Does your child get small, itchy bumps on their elbows or knees every summer? These stubborn rashes could be a sign of frictional lichenoid dermatitis, a seasonal skin disorder that often affects active children. This papular eruption of childhood often appears in the warmer months, especially after engaging in outdoor activities.
The rash is usually mild, but it may itch or worsen with chronic scratching. The name might sound complex, but the causes are pretty straightforward. These skin bumps happen when friction (like from rough clothes or surfaces) combines with sweat, heat, and sun exposure - things that are more common in summer.
It's important to get the diagnostic criteria right, especially since this morphologic variant can mimic other conditions.
Understanding Dermatitis
Dermatitis is a common condition that causes swelling and irritation of the skin. It has many causes and forms and often involves itchy, dry skin or a rash. Or it might cause the skin to blister, ooze, crust, or flake. Three common types of this condition are atopic dermatitis, contact dermatitis, and seborrheic dermatitis. Dermatitis isn't contagious, but it can be very uncomfortable. Moisturizing regularly helps control the symptoms. Each type of dermatitis tends to occur on a different part of the body.
Our skin is like a brick wall. Where your waistband would sit, where your socks or shoes would rub. If you have a watch, where you would wear your watch. It's important to bathe regularly. It's important to hydrate the skin with a moisturizer that is hypoallergenic.
There are certain plants and fruits in nature, such as dill, buttercup, bergamot, musk ambrette, parsley, parsnip, and citrus fruits, especially lime, that when these chemicals they contain hit your skin and then it's exposed to ultraviolet light, a chemical reaction occurs. Typical scenarios would be when you brush up against certain plants on a hike or when you squeeze a lime into a drink, maybe you get some juice on your hands, you touch your arm. A lot of people think that it's poison ivy with the lines and the streaks, but it's, indeed, not.
A common cause of dermatitis is contact with something that irritates your skin or triggers an allergic reaction. Examples of such things are poison ivy, perfume, lotion, and jewelry containing nickel. Age can also be a factor; dermatitis can occur at any age, but atopic dermatitis is more common in children than adults. Allergies, atopic dermatitis, and asthma can also contribute. Occupation plays a role as well; jobs that put you in contact with certain metals, solvents, or cleaning supplies increase your risk of contact dermatitis. Other health conditions can also be a contributing factor.
Complications of Dermatitis
Repeated scratching that breaks the skin can cause open sores and cracks. These increase the risk of infection from bacteria and fungi. In people with brown and Black skin, dermatitis might cause the affected skin to darken or lighten. These conditions are called post-inflammatory hyperpigmentation and post-inflammatory hypopigmentation.
Basic Skin Care Routine for Prevention
Developing a basic skin care routine may help prevent dermatitis. Take shorter baths and showers; limit your bath or shower to about 10 minutes. Use lukewarm, not hot, water. Use a mild soap or a soapless cleanser. Choose a cleanser that has no dyes, alcohols, and fragrance, as some soaps can dry the skin. For young children, you usually need only warm water to get them clean-no soap or bubble bath needed.
Pat dry. After bathing, gently pat the skin with a soft towel. Moisturize all the skin. While the skin is still damp, seal in moisture with an oil, cream, or lotion. Many moisturizers are sold; try different products to find one that works for you. The ideal moisturizer is safe, unscented, effective, affordable, and one that you like to use regularly.
Frictional Lichenoid Dermatitis: Specifics
Frictional lichenoid dermatitis is a benign, seasonal, and self-limiting condition. Knowing about it helps avoid unnecessary concern or overtreatment. Frictional lichenoid eruption is a rare, self-limiting skin disease diagnosed with a rash in young children. Previously, it was believed to have a correlation with atopic dermatitis (a condition where the skin becomes dry, itchy, and inflamed).
The rash is typically described as skin-colored or reddish-raised papules on the outer surface of the joints and elbows. The etiology is unknown. The condition is self-limiting. Boys are more commonly affected than girls in the ratio of 3:1. The most common sites of involvement are the elbows, knees, and dorsal hands. Skin rashes tend to resolve spontaneously. The number of lesions may vary from few to many, as they can coalesce to form plaques.
Causes and Triggers
Dry elbows may be due to changes in climate, lack of hydration, or irritation from fabrics or lotions. Dry elbows may be uncomfortable and may cause skin discoloration in some cases. Sometimes, dry elbows may be a sign of an underlying condition, such as psoriasis, eczema, diabetes, or thyroid issues.
Dry skin on the elbows occurs from a lack of moisture in the skin. There may not be enough moisture, or a lack of oil to keep the moisture in, resulting in dry skin. Hot baths and showers can strip the skin of oils and cause dryness. Occupations that involve frequent contact with water, such as hairdressing, cleaning, or cooking, can also have a similar effect. Cool, dry, or hot weather can play a part in dry skin. Low humidity, wind, and cold or heat can exacerbate dryness. Dry air from fans or air conditioning could also worsen dry skin.
Dehydration: A lack of hydration in the body can cause dry skin. Sweating may also contribute to dehydration, especially if the person does not replace lost fluids. Smoking: The chemicals in cigarettes speed up skin aging, which can result in dry, coarse skin. Friction: Friction from tight clothes may irritate and dry the elbows. A person who rests on hard surfaces can also make elbows dryer and rougher, due to the friction that rubs or irritates the skin. Age: As people age, they tend to produce less sweat and oil, which results in dryer skin around the body. Certain medications: Some drugs, such as diuretics or statins, may dry out the skin.
Underlying Health Conditions
Several health conditions can cause dry skin on the elbows:
- Eczema: A skin condition that causes dry, itchy skin. It can occur anywhere on the body, including the elbow. Other symptoms include inflamed patches of skin, skin that feels scaly, tough, or thickened, cracking, and oozing. If the skin is cracked, oozing pus, or warm to the touch, a person may have an infection and should speak with a doctor as a priority.
- Psoriasis: A skin condition that can affect any part of the body, but it usually appears on the elbows, knees, or scalp. Symptoms include raised patches or plaques on the skin, itchiness, a burning or stinging sensation, lesions or pustules, and flaking skin.
- Nutritional deficiencies: Deficiencies in iron, zinc, vitamin D, vitamin A, or vitamin B3 (niacin) can lead to dry skin. Other potential signs of deficiencies can include tiredness, mood changes, or difficulty concentrating.
- Thyroid problems: Thyroid conditions can disrupt the skin’s function, leading to dry skin on the elbows and other areas of the body. People may have scaly skin that cracks or feels tough and waxy. Other symptoms of thyroid conditions can include thinning hair, an itchy scalp and dandruff, brittle or crumbly nails, slow-healing wounds, and swelling in the neck (a goiter) or protruding eyes.
- Diabetes: People with diabetes are more likely to have dry skin. High blood sugar levels can cause dry, itchy skin. Other signs of diabetes that appear on the skin include patches that feel velvety and are darker than the surrounding skin, thick, waxy patches on the fingers, toes, and other areas of the body, slow-healing wounds (particularly on the feet), and infections.
- Sjögren disease: Other symptoms of Sjögren disease include dry eyes, nose, and mouth, fatigue, difficulty with memory or concentration, numbness or tingling in fingers and toes, and digestive symptoms.
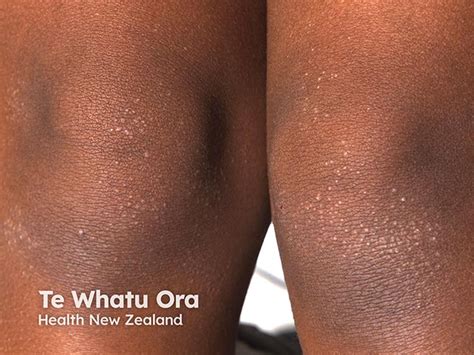
Symptoms of Dry Elbows
Dry elbows may feel dry, rough, or tight. The skin may also look dry, scaly, or irritated. The skin may flake, peel, itch, feel sore or uncomfortable, crack, or bleed.
Management and Treatment
For people with mild dryness on the elbows, self-care may help to ease the symptoms. It may help to:
- Minimize contact with water, particularly hot water, where possible.
- Wash the body using warm but not hot water and a gentle soap.
- Moisturize the area regularly, especially after contact with water.
- Wear soft fabrics consisting of natural fibers, such as cotton.
- Wash clothes with nonbiological detergents suitable for sensitive skin.
- Use a humidifier if dry indoor air is making dry skin worse.
- Protect the skin from the sun, wind, or cold.
Avoid rubbing the area or using harsh soaps or scrubs. People cannot scrub dry skin away, and this may make the skin sore and more irritated.
If an underlying condition is responsible for dry elbows, a person can see their doctor, who can diagnose the issue and suggest a treatment. If a person thinks medication might be responsible for their dry elbows, they can speak to a doctor. A healthcare professional may alter the treatment to reduce side effects or suggest ways to avoid temporary dryness.
Contact a doctor if dry skin does not respond to treatment, or if symptoms get worse. Symptoms that can indicate a need for medical attention include open cracks and bleeding, sore or swollen skin, and signs of an infection, such as pus or fever. If people have any additional symptoms alongside dry elbows, they can see a doctor who can check for underlying health conditions.
Healthcare professionals may refer to dry skin as xerosis. To find the cause of dry elbows, they may take a full medical history and carry out a physical examination. Blood tests can also help the diagnosis process.
Products to Aid Management
This Satya Organic Eczema Relief Glide Stick makes it easy with a mess-free, travel-friendly format kids can use themselves. Remedywear Long Pants for Kids are lightweight, protective pants designed to be worn under regular clothing or as a dry wrap layer. Remedywear Long Sleeve Shirt for Kids is a soft, breathable top that comforts sensitive skin while shielding common flare-up areas like arms, chest, and back.
Dermatologist’s Top 5 Tips for Dry Skin | How to Fix Dry, Flaky Skin Fast
When to Seek Medical Advice
Contact a doctor if dry skin does not respond to treatment, or if symptoms get worse. Symptoms that can indicate a need for medical attention include open cracks and bleeding, sore or swollen skin, and signs of an infection, such as pus or fever. If people have any additional symptoms alongside dry elbows, they can see a doctor who can check for underlying health conditions.
For those with an underlying condition, treating the root cause may result in an improvement in dryness, but this can depend on the cause and available treatments.
Differentiating Frictional Lichenoid Dermatitis from Other Conditions
It's important to differentiate frictional lichenoid dermatitis from other skin conditions that may present with similar symptoms:
- Atopic Dermatitis: Papular eczema (patches of skin becoming rough and inflamed) may appear similar to frictional lichenoid eruption.
- Psoriasis: The plaques of psoriasis are usually erythematous. The papules usually coalesce to form large plaques. The psoriatic lesions are more commonly found on the scalp, elbows, knees, umbilicus, and genital organs. In the case of psoriasis, there is widespread skin involvement. A prominent silver scaling is seen in the psoriatic lesions.
- Keratosis Pilaris: The rough keratotic papules are typically present on the extensor surfaces of the upper and lower extremities. They are also commonly seen on the cheeks.
- Dermatomyositis: The skin findings in this disease include reddish or violet papules over metacarpophalangeal joints, proximal interphalangeal joints, and distal interphalangeal joints. These papules or plaques can also be present on elbows and knees.
- Flat Warts: Usually, the lesions are smooth or hyperkeratotic. The number of papules usually ranges from a few to hundreds.
- Molluscum Contagiosum: Usually, small lumps develop on the skin that are pearly-white or slightly pink. A tiny dimple is usually developed in the center of each molluscum.
The diagnosis is usually determined based on the characteristic clinical presentation of the skin disorder along with the age of the child, the time of the year when it occurs, the type of treatment modality, and relapses over the period of time. The typical rash appears as flesh-colored, mildly pigmented papules on the extensor surface of the knees, elbows, and sometimes the dorsal surface of hands. No laboratory or imaging techniques are required. A biopsy is usually not performed.
Usually, the disease rash is self-limiting, but if parents or the child are concerned about the symptoms, mild topical corticosteroids can be prescribed to control these symptoms. Vaseline petroleum jelly is also advised in some cases. It is a clinical skin disorder that is exacerbated by friction. Hence, the patient is advised to wear loose cotton clothes to avoid friction. Since this disease is aggravated by ultraviolet rays, it is advisable for the patient to sun protect themselves from the harmful ultraviolet rays. The most commonly prescribed medicine for inflammatory reactions is antihistamines. Antibiotics are most frequently prescribed in case of a superimposing infection. A healthcare professional can also recommend certain steroid gels for topical application.
