Understanding the difference between a tick bite and a pimple is crucial for recognizing potential health risks. While both can appear as small bumps on the skin, tick bites can lead to serious infections like Lyme disease, necessitating prompt identification and treatment. This guide provides detailed information on the symptoms, risk factors, and prevention of tick bites, helping you distinguish them from common skin irritations.
Understanding Tick Bites
Ticks are tiny, biting arachnids that feed on the blood of warm-blooded animals, including humans. They burrow painlessly into the skin with their feeding parts, bite, draw blood, and eventually drop off when they become engorged with blood. Only the feeding parts are inserted into the skin. The body, which is dark in color and ranges from the size of a poppy seed to a pencil eraser, remains visible on the skin surface or scalp. Ticks swell and turn bluish-gray when filled with blood.
The secretions from a tick's feeding parts can cause skin reactions such as raised areas, lumps, and growths called granulomas. In rare cases, fever and paralysis may develop after bites from many types of ticks; paralysis is due to a toxin transmitted from the tick's secretions, not an infection.
Where Ticks Live and How They Transmit Disease
Ticks inhabit tall grass and wooded areas, particularly cool, moist, mature woods with thick undergrowth. They can also be found at the edges of woods near lawns or fields, but rarely in lawns, which are too dry and hot. Ticks wait in the underbrush for an animal or human to brush by, and then grasp the fur or skin and crawl up the leg. They do not fly, jump, or drop from trees.
Lyme disease is an illness caused by Borrelia bacteria. Ticks that can carry Borrelia bacteria live throughout most of the United States, but Lyme disease is most common in the upper Midwest and the northeastern and mid-Atlantic states. In Europe, a different species of Borrelia causes Lyme disease. Ticks pick up bacteria from a host, such as a deer or rodent. They don't get sick, but they can pass the bacteria to another host. When an infected tick feeds on a person, the bacteria can move to the person's bloodstream. Both young and adult ticks can carry the disease; young ticks are tiny and hard to spot.

Symptoms of Tick Bites and Tick-Borne Diseases
Most tick bites do not cause any symptoms. Tick paralysis is relatively rare and begins in the feet and legs, gradually working its way to the upper body, arms, and head over a period of hours or days. Once the tick is removed, a person with tick paralysis will recover completely.
Symptoms associated with tick-borne infections differ depending on the type of infection. Generally, the tick bite itself does not cause immediate symptoms, although some people may develop fever, headache, nausea, and a general sick feeling caused by tick secretions. Tick saliva contains immunosuppressants and numbing agents that help the tick feed undetected.
Early Symptoms of Lyme Disease
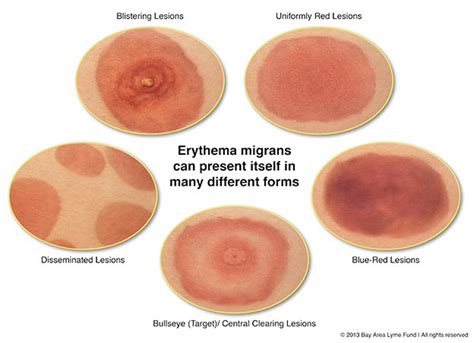
Early symptoms of Lyme disease usually happen within 3 to 30 days after a tick bite. This stage of disease has a limited set of symptoms. A rash is a common sign of Lyme disease, but it doesn't always happen. The rash is usually a single circle that slowly spreads from the site of the tick bite. It may become clear in the center and look like a target or bull's-eye.
Stage 2 Lyme Disease
Without treatment, Lyme disease can worsen. The symptoms often show up within 3 to 10 weeks after a tick bite. Stage 2 is often more serious and widespread.
Stage 3 Lyme Disease
In the third stage, you may have symptoms from the earlier stages and other symptoms. In the United States, the most common condition of this stage is arthritis in large joints, particularly the knees. Pain, swelling, or stiffness may last for a long time, or the symptoms may come and go. The type of Lyme disease common in Europe can cause a skin condition called acrodermatitis chronica atrophicans, where the skin on the backs of the hands and tops of the feet becomes discolored and swells. It may also show up over the elbows and knees.
Other Tick-Borne Infections
A tick bite can cause many different tick-borne infections, with highly variable durations. Some include:
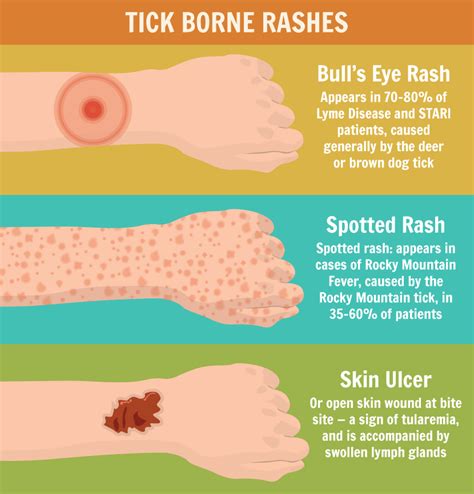
- Human monocytic ehrlichiosis: Symptoms ranging from mild to severe can involve many organ systems, including high fever, headache, fatigue, nausea, weight loss, and a spotted rash.
- Anaplasmosis: Symptoms range from mild to severe and include high fever, headache, a general sick feeling (malaise), achy muscles (myalgia), nausea, vomiting, cough, stiff neck, and confusion.
- Babesiosis: Many people will not have any symptoms. Others develop fatigue, fever, drenching sweats, nausea, vomiting, headache, muscle aches, joint aches, and jaundice.
- Tularemia: Symptoms vary widely, from asymptomatic to severe septic shock and death. Common symptoms include fever, chills, headache, and malaise. Many also develop a single, red ulcerated lump with a central scab and tender, swollen lymph nodes.
- Rocky Mountain spotted fever: Symptoms include fever, headache, a spotted rash on wrists and ankles, and a patchy rash on arms and legs.
- Alpha-gal syndrome: This is a unique food allergy that develops one to three months following a tick bite. The tick bite introduces a sugar molecule, "alpha-gal," to which the person develops an allergy. Eating foods containing alpha-gal (such as beef, lamb, and pork) can trigger abdominal pain, diarrhea, hives, and even anaphylaxis two to eight hours after consumption.
Tick Bites vs. Pimple Symptoms
A tick bite can often resemble a small pimple, especially in its early stages. It may appear as a small, red bump, much like a mosquito bite, for one to two days following the bite. Unless it is infected, there will be no fluid or pus. The key difference often lies in the presence of the tick's mouthparts or the characteristic bull's-eye rash associated with Lyme disease.
When ticks attach onto the skin, it's not uncommon for a part of their mouth to remain embedded. This can appear as a dark spot or a small, hard bump. While a pimple is typically caused by clogged pores and bacterial infection, a tick bite is an actual puncture wound made by an arachnid. Significant redness, swelling, especially when accompanied by severe pain, can indicate infection or other problems related to a tick bite.
Risk Factors for Tick Bites
Your risk for getting Lyme disease depends on if you spend time where ticks are likely to live. This includes regions where deer ticks that carry Lyme disease are widespread, such as the upper Midwest, northeastern and mid-Atlantic states, and in south central and southeastern Canada.
Habitat: Ticks are found in grassy, brushy, or wooded areas. They are especially found in wooded areas where deer and rabbits live, which are also popular spots for outdoor activities like camping, hiking, hunting, and fishing. Increasingly, people encounter ticks in their own backyards.
Time of Year: The risk of infection is greater in the spring, summer, and fall.
Activities: Spending time outdoors in tick-infested areas, such as walking or working in grassy, wooded areas or overgrown fields, increases risk. Ticks often attach to the lower legs and feet.
Preventing Tick Bites
The best way to prevent Lyme disease is to avoid tick bites when you are outdoors. Here are key prevention strategies:
- Use Repellents: Spray your outdoor clothing, shoes, tents, and other camping gear with a repellent that has 0.5% permethrin. Use an insect repellent registered with the Environmental Protection Agency on any exposed skin, except your face.
- Wear Protective Clothing: When in tick-prone areas, wear long sleeves and pants, tucking your pants into your socks.
- Stay on Trails: When in the woods, walk on cleared trails and avoid walking through tall grass or dense underbrush.
- Check Yourself and Others: Thoroughly check yourself, children, and pets for ticks after spending time in tick-infested areas. Pay attention to your underarms, hair and hairline, and scalp. Use a mirror to check your body well.
- Shower Promptly: Shower as soon as possible after coming indoors to wash off any loose ticks.
- Check Gear: Inspect your camping gear and clothing for ticks.

Removing Ticks and Seeking Medical Attention
When a tick is discovered on the skin or scalp, it should be removed immediately to avoid a skin reaction and to reduce the likelihood of developing a tick-borne infectious disease. The organisms that cause Lyme disease and babesiosis are rarely transmitted if ticks are removed within the first 24 hours after they attach and before they become engorged.
Proper Tick Removal
- Grasp the head of the tick with a pair of fine-tipped or curved forceps or tweezers held as close to the skin as possible.
- Avoid squeezing the tick's body.
- Gently pull the head of the tick away from the skin with a slow, steady upward motion, without twisting.
- Clean the bite area thoroughly with soap and water.
If a tick has buried itself deep in the skin and you cannot remove it, or if you find an engorged tick on your skin and are living in or visiting an area where Lyme disease is a risk, seek medical attention.
When to See a Doctor
Most people who get Lyme disease don't remember having a tick bite, and many symptoms of Lyme disease relate to other conditions. See your health care provider if you have Lyme disease symptoms. If you know you had a tick bite or might have been around ticks, watch for symptoms.
Seek medical attention if:
- You develop fever and flu-like symptoms after a known tