When considering treatment options for skin conditions, it's crucial to understand the nature of the infection. While some individuals may consider using leftover medications, this approach is generally not recommended due to potential risks and the importance of accurate diagnosis. This article aims to clarify the role of clindamycin in treating skin conditions, particularly in relation to ringworm, and to provide information on appropriate antifungal treatments.
Understanding Ringworm
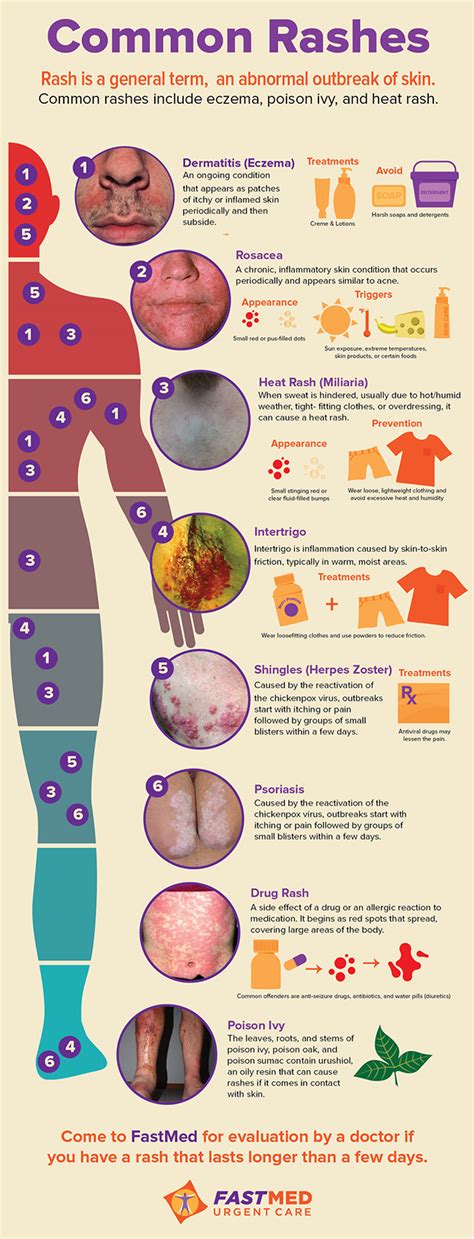
Ringworm, medically known as tinea, is a fungal infection, not a bacterial one. This distinction is fundamental when selecting the correct treatment. Symptoms can include circular, itchy rashes, often with raised edges. The duration and severity can vary, with some cases persisting for months.
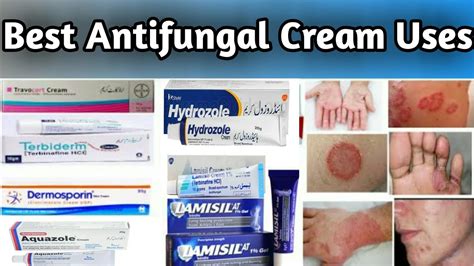
A common course of treatment for ringworm involves antifungal medications. These can be in the form of topical creams, gels, lotions, or powders applied directly to the skin. Examples of commonly prescribed topical antifungals include:
- Butenafine (Mentax)
- Ciclopirox (Loprox)
- Econazole
- Clotrimazole (Mycelex)
- Terbinafine (Lamisil)
For more persistent or widespread infections, or for ringworm affecting the scalp, oral antifungal medications may be prescribed. These are typically taken for a longer duration, often one to three months.
What is Clindamycin?
Clindamycin is an antibiotic belonging to the lincosamide class. It is primarily used to treat bacterial infections. Clindamycin exhibits a broad spectrum of antimicrobial activity, including against Gram-positive aerobes and anaerobes, Gram-negative anaerobes, and certain protozoa. It is available in various forms, including topical solutions, gels, lotions, and foams, as well as oral and intravenous formulations.
Topical clindamycin is often prescribed for the treatment of acne, where it helps to control bacterial growth contributing to breakouts. It may be used alone or in combination with other acne treatments.
Forms of Topical Clindamycin
Clindamycin is available in several topical dosage forms:
- Foam
- Solution
- Lotion
- Pad
- Gel/Jelly
When Clindamycin Might Be Used for Skin Issues
While clindamycin is not a direct treatment for fungal infections like ringworm, it may be considered in cases where a secondary bacterial infection complicates the fungal rash. If the affected area shows signs of bacterial infection, such as increased redness, warmth, pus, or pain, an antibiotic like clindamycin might be prescribed by a healthcare professional. However, it is essential that this is determined by a doctor, as using antibiotics inappropriately can lead to resistance and other complications.
Why Clindamycin is Not for Ringworm
The core reason clindamycin is not suitable for treating ringworm is that ringworm is caused by fungi, and clindamycin is an antibiotic that targets bacteria. Antifungal medications work by killing or inhibiting the growth of fungi, while antibiotics target bacteria. Using an antibiotic for a fungal infection will not be effective and could potentially worsen the condition or lead to the development of resistant microorganisms.
Potential Risks and Side Effects of Clindamycin
Like all medications, clindamycin can have side effects. It is crucial to use it only as prescribed by a healthcare professional.
Important Precautions Before Using Clindamycin:
- Allergies: Inform your doctor about any history of allergic reactions to clindamycin or other medications, foods, dyes, preservatives, or animals.
- Pediatric Use: Studies are primarily conducted on adults; use in children should be guided by a doctor.
- Geriatric Use: While generally not expected to cause different side effects in older adults, individual responses may vary.
- Breastfeeding: Adequate studies in women are lacking; potential benefits should be weighed against risks.
- Drug Interactions: Clindamycin can interact with various medications. It is vital to inform your doctor about all medications you are taking, including those listed as not recommended or usually not recommended for use with clindamycin (e.g., certain antifungals like ketoconazole and fluconazole, and other antibiotics like erythromycin).
- Other Medical Problems: Inform your doctor about any pre-existing conditions, especially stomach or intestinal diseases like colitis, as these can increase the risk of certain side effects.
Common Side Effects:
When used topically, common side effects may include:
- Dryness, scaliness, or peeling of the skin (especially with the solution form)
- Stinging or burning feeling of the skin
- Skin irritation or oiliness
- Headache
- Mild diarrhea
Serious Side Effects:
Less common but serious side effects include:
- Severe abdominal or stomach cramps, pain, and bloating
- Watery and severe diarrhea, which may also be bloody
- Fever
- Nausea or vomiting
- Unusual tiredness or weakness
- Unusual weight loss
Severe diarrhea can be a sign of pseudomembranous colitis, a serious condition caused by an overgrowth of the bacterium Clostridium difficile. If significant diarrhea develops, the drug should be stopped, and medical advice sought immediately.
Topical Medication Application- Nursing Skills
Self-Medication and Over-the-Counter (OTC) Treatments
Self-medicating with leftover prescriptions or using unverified treatments is strongly discouraged. It is essential to obtain a proper diagnosis from a healthcare professional to ensure the correct treatment is administered. For ringworm, over-the-counter antifungal medications are often effective for milder cases on the skin, such as athlete's foot (tinea pedis) and jock itch (tinea cruris). However, it is always advisable to consult a healthcare provider even for these conditions to confirm the diagnosis and receive guidance.
Important Note: Avoid using over-the-counter creams containing steroids (corticosteroids) for ringworm or undiagnosed rashes. Corticosteroids can weaken the skin's ability to fight fungal infections, potentially making the ringworm worse and spreading it to other parts of the body. They can also mask symptoms, making diagnosis more difficult.
When to Seek Medical Advice
It is recommended to consult a healthcare provider for any suspected ringworm, even if over-the-counter treatments are available. A healthcare professional can accurately diagnose the condition, differentiate it from other skin issues, and recommend the most effective treatment plan. If a prescribed treatment, such as topical antifungals or oral medications, does not show improvement within a reasonable timeframe (e.g., 6 weeks for topical acne treatments, though ringworm treatment durations vary), or if the condition worsens, medical advice should be sought promptly. Travel history should also be discussed with a healthcare provider, as certain types of ringworm have been reported to spread in different regions.
tags: #clindamycin #for #ringworm