus Rash
Characterized by itchy, painful, tender, and discolored bumps, this rash is triggered by cold and wet temperatures.
Lupus Erythematosus Tumidus (Lupus Tumidus)
This form presents as raised patches (plaques) with bumps and skin discoloration. Fortunately, these rashes do not typically leave permanent changes after healing.
Subacute Cutaneous Lupus Erythematosus (SCLE)
SCLE rashes commonly develop on sun-exposed areas such as the arms, shoulders, chest, and neck. These rashes appear relatively quickly, are not always present, and are typically not painful or itchy. While they do not scar, they can cause permanent skin discoloration (lightening or darkening). SCLE rashes may form shapes that connect into interlocking circles and can be triggered or worsened by ultraviolet (UV) light.
Approximately 10% of lupus patients have SCLE. The lesions are usually not thick or scaly and rarely scar, though they can cause discoloration. About half of individuals with SCLE also meet the criteria for systemic lupus erythematosus (SLE). SCLE can be caused or exacerbated by certain medications, such as proton pump inhibitors and calcium channel blockers, appearing months to years after starting the drug.
Acute Cutaneous Lupus Erythematosus (ACLE)
ACLE rashes occur during a lupus flare-up, indicating active disease. These rashes typically appear on the face, arms, legs, or other body parts. A common manifestation is the butterfly rash (malar rash). ACLE rashes can present with bumps, discoloration (pink to red or darker than natural skin tone), pain (burning sensation), and scales. Rarely, ACLE can also cause canker sores, hives, and temporary hair loss.
Almost everyone with ACLE also has systemic lupus erythematosus (SLE). There are two main forms: localized and generalized. The localized form includes the malar or "butterfly" rash, which spans the cheeks and bridge of the nose, resembling a butterfly. While often associated with SLE, the butterfly rash occurs in only about 30% of SLE patients. Generalized ACLE manifests as raised red rashes across the body, typically seen in severely ill SLE patients.

Neonatal Lupus Erythematosus Rash
This type affects newborns and may present as discolored, circular rashes.
Non-Specific Rashes in Lupus
Beyond the specific cutaneous lupus rashes, individuals with lupus can experience various non-specific skin manifestations that may also occur in other inflammatory or autoimmune conditions. These include:
- Mouth and Nose Sores: Painful ulcers or sores within the mouth or nose are common.
- Hives (Urticaria): Raised, itchy, and sometimes painful bumps that can last longer than 24 hours.
- Angioedema: Swelling, often of the lips, tongue, or eyelids.
- Cutaneous Vasculitis: Inflammation of blood vessels near the skin, restricting blood flow. This can cause hive-like lesions, itchy rashes that don't blanch when pressed, open sores, or even gangrene of the digits in severe cases.
- Skin Ulcers: Open sores on the skin.
- Bruises (Purpura): Small red or purple discolorations caused by leaking blood vessels. Petechiae are small spots, while eccymoses are larger.
- Livedo Reticularis: A lacy, web-like pattern under the skin, often violet or reddish, which may be accentuated by cold exposure.
- Telangiectasias: Small, dilated blood vessels visible on the skin.
- Palmar Erythema: Redness of the palms.
- Erythema Nodosum: Tender red nodules, usually on the shins.
- Vitiligo: Loss of skin pigment, resulting in white patches.
Causes and Triggers of Cutaneous Lupus
The exact cause of cutaneous lupus erythematosus (CLE) is not fully understood but is believed to result from a combination of genetic, environmental, and immune system factors.
Genetic Susceptibility
A family history of lupus or other autoimmune diseases increases the likelihood of developing CLE, suggesting a significant genetic predisposition. While lupus is not directly inherited, certain genetic traits can elevate risk when combined with other triggers. Studies indicate a higher incidence among individuals with close relatives who have the disease, pointing to shared genes and environmental exposures.
Environmental Factors
Various environmental triggers can contribute to the development or flare-ups of CLE.
Sun Exposure (UV Radiation)
Ultraviolet (UV) rays from the sun are one of the most common triggers for lupus skin rashes. Even brief exposure can cause flare-ups, especially in individuals with photosensitivity. Approximately 40-70% of people with lupus are sensitive to UV radiation. The immune system's process of removing UV-damaged cells can be prolonged in lupus patients, leading to a buildup of these cells and triggering an immune reaction and subsequent flare-up. This sensitivity can cause symptoms to worsen during summer months due to increased sun exposure.
UV radiation can lead to symptoms such as joint pain, numbness and tingling, and fatigue. Protective measures, including sunscreen, protective clothing, hats, and limiting sun exposure, are crucial for preventing CLE symptoms.
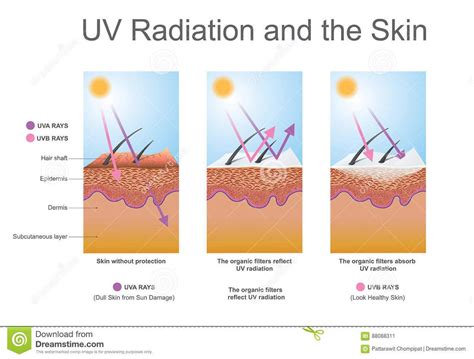
Heat Exposure
Increases in ambient temperature have been associated with skin rash flares, joint-related flares, and blood-related flares in individuals with SLE. High body temperature can also affect the immune system, potentially worsening lupus symptoms. While applying heat to painful areas (e.g., hot baths, warm towels) may offer some relief, there is no definitive evidence that heat therapy specifically treats lupus pain. Conversely, some individuals find that heat can exacerbate their symptoms.
Repeated exposure to low-level heat can damage skin vessels and pigment, leading to conditions like "toasted skin syndrome." Symptoms may include mild stinging, itchy skin, skin discoloration, a netlike or patchy rash, and changes in skin thickness. This can result from modern heat sources like heated blankets, heating pads, laptops, and space heaters.
Medications
Certain drugs can induce lupus-like skin reactions, a condition known as drug-induced lupus. While symptoms often improve after discontinuing the medication, the effects can sometimes persist.
Infections and Stress
Infections, physical stress, and hormonal changes can also trigger or worsen lupus symptoms.
Cigarette Smoking
Smoking is strongly linked to cutaneous lupus, increasing the risk of developing CLE and reducing treatment effectiveness. Chemicals in cigarettes may damage skin cells and worsen inflammation.
Immune System Responses
Both the innate and adaptive immune systems play a role in lupus. In CLE, the immune system mistakenly attacks healthy skin cells, causing chronic inflammation and rashes. Autoantibodies, which target the body's own tissues, contribute to the formation of rashes, redness, and swelling.
Managing Lupus Rashes and Skin Health
Effective management of lupus rashes involves a combination of medical treatment, lifestyle adjustments, and diligent skin care.
Medical Management
A healthcare provider, particularly a dermatologist specializing in medical dermatology or lupus, is essential for diagnosis and treatment. Diagnostic tools may include a skin biopsy for microscopic examination. It's crucial to distinguish lupus rashes from other conditions like drug reactions, allergies, eczema, or psoriasis for correct treatment. If a rash is diagnosed as lupus-related, treatment may involve topical steroids, antimalarials, or other medications prescribed by a rheumatologist or dermatologist. For chronic skin lesions, regular monitoring by a healthcare provider is recommended.
Sun Protection
Given the significant role of UV radiation, rigorous sun protection is paramount. This includes:
- Applying sunscreen with a high SPF (70 or higher) and broad-spectrum protection (Helioplex) daily, even on cloudy days.
- Wearing long-sleeved clothing, hats, and sunglasses when outdoors.
- Seeking shade and avoiding prolonged sun exposure, especially during peak UV hours.
- Being mindful of UV exposure from indoor sources like tanning beds and some artificial lighting.

Lifestyle Modifications
Lifestyle choices can significantly impact lupus symptoms:
- Diet: Following an anti-inflammatory diet rich in healthy fats, vegetables, and limited processed foods and added sugars may help. Avoiding trigger ingredients like alcohol, caffeine, and spices can also be beneficial.
- Stress Management: Employing stress-reducing techniques is important, as stress can trigger flares.
- Smoking Cessation: Quitting smoking is vital for overall health and can improve treatment outcomes for CLE.
- Temperature Regulation: Maintaining a comfortable home environment, using fans, and avoiding excessive heat can help. For individuals experiencing warmth due to inflammation or vasculitis, applying skin-safe gel packs may provide relief, but consultation with a healthcare provider is advised.
Addressing Specific Symptoms
Hair Loss: Hair loss in lupus is often characterized by dry, brittle hair that breaks. While treatments like topical steroids and minoxidil (Rogaine) may be prescribed, hair loss resulting from scarring discoid lesions can be permanent.
Raynaud's Phenomenon: This condition causes blood vessels in the fingers and toes to constrict, especially in cold temperatures, leading to discoloration and potential ulceration. Wearing gloves and socks in cool weather and avoiding caffeine and cigarettes are important preventive measures.
Skin Infections: Immunosuppressive medications used for lupus can increase the risk of skin infections. Signs of infection include swelling, pus, and pain. Prompt medical attention is necessary if an infection is suspected.
Precancerous and Cancerous Changes: In rare cases, long-term or repeated heat exposure can lead to precancerous or cancerous skin changes. Any thickened areas, sores, or lesions that do not improve after removing the heat source should be evaluated by a healthcare provider.
Lupus: Symptoms, Risk factors, Pathophysiology, Diagnosis and Treatments.
It is crucial for individuals with lupus to maintain open communication with their healthcare providers about any new or changing symptoms, including rashes or lesions that feel hot, to ensure timely and appropriate medical advice and treatment.