Fungal nail infections, medically known as onychomycosis, are a common condition affecting millions worldwide. While often perceived as a cosmetic concern, these infections can lead to discomfort, embarrassment, and pain that impacts daily life. Fungus thrives in warm, damp environments, making shoes and public places like locker rooms and swimming pools common breeding grounds.
The fungus grows underneath or within the nail, causing it to become thickened, brittle, and discolored over time. Fortunately, several over-the-counter (OTC) antifungal treatments are available to help manage mild to moderate infections and improve nail health.
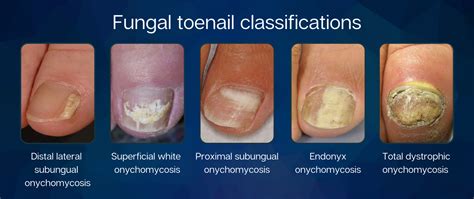
Understanding OTC Antifungal Nail Treatments
OTC antifungal nail treatments work by targeting the fungus responsible for the infection. The key to success with these treatments is consistency and early intervention. For OTC treatments to be most effective, it's recommended to start them at the first signs of infection, when it affects less than 50% of the nail surface and is not severely thickened.
A crucial step in any antifungal nail care regimen is proper preparation. Always begin by thoroughly cleaning and drying the affected area. Filing the nail surface can create microscopic channels, allowing topical treatments to penetrate deeper into the nail plate where the fungus resides, significantly improving their effectiveness.
Popular OTC Ingredients and Products
Several FDA-approved ingredients are commonly found in OTC antifungal toenail treatments. The most effective OTC ingredient for toenail fungus is undecylenic acid. It works by penetrating the nail plate and inhibiting fungal cell growth, acting as a fungistatic agent that prevents the spread of the fungus.
Other commonly used ingredients and products include:
- Undecylenic Acid: Available as a liquid or polish, it's the main ingredient in many OTC products and eases irritation associated with fungal infections. It is typically applied daily for 4-12 months, with success rates ranging from 40-60% for mild to moderate infections.
- Terbinafine (Lamisil): One of the most effective OTC choices, it targets the fungal cell membrane to stop growth. It's available in various forms like creams, gels, sprays, or powders.
- Clotrimazole (Lotrimin): Often recommended for mild infections, it stops fungal growth by disrupting the fungal cell structure. It's found in many OTC yeast infection creams and has shown effectiveness in trials.
- FungiCure (Undecylenic Acid): Specifically designed to stop fungal growth on nails and surrounding skin, it is best suited for mild infections.
- Kerasal Fungal Nail Renewal: This product works by softening thickened nails with urea and salicylic acid, which allows antifungal medications to penetrate more effectively, rather than killing the fungus directly.
- Tea Tree Oil: Derived from an Australian tree, it exhibits antifungal properties in laboratory studies and shows a clinical success rate of 20-30%. However, its effectiveness is limited by poor nail penetration compared to pharmaceutical treatments.
- Vicks VapoRub: While not a traditional antifungal, the camphor, eucalyptus oil, and menthol in Vicks are believed to possess mild antifungal properties. Some small studies suggest it may be effective for some individuals.
- Snakeroot Extract: Derived from a plant, this natural remedy has shown results comparable to ciclopirox, a prescription medication for fungal skin infections.
- Baking Soda: Sodium bicarbonate has demonstrated the ability to limit the growth of common fungi in laboratory settings.
- Ozonized Sunflower Oil: Emerging research indicates promise for this natural remedy against yeasts that cause foot fungus, though more clinical evidence is needed.

Application and Best Practices
Applying antifungal nail treatments consistently is paramount for achieving results. Most treatments should be applied daily to the affected nail and surrounding skin. The duration of treatment can vary significantly, often requiring 4 to 12 months, or even longer, as it depends on the natural growth cycle of the nail.
Key practices for maximizing effectiveness include:
- Clean and Dry Thoroughly: Always ensure the affected area is clean and completely dry before application.
- File the Nail Surface: Gently filing the nail surface can improve penetration of topical treatments.
- Regular Application: Missing applications can significantly delay results. Adhere to the product's instructions for daily use.
- Trim and Thin Nails: Regularly trimming and thinning thick nails can reduce pressure and pain, and help treatments penetrate better. Soften nails with urea-containing creams before trimming or thinning.
It is important to note that toenails grow approximately 1mm per month, meaning complete fungus elimination requires the full replacement of the nail.
When to Seek Professional Help
While OTC treatments can be effective for mild to moderate infections, they are not always sufficient. If your infection does not improve after several weeks of consistent treatment, or if you experience increased pain, swelling, redness, or discharge, it is essential to consult a healthcare professional, such as a podiatrist.
A podiatrist can accurately diagnose the condition, as other nail disorders like psoriasis can mimic fungal infections. They can perform laboratory tests on nail clippings or scrapings to confirm the presence of fungus and identify the specific type. This ensures the most appropriate treatment plan is initiated.
Signs that warrant professional evaluation include:
- No improvement after 3 months of OTC treatment.
- Infection affecting multiple nails.
- Severe thickening, pain, or discoloration of the nail.
- Underlying health conditions such as diabetes, poor circulation, or a weakened immune system.
- The nail is painful or lifting from the nail bed.
- Recurrent athlete's foot or skin infections around the nail.
Professional Treatment Options
For more severe or persistent fungal nail infections, a podiatrist may recommend or prescribe:
- Prescription Oral Antifungal Medications: Drugs like terbinafine or itraconazole are often considered first-line treatments. They work systemically, delivering medication directly to the nail matrix for higher cure rates. However, they can have side effects and may require medical monitoring.
- Prescription Topical Nail Products: Medications such as efinaconazole, tavaborole, or ciclopirox are available as medicated nail polishes or creams. These are typically used for mild to moderate infections and require daily application for many months.
- Laser Therapy: This treatment uses focused light to heat and destroy fungal organisms in the nail bed without damaging surrounding tissue. It usually requires several sessions.
- Combination Therapy: In some cases, a combination of oral and topical treatments, along with regular nail debridement, may be recommended to improve outcomes.
While professional treatments may have a higher upfront cost, they often achieve faster results and higher cure rates compared to OTC options, typically within 3-6 months.
Preventing Reinfection
Preventing reinfection is a critical aspect of managing fungal nail conditions. Fungal spores can survive in shoes and socks, leading to reinfection even after successful treatment.
Strategies to prevent reinfection include:
- Treating Athlete's Foot: Athlete's foot (tinea pedis) is a skin fungus that can spread to the nails or keep reinfecting them. Treating this condition is crucial.
- Shoe Hygiene: After completing treatment, consider replacing footwear or treating existing shoes with antifungal sprays or UV sanitizers.
- Keep Feet Dry: Wear breathable footwear and change socks regularly, especially if your feet tend to sweat.
- Avoid Walking Barefoot: In public places like gyms or swimming pools, wear protective footwear.
What are the Best Treatments for Fungal Toenails - Seattle Podiatrist Larry Huppin
Comparing OTC and Prescription Costs
The cost of treating fungal nail infections can vary significantly between OTC and prescription options. While OTC treatments are less expensive initially, they require continuous purchase over a prolonged period (12-18 months), which can add up.
Prescription medications may have a higher upfront cost but often lead to faster results, potentially reducing the overall duration and cost of treatment. Calculating the total cost over the expected treatment duration is advisable when comparing options.
tags: #otc #antifungal #toenail