Tinea versicolor, also known as pityriasis versicolor, is a common fungal infection of the skin. It is caused by an overgrowth of a type of yeast (fungus) that is naturally found on the skin. This condition disrupts normal pigmentation, leading to the development of discolored patches on the skin.
What Causes Tinea Versicolor?
The underlying cause of tinea versicolor is the excessive growth of a yeast, typically from the genus Malassezia, which is a normal inhabitant of the skin's flora. While this yeast is present on healthy skin, certain factors can trigger its overgrowth.
Factors Contributing to Yeast Overgrowth:
- Hot and Humid Climates: These conditions create an environment conducive to fungal growth.
- Oily or Sweaty Skin: Excessive sebum production can promote yeast proliferation.
- Weakened Immune System: Conditions or medications that suppress the immune system can make individuals more susceptible.
- Hormonal Changes: Pregnancy and puberty, periods of significant hormonal fluctuation, can increase susceptibility.
- Genetic Predisposition: Some individuals may have a hereditary tendency to develop the condition.
- Certain Medical Conditions: Diabetes and conditions requiring corticosteroid use are associated with increased risk.
The exact reasons why the yeast overgrows on some people's skin and not others remain unclear, but these factors are believed to play a significant role.
Symptoms and Appearance of Tinea Versicolor
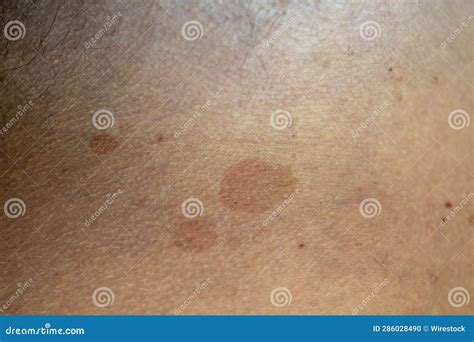
Tinea versicolor typically manifests as small, round patches on the skin that are either lighter or darker than the surrounding skin. These patches can vary in color and appearance.
Key Symptoms and Visual Characteristics:
- Discolored Patches: The most common symptom is patches of skin that are lighter (hypopigmented), darker (hyperpigmented), pink, red, tan, or yellow compared to normal skin tone.
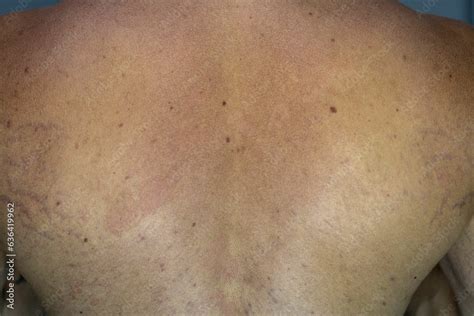
- Location: These patches most often occur on the chest, back, neck, and upper arms.
- Texture: The patches may appear dry and scaly.
- Sun Exposure Effect: The affected areas do not tan normally in the sun, making the discolored patches more noticeable, especially during warmer months.
- Mild Itching: Some individuals may experience mild itching, particularly when they become hot or sweaty.
The appearance of the patches can differ based on skin color. On darker skin, tinea versicolor often appears lighter, while on lighter skin, it may look pink or light red. The patches can enlarge and merge to form larger areas over time.
Diagnosis of Tinea Versicolor
Healthcare professionals can often diagnose tinea versicolor based on its characteristic clinical appearance. However, further tests may be used to confirm the diagnosis.
Diagnostic Methods:
- Physical Examination: A visual inspection of the skin is usually the first step.
- Wood's Lamp Examination: An ultraviolet light, known as a Wood's lamp, may be used. In some cases, tinea versicolor lesions can fluoresce with a yellow-green or coppery-orange hue under this light, although this is not always present.
- Skin Scraping: A healthcare provider may gently scrape the surface of the skin with a small tool to collect skin cells. These cells are then examined under a microscope, often after being treated with potassium hydroxide (KOH). The classic microscopic finding resembles "spaghetti and meatballs" due to the presence of yeast cells and hyphae.
- Skin Biopsy: In rare cases, if the diagnosis is uncertain, a small sample of skin tissue may be removed for laboratory testing.
Treatment for Tinea Versicolor
Tinea versicolor is treatable, and the goal of treatment is to eliminate the overgrowth of the fungus. Treatment options range from over-the-counter products to prescription medications.
Topical Antifungal Treatments:
Topical medications are typically the first line of treatment for tinea versicolor. These are applied directly to the skin.
- Antifungal Shampoos: Shampoos containing ingredients like selenium sulfide (2.5%) or ketoconazole (2%) are highly effective. They are usually applied over the entire body in the shower, left on for a few minutes, and then rinsed off. They may be used daily for a week or weekly for a month.
- Antifungal Creams, Lotions, and Soaps: Over-the-counter options like clotrimazole cream or medicated soaps (e.g., pyrithione zinc soap 2%) can be used for mild cases. Prescription-strength topical azoles (e.g., ketoconazole 2% cream) may also be prescribed.
Oral Antifungal Medications:
Oral antifungal medications are generally reserved for cases that are widespread, resistant to topical treatments, or frequently recurrent.
- Fluconazole: Often taken orally for 2 to 4 weeks.
- Itraconazole: Typically prescribed at a dose of 200 mg daily for 5 to 7 days, or 200 mg weekly for 2 weeks for recurrent cases.
It is important to note that oral terbinafine and griseofulvin are generally not effective for tinea versicolor. Oral ketoconazole, while effective, carries risks of hepatotoxicity and drug interactions, making it a less preferred option.
Patchy, Discolored Rash on the Body? How to Treat Tinea Versicolor like a Dermatologist
Preventing Recurrence
Tinea versicolor has a high rate of recurrence because the causative fungus is a normal part of the skin's flora. Preventive measures can help reduce the likelihood of the infection returning.
Preventive Strategies:
- Regular Use of Antifungal Shampoos: Once the infection has cleared, using an antifungal shampoo (like selenium sulfide or ketoconazole) once a month for several months, especially during warm weather, can help prevent recurrence.
- Good Hygiene: Maintaining good personal hygiene, especially in hot and humid conditions.
- Avoiding Oily Products: Limiting the use of oily lotions and creams, particularly on the trunk and upper body.
Even with successful treatment, the discoloration of the skin may persist for several weeks or months as the skin gradually returns to its normal color.
Differential Diagnosis
It is important to differentiate tinea versicolor from other skin conditions that may present with similar symptoms. Some of these include:
- Seborrheic dermatitis
- Pityriasis rosea
- Erythrasma
- Pityriasis alba
- Vitiligo
- Secondary syphilis
- Confluent reticulated papillomatosis
- Guttate psoriasis
- Mycosis fungoides
- Terra firma-forme dermatosis
A KOH preparation from skin scrapings is crucial in distinguishing tinea versicolor from these other conditions.
tags: #tinea #versicolor #specialists