Human papillomavirus (HPV) is a prevalent viral infection that affects the skin and mucous membranes. Classified into over 200 types based on genome sequencing, HPV can manifest in various ways, from subclinical infections to visible lesions known as warts.
While non-sexually acquired HPV can affect the skin, certain types of HPV are primarily transmitted sexually and can cause genital warts. These infections are widespread, and understanding their transmission, particularly the potential for transmission to the face, is crucial for prevention and management.
What are Genital Warts?
Genital warts are one of the most common types of sexually transmitted infections (STIs), caused by specific types of the human papillomavirus (HPV). These warts typically appear on the skin around the genitals and anus. They affect the moist tissues of the genital area and can vary in appearance, ranging from small, skin-colored bumps to lesions resembling cauliflower. Some strains of genital HPV can cause warts, while others are considered "high-risk" and can lead to cancer if left untreated.
The warts can be so small and flat that they are not always visible. While some strains of HPV that cause genital warts are considered "low-risk" and do not lead to cancer, it is important to be aware of the different types and their potential implications.
Transmission of Genital Warts
Genital warts are almost always spread through sexual contact, involving skin-to-skin or mucous membrane-to-mucous membrane contact with an infected person. This can occur during vaginal, anal, or oral sex.
Key aspects of genital wart transmission include:
- Skin-to-skin contact: Transmission occurs through direct contact with infected skin, even if no visible warts are present. This is less common but still possible.
- Sexual activities: Vaginal, anal, and oral sex are the primary modes of transmission.
- Asymptomatic shedding: The virus can be spread even when the infected person does not have any visible warts or other symptoms, although this is less common.
- Duration of infection: Symptoms may appear years after the initial sexual contact with an infected person.
- Contagiousness: You are more likely to spread genital warts when you are experiencing symptoms, such as visible warts.
Can Genital Warts Transmit to the Face?
While genital warts themselves are typically confined to the genital and anal regions, the underlying HPV infection can potentially spread to other areas of the body, including the face, through different transmission routes.
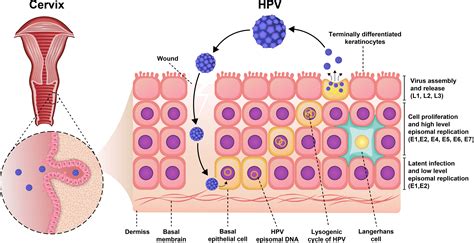
The human papillomavirus (HPV) reproduces itself in human epithelial cells. HPV types that cause genital warts and anogenital cancers infect epithelial cells lining mucosal surfaces. The virus remains in the area of the original infection and does not travel through the bloodstream to cause infections at distant sites. However, viral particles are released as infected cells die and slough off at mucosal epithelial surfaces. This process, combined with intimate interactions, makes transmission likely.
Transmission to the face is not a direct spread from genital warts but rather through contact with the virus. This can occur via:
- Auto-inoculation: If an individual with genital warts touches the warts and then touches their face without proper hand hygiene, they can transfer the virus.
- Oral sex: While oral sex primarily transmits HPV to the mouth and throat, if there are concurrent skin-to-skin contacts involving the face, transmission is theoretically possible, though less common for visible warts.
- Sharing personal items: Although less common, sharing items that come into contact with infected skin, such as towels or razors, could potentially lead to transmission if not properly cleaned.
It is important to distinguish between common warts (verruca vulgaris) and genital warts. Common warts, which often appear on hands, feet, and knees, are caused by different HPV types than those that cause genital warts. However, the principle of skin-to-skin transmission applies to all wart types.
Types of Warts and Their Characteristics
HPV infections of the skin can present with clinical lesions, commonly known as warts. These can be classified based on their location and appearance:
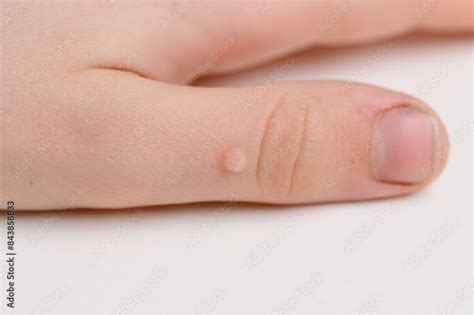
- Common viral warts (verruca vulgaris): These affect keratinized skin, particularly on the hands, feet, and knees. They are typically dome-shaped, circumscribed, hyperkeratotic, and verrucous papules and nodules.
- Plantar warts (verruca plantaris): Found on the soles of the feet, these present as a thickening with a loss of surface skin lines. Paring them down reveals multiple pinpoint bleeding spots of patent papillary capillaries or black dots of thrombosed capillaries.
- Subungual and periungual warts: These affect the nail plate and the surrounding skin.
- Filiform warts: Characterized by a narrow base and fine, elevated keratotic fronds.
Epidermodysplasia verruciformis is a rare genetic disorder that increases susceptibility to specific HPV types, carrying a higher risk of HPV-related cutaneous squamous cell carcinoma (SCC).
Diagnosis and Histology
A skin biopsy may be required for diagnosis, especially in cases where a lesion is suspicious for squamous cell carcinoma, such as in organ transplant recipients. Warts exhibit characteristic features on histology.
Treatment of HPV Infections and Warts
Treating cutaneous manifestations of HPV infections can be challenging. Various treatment modalities are available:
- Over-the-counter treatments: Paints and pastes containing salicylic acid, podophyllin, and other ingredients are often the first line of treatment for common warts.
- Cryotherapy: This involves applying liquid nitrogen to freeze and destroy the wart. It is a common treatment performed by doctors and often requires multiple applications. To be effective, cryotherapy should induce a blister and include a rim of normal-looking skin, as the virus may have already spread to adjacent areas.
- Topical medications: Prescription chemical solutions or creams can be applied to the warts, causing blisters to form underneath and cutting off blood supply.
- Surgery: Warts can be surgically cut out, especially if they are large or do not respond to other treatments. This may involve local anesthesia.
- Laser treatment: This method uses laser light to destroy blood vessels within the warts.
- Electrocautery: An electric current is used to burn away warts.
- Loop electrosurgical excision procedure (LEEP): This procedure uses an electrically charged wire loop to remove warts, particularly effective for warts on the cervix.
It is important to note that treatment for genital warts does not cure the HPV infection itself. The warts may come back even after successful removal because the virus can remain dormant in the body. Some treatments, like certain creams, can weaken condoms and vaginal diaphragms, necessitating careful discussion with a healthcare provider.
What are warts (HPV)? - 3D animation
Prognosis and Spontaneous Resolution
Cutaneous warts caused by non-sexually acquired HPV often resolve spontaneously in the majority of children within two years. In adults, warts tend to resolve more slowly and may take several years. Recurrence of warts in adjacent skin after treatment is common due to subclinical or latent infection.
Genital warts and the HPV infection can be lifelong. Even with treatment to remove visible warts, they may reappear. While genital warts themselves do not turn into cancer, certain high-risk HPV strains can lead to various cancers, including cervical, vulvar, vaginal, penile, anal, and oropharyngeal cancers. Regular screening, such as Pap tests for cervical cancer, is crucial for early detection and management of HPV-related health issues.
Prevention
Prevention is a key strategy in managing HPV infections and related conditions:
- HPV Vaccination: The HPV vaccine is safe and effective in preventing diseases caused by HPV, including genital warts and certain cancers. Vaccination is recommended for both girls and boys at ages 11 and 12, with a two-dose schedule.
- Safe Sex Practices: Using condoms every time you have sex can lower your chances of getting HPV, but it does not offer complete protection as HPV can infect areas not covered by a condom. Limiting the number of sexual partners and having sex with a mutually monogamous partner also reduces risk.
- Hygiene: Practicing good hand hygiene after touching warts can help prevent auto-inoculation.
- Screening: Regular screening for cervical cancer is essential for women.
If you or your partner have genital warts, it is advisable to abstain from sexual contact until the warts are no longer present to reduce the chance of spreading the infection.