Frictional lichenoid eruption is a benign, self-limiting, and usually recurrent disease. It usually resolves within weeks or months. The diagnosis is usually determined on the basis of clinical presentation.
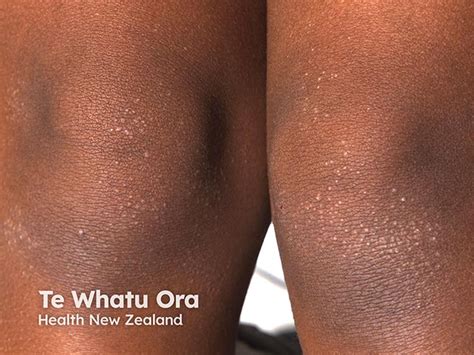
Frictional lichenoid dermatitis is a benign skin eruption that usually affects school-aged children. It typically appears in the summer months, presenting as small, flat, skin-colored or whitish bumps that may itch. These lesions often appear in areas of repetitive rubbing or friction, such as the elbows, knees, and backs of the hands. This condition has been known by many different names, reflecting the uncertainty around its exact cause: “juvenile papular dermatitis,” “frictional lichenoid eruption,” or even “slide dermatitis” (due to its association with play on friction-inducing surfaces).
The diagnosis is clinical, meaning it’s based on what we see during a skin exam and the patient’s context. Affected children are usually otherwise healthy, with no other skin diseases, and the lesions appear exclusively during the summer. The lesions have a typical distribution: small, flat, skin-colored tiny bumps, sometimes accompanied by mild redness or signs of scratching. Parents often consult because of the rash, especially if it itches, though it’s usually not very bothersome. A biopsy or other tests are rarely needed unless the diagnosis is unclear. In such cases, it’s important to rule out other conditions that might look similar, such as keratosis pilaris, lichen nitidus, or polymorphic light eruption.
Frictional lichenoid dermatitis is not dangerous. This is a mild, temporary skin condition with no serious consequences. It doesn’t affect internal organs, doesn’t leave scars, and has no long-term effects. It often resolves on its own by the end of the summer, even without treatment. There is no clear association with atopic dermatitis, although some overlap may occur in certain cases.
In many cases, no active treatment is needed, as it tends to disappear spontaneously. However, if the lesions are itchy or bothersome, the following measures can help: moisturizing creams or emollients to soothe and protect the skin, and mild topical corticosteroids for a few days, if there’s significant itching or inflammation. The most important thing is not to worry because this is not a serious or contagious condition. No special preventive measures are needed, although reducing friction (e.g., wearing looser clothing or avoiding rough play surfaces) may help.
In summary, frictional dermatitis is a benign, seasonal, and self-limiting condition. Knowing about it helps avoid unnecessary concern or overtreatment.
A 5-year-old boy presented to urgent care with a pruritic rash present on his elbows and knees. The rash had been present for approximately 1 month and had no known etiology. The severity of pruritus had been keeping him awake at night. The parents had been treating the rash and associated pruritus with over-the-counter topical hydrocortisone but noted that it had had minimal effect. No one in the household other than the patient had a rash or pruritus. The patient’s family history was notable for a grandmother with eczema. On physical examination, the child was interactive and appeared healthy. He was normocephalic with moist, clear mucous membranes. His lungs were clear to auscultation without increased respiratory effort. His cardiovascular examination showed normal rate and regular rhythm without heart murmurs. Skin examination revealed flat-topped papules that were flesh-colored to slightly erythematous on the extensor surfaces of the elbows and knees.
No laboratory or imaging studies were performed. The patient’s parents were counseled that FLD is a benign and self-limiting condition. FLD is a rarely diagnosed rash that occurs most commonly in children. It has been known by other names such as Sutton’s summer prurigo and dermatitis papulosa juvenilis, and previously it had been believed to be a variant of or have correlation with atopic dermatitis. The rash typically is described as flesh-colored or mildly erythematous flat-topped papules on the extensor surface of the elbows and knees, with unknown etiology to the patient and parents. A 2009 report described cases of FLD in 3 adult patients. While this disease has been seen most often in children since its first description in 1956, this 2009 case series would be the first reported diagnoses of FLD in adults. These 3 case diagnoses were verified through histologic comparison of biopsies.
tags: #frictional #lichenoid #dermatitis #elbow