Pharmacists frequently encounter questions regarding the treatment of minor medical conditions, such as tinea pedis, commonly known as athlete's foot. Occasionally, patients may require confirmation that they indeed have the condition. Dermatophytes are a class of keratinophilic cutaneous fungal organisms that subsist on the stratum corneum, the outermost dead layer of skin, as well as hair, fingernails, and toenails. These mycoses are typically unable to survive on unkeratinized, living layers of skin and mucous membranes. Like other dermatophytes, the organisms responsible for tinea pedis thrive optimally in warm, moist areas, such as intertriginous skin (areas that are often or constantly in contact with other skin). Consequently, this common dermatophytic skin infection often affects the areas between the toes.
Tinea pedis is more prevalent in adults aged 15 to 40 years than in other age groups and tends to affect males more than females. A significant epidemiologic risk factor is the use of communal bathing facilities, which makes individuals who use them prime targets. Another epidemiologic factor involves footwear choices. While some individuals who walk on contaminated surfaces may escape the condition, others experience its uncomfortable symptoms. After the fungus reaches target tissues, it requires optimal warmth and humidity to fully begin infecting the host. Research has also identified pet ownership as a risk factor for tinea pedis. In these instances, the pet harbors fungal organisms (e.g., *M. canis*) capable of existing on human tissues, and normal human-pet interactions facilitate transmission to the owner. Many owners deny that their pet is the cause, believing that an infected pet would exhibit visible signs of infection, such as large patches of hair loss.
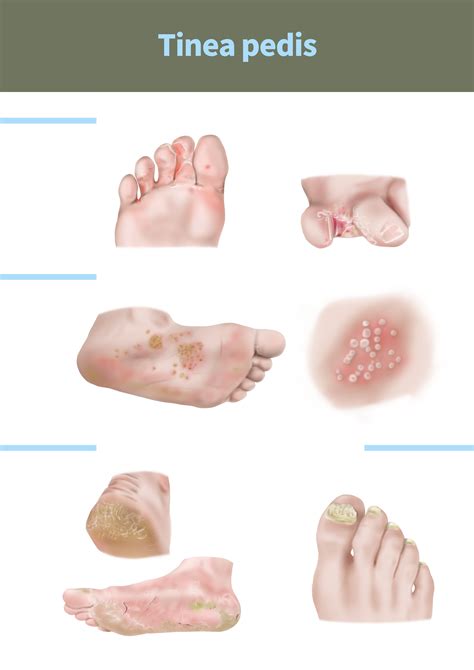
When pharmacists address questions about potential tinea pedis, it is crucial to be aware of the condition's visible signs and symptoms to fully and effectively assist the patient. Tinea pedis most often begins on the smallest toe or in the groove between the fourth and fifth toes, so these areas should be examined first. The reason for this geographic predilection is that the fifth toe is most likely to be overcrowded in tight shoes or sneakers, and its continuous close proximity to the fourth toe prevents the interdigital toe web from drying as thoroughly as other surfaces of the foot. Moisture accumulation and maceration create ideal conditions for the organisms to proliferate following implantation. The most common category is known as interdigital tinea pedis. In this type, the skin between the patient's toes (most often the fourth and fifth) begins to itch and break down.
Tinea pedis can also present as a second form, known as acute vesiculobullous infection. Foul odor and intense pruritus are also present. The lesions include vesicles and pustules; inflammation and fissuring are also prominent. The third form of tinea pedis is the moccasin type, most often caused by anthropophilic fungi transmitted from person to person. The patient notices fine scaling over the plantar surface, but there are no vesicles, and symptoms may be absent. The name is justified, as the preferential locations (plantar surface, heel, and sides of the foot) are those covered by a moccasin.
The pharmacist should also inquire if one or both hands have started to appear red, dry, or scaly. This is common in patients who habitually attempt to alleviate the pruritus of tinea pedis by scratching, thereby transferring the tinea to the hand. This condition, known as tinea manuum, may be present on both hands but is more common on just one hand, a condition referred to as "two-foot, one-hand" syndrome. Pharmacists often note that tinea pedis is accompanied by toenail infection, a condition known as tinea unguium or onychomycosis. Toenails infected with tinea frequently appear brittle, opaque, yellow, thickened, and crumbled. Infection of the nails may be the reason for persistent tinea pedis, as the organisms remain there to spread when conditions permit. Nonprescription products are unable to treat this condition.
Nonprescription Treatment Generations for Tinea Pedis
Tinea pedis can be treated with topical or systemic prescription therapies. Nonprescription treatment of tinea pedis is categorized into three generations, with succeeding products offering significant advantages. The first generation includes clotrimazole (e.g., Cruex Cream, Lotrimin AF Cream); miconazole (e.g., Cruex Spray Powder, Desenex Powder, Lotrimin AF Powder, Micatin Spray Liquid); and tolnaftate (e.g., Lamisil AF Defense Powder, Tinactin Cream and Spray). These are indicated for patients aged 2 years and above. Patients are instructed to apply the product twice daily, and treatment must continue for 4 weeks. The product labels state that they will cure tinea pedis but do not indicate any difference in efficacy among the three subtypes. These imidazole compounds are not fungicidal, as they only interrupt the development of the membrane of growing fungal cells. Thus, they are only bacteriostatic, which accounts for their relatively long application time.
The second generation of over-the-counter (OTC) antifungals for tinea pedis contains two ingredients: topical butenafine and terbinafine. Butenafine is a synthetic fungistatic/fungicidal benzylamine, and terbinafine is a fungicidal allylamine. These products warrant separate consideration because they promise cures in a shorter duration and are not safe for patients under 12 years of age. Butenafine (e.g., Lotrimin Ultra Cream) can cure tinea pedis between the toes (e.g., the interdigital form) in just 1 week if used twice daily, or in 4 weeks if the patient uses it only once daily. Therefore, the pharmacist should urge the patient to apply the product each morning and night. Butenafine is not known to be effective if the patient has tinea pedis on the bottom and sides of the feet (i.e., moccasin type).
Topical terbinafine (e.g., Lamisil AT Cream, Spray Pump, Solution) can cure tinea pedis between the toes when used twice daily for 1 week. The newest generation of nonprescription tinea pedis products contains only one ingredient: terbinafine in a gel dosage form (e.g., Lamisil AT Gel). This product can also cure tinea pedis between the toes in patients aged 12 years and above, but it is in a separate class because the gel requires only once-daily application to achieve a cure in 1 week.
Comparing Miconazole Nitrate and Tolnaftate
Both miconazole nitrate and tolnaftate are established topical antifungal agents commonly used as first-generation treatments for tinea pedis. They are available over-the-counter and are indicated for patients aged 2 years and older. Treatment typically requires application twice daily for a duration of 4 weeks.
Mechanism of Action
Miconazole nitrate belongs to the imidazole class of antifungals. It works by inhibiting the synthesis of ergosterol, a critical component of the fungal cell membrane. This disruption leads to increased membrane permeability and ultimately cell death. Tolnaftate, on the other hand, is a synthetic thiocarbamate. Its mechanism of action is distinct from azoles; it is thought to inhibit squalene epoxidase, an enzyme involved in the biosynthesis of ergosterol. This inhibition also disrupts fungal cell membrane integrity and function.
Efficacy and Treatment Duration
While both miconazole and tolnaftate are considered effective for treating tinea pedis, clinical studies suggest variations in their cure rates. The Cochrane Database of Systematic Reviews reported a 47% cure rate for azoles (including miconazole) and a 64% cure rate for tolnaftate in placebo-controlled trials. Both agents generally require a treatment duration of 2 to 4 weeks of twice-daily application.
Cost and Availability
A significant advantage of both miconazole and tolnaftate is their affordability and widespread availability as over-the-counter products. They are often considerably less expensive than newer generation antifungals, making them accessible treatment options for many patients.
Limitations
It is important to note that these first-generation antifungals are generally considered fungistatic, meaning they inhibit fungal growth rather than killing the fungi outright. This fungistatic action contributes to the longer treatment durations required for their efficacy. Furthermore, they are not typically effective for more extensive infections, such as tinea unguium (onychomycosis), or for severe cases of tinea pedis, which may necessitate prescription-strength topical or oral antifungal medications.

Prevention of Tinea Pedis
Pharmacists can provide valuable advice on preventing tinea pedis. Patients should keep their feet dry and clean, drying them thoroughly (especially between the toes) before putting on socks and shoes. They should go barefoot whenever possible to allow for thorough drying and be encouraged to wear rubber sandals when walking in communal bathing facilities or any location where people have walked barefoot. If a toenail becomes infected, prompt medical attention is necessary to prevent the spread of infection to the surrounding skin. Finally, if patients develop tinea in another part of the body, they must take great care to prevent transferring it to the foot (e.g., by washing and drying that part of the body with separate cloths).
Athlete's foot, also known as tinea pedis, is a fungal infection that can appear in several forms. Perhaps you have noticed the area between your fourth and fifth toes has become infected, with fissures, cracking, and a wet look and feel, with whitening and/or thickening of the skin. Itching may be so severe that it requires almost constant scratching. You may notice that other spots on the foot are involved as well. Perhaps the sole and sides of the foot are affected with small blisters, scaling, swelling, and open cracking. Your toenails appear white or brittle, with crumbling and cracking of the nail. The nail may even lift up from its nail bed. Finally, tinea pedis that is not cured tends to be less intense during the winter and may seem to almost disappear.
There are many noninfective conditions that affect the foot, such as psoriasis and poison ivy. If you are unsure whether your problem is athlete's foot (i.e., symptoms differ markedly from those previously explained), you should visit a physician. Your pharmacist may also be able to recognize the presence of athlete's foot. Once athlete's foot is confirmed, you may treat the problem with nonprescription products. Generally, OTC products are safer than prescription products, as they have fewer side effects. Your pharmacist can provide full counseling information on treatment options for athlete's foot. You must read the labels carefully and follow all directions provided.
Several over-the-counter antifungal creams are effective in treating athlete's foot. These include clotrimazole, terbinafine, miconazole, econazole, and tolnaftate. When choosing an antifungal cream for athlete's foot, consider factors such as the severity of your symptoms, any allergies or sensitivities you may have, and whether you prefer a specific formulation (cream, gel, spray, etc.).
5 Ways to Cure Athlete’s Foot (That Actually Work)
It is important to consult your podiatrist or healthcare professional before using any medication or treatment for this condition. Podiatrists play a crucial role in the diagnosis and treatment of athlete's foot. They can provide accurate diagnoses through physical examination and laboratory analysis, prescribe appropriate medications based on the severity and type of infection, and create customized treatment plans. Foot and ankle specialists also educate patients on proper foot hygiene practices, monitor treatment progress, and offer preventive strategies to reduce the risk of future fungal infections.
tags: #miconazole #nitrate #vs #tolnaftate