Comedonal acne is a common skin concern that many of us face, often starting in puberty and sometimes lingering longer than we’d like. These persistent bumps can be frustrating, but understanding their causes and treatments is key to achieving clear, radiant skin. In this guide, we will delve into the intricacies of comedonal acne, exploring its causes, how to identify it, and the most effective treatments. Let’s embark on this journey to healthier skin together.
What is Comedonal Acne?
Comedonal acne is a mild form of acne vulgaris characterized by the presence of comedones. These small, flesh-coloured bumps develop when hair follicles become clogged with sebum and dead skin cells. Comedonal acne is primarily non-inflammatory, distinguishing it from other types of acne that involve inflammation, such as papules or pustules. Comedones are the skin-coloured, small bumps (papules) frequently found on the forehead and chin of those with acne. Comedonal acne is a pattern of acne in which most lesions are comedones.
Types of Comedones
There are two main types of comedones:
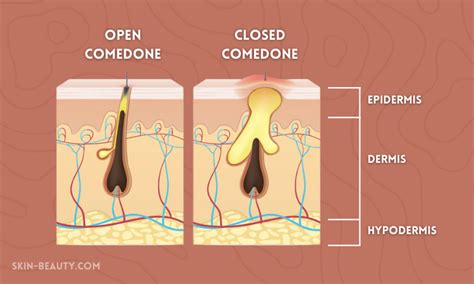
- Open comedones (blackheads): These appear as dark spots on the skin’s surface due to oxidation of the trapped sebum.
- Closed comedones (whiteheads): These present as small, flesh-coloured or slightly raised bumps beneath the skin’s surface. Closed comedones are small, white or skin-coloured bumps that form when a pore becomes blocked by oil and dead skin cells but stays sealed beneath the surface. They’re a type of comedonal acne that can make the skin feel uneven but are not usually sore or inflamed. Closed comedones develop when oil, dead skin cells and bacteria become trapped within a pore, covered by a thin layer of skin. Unlike blackheads, they aren’t open to the air, so they stay pale or flesh-coloured rather than turning dark.
In some cases, larger comedones known as macrocomedones may develop, which can be more challenging to treat. Microcomedones are the earliest stage of acne lesions and are not visible to the naked eye. Macrocomedones are closed comedones that are larger than 2 to 3 millimeters (mm) across. Microcomedones are usually not visible.
Common Areas Affected
Comedonal acne commonly affects the forehead, nose, and chin, but can occur on other areas of the face and body as well. The T-zone, which includes the forehead, nose, and chin, is particularly prone to comedone formation due to its higher concentration of sebaceous glands.
What Causes Comedonal Acne?
Comedones arise when cells lining the sebaceous duct proliferate (cornification), and there is increased sebum production. A comedo is formed by the debris blocking the sebaceous duct and hair follicle. Several factors can contribute to the development of comedonal acne.
Excess Sebum Production
Overactive sebaceous glands can lead to increased oil production, clogging pores and contributing to the formation of comedones. This excess sebum can combine with dead skin cells to form a plug in the hair follicle, leading to comedone development.
Hormonal Changes
Fluctuations in hormone levels, particularly during puberty, can stimulate sebum production. Androgens, such as testosterone, play a significant role in increasing sebum production, which can lead to the formation of comedones.
Environmental Factors and Lifestyle Habits
High humidity, exposure to certain irritants, and the use of comedogenic skincare or makeup products can exacerbate comedonal acne. Additionally, certain foods and dietary habits may influence acne development in some individuals, although the relationship between diet and acne is complex and varies from person to person. People who smoke are more likely to experience comedonal acne. Dietary factors can also contribute, such as consuming excess milk or sugar.
Genetic Predisposition
Some individuals may be more prone to developing comedonal acne due to their genetic makeup. If your parents or siblings have a history of acne, you may be more likely to experience it as well.
What Does Comedonal Acne Look Like?
Key characteristics of comedonal acne include:
- Small, flesh-coloured or slightly raised bumps on the skin.
- Blackheads, appearing as dark spots on the skin’s surface.
- Whiteheads, presenting as closed bumps beneath the skin.
- A rough or uneven skin texture.
- Predominantly non-inflammatory lesions.
Comedonal acne presents as many small papules, the same color as the surrounding skin, that make the skin appear bumpy. Types include whiteheads or closed comedones, blackheads, and open comedones. The appearance of comedonal acne is different from that of inflammatory acne. Comedonal acne involves blackheads and whiteheads rather than pimples. While this form can develop in anyone, it is most common in young adolescents. The papules, called comedones, usually occur on the forehead and chin and can prevent the skin from appearing smooth and even.
Differentiating Comedonal Acne from Other Types of Acne
Comedonal acne is primarily non-inflammatory, unlike other forms of acne such as inflammatory acne, which may include red, swollen lesions like papules or pustules. Comedonal acne focuses on the presence of comedones, while other types may involve more severe lesions or widespread inflammation. Comedonal acne does not usually contain pus or the bacteria that can cause acne. They also typically neither cause skin redness or other discoloration nor are tender to the touch. A person with comedonal acne may have more than one type of comedone at a time. Meanwhile, depending on their skin tone, people with inflammatory acne can also have comedones, in addition to larger red or discolored and tender blemishes. Comedonal acne also differs from other types because its lesions tend to be small. For example, nodular and nodulocystic forms of acne can cause larger, tender, fluid-filled lesions to form. Doctors usually consider comedonal acne to be a mild to moderate form of the condition.
How to Get Rid of Closed Comedones
If you have comedonal acne, choose oil-free cosmetics and wash twice daily with a mild soap and water. Choose "comedolytic" topical medications. These should be applied once or twice daily as a thin smear to the entire area affected. It may take several weeks to months before worthwhile improvement occurs.
Over-the-Counter Topical Treatments
Several effective over-the-counter options can help manage comedonal acne:
- Salicylic acid: This beta-hydroxy acid (BHA) helps exfoliate the skin and unclog pores.
- Benzoyl peroxide: While primarily known for its antibacterial properties, it can also help reduce comedones.
- Retinol: This vitamin A derivative promotes cell turnover and helps prevent the formation of microcomedones.
Prescription Medications
For more severe or persistent cases, a dermatologist may prescribe:
- Topical retinoids: Stronger vitamin A derivatives like tretinoin or adapalene can be highly effective in treating comedonal acne by promoting cell turnover and preventing clogged pores. A person will require a prescription for retinoids from a dermatologist or another healthcare professional because they can be more abrasive to the skin. After reviewing tolerance to various retinoids, it can be concluded that a person’s skin may respond best to an OTC adapalene gel sold as Differin.
- Topical antibiotics: These are not usually the first choice for treating comedonal acne, but they might be used if there’s a risk of bacterial infection.
- Oral medications: In some cases, oral antibiotics or hormonal treatments may be recommended to address underlying causes and reduce acne severity. Unlike inflammatory acne, comedonal acne does not usually respond well to antibiotics, isotretinoin pills, or hormonal medications that can manage breakouts, such as birth control pills.
Professional Treatments
In-office procedures can provide additional benefits:
- Chemical peels: Using acids like glycolic acid or salicylic acid to exfoliate the skin and unclog pores.
- Microdermabrasion: A technique that physically exfoliates the skin to remove dead skin cells and unclog pores.
- Comedone extraction: A procedure performed by a skincare professional to manually remove comedones. In some cases, a doctor may recommend an in-office treatment to close off comedones to help keep them from returning. These treatments include microdermabrasion, cryotherapy, and electrosurgery.
Establishing a Consistent Skincare Routine
Consistency is key when managing comedonal acne. Stick to a regular routine of cleansing, treating, and moisturising to keep your skin clear and healthy. Use oil-free, non-comedogenic makeup and skincare products to avoid clogging your pores. Preventing closed comedones is often about routine rather than strong treatments. Cleanse regularly, moisturise daily, and protect your skin with SPF. Closed comedones are common and nothing to worry about. With a gentle skincare routine that includes mild cleansing, light moisturising, and daily sun protection, most people can improve uneven skin texture and support smoother-looking skin over time.

What Skincare is Good for Comedonal Acne?
Incorporating a targeted anti-blemish skincare routine can significantly improve comedonal acne. Look for mild, fragrance-free skincare. Avoid thick creams or oils that may clog pores. Ingredients like coconut oil can be comedogenic and worsen congestion.
Cleansing
Wash your face twice daily with a gentle, non-abrasive cleanser. This helps remove excess oil, impurities, and dead skin cells without over-drying the skin, aiding in unclogging pores.
Moisturising
Moisturising is essential, even for oily skin. Use a light, non-comedogenic moisturiser to maintain hydration and balance oil levels without clogging pores.
Suncare
Protecting your skin from UV rays supports a healthy skin barrier and can prevent further irritation or discoloration.
Product Choices and Ingredients
When choosing products, look for those labelled "oil-free" and "non-comedogenic." Ingredients like salicylic acid and retinol are particularly beneficial for their exfoliating and cell-turnover-promoting properties.
The Vinopure Routine
The Vinopure line offers a comprehensive approach to targeting comedonal acne:
- Cleansing with the Vinopure Purifying Gel Cleanser: This cleanser effectively removes excess oil, impurities, and dead skin cells without over-drying the skin. It helps unclog pores and prepare the skin for applying follow-up skincare products.
- Toning with the Vinopure Purifying Toning Lotion: The toning lotion refines pores and further preps the skin for treatment, helping to balance oil production and soothe the skin.
- Treating with the Vinopure Blemish Control Salicylic Acid Serum: This serum contains natural salicylic acid to target comedones and prevent new formations. It penetrates pores to dissolve excess sebum and exfoliate dead skin cells.
- Moisturising with the Vinopure Moisturizing Mattifying Fluid: The oil-control moisturiser hydrates the skin without clogging pores, helping to maintain a balanced and clear complexion.
- Purifying with the Green Clay Mask: This mask allows for the reduction of blemishes, enlarged pores, blackheads, and oiliness, leaving the skin mattified and clear. Made with green clay and zinc, it purifies pores in just 5 minutes and is ideal for acne-prone skin.
Caudalie Vinopure Pore Purifying Gel Cleanser
Preventing Closed Comedones
Preventing comedonal acne involves consistent skincare habits and avoiding pore-clogging ingredients. Gentle cleansing and hydration help the skin clear naturally. Stay consistent with your routine.
Practical Daily Habits
- Avoid popping closed comedones, as it can cause irritation or scarring and may damage your skin barrier.
- Refrain from using skin or hair care products, including cosmetics, that contain oil.
- Avoid thick creams or oils that may clog pores.
- Avoid regularly touching your face or wearing tight headgear, as heat, humidity, and sweat can worsen congestion.
Consistently following a skin care routine that involves washing the face and using gentle, oil-free products can also help prevent future comedone breakouts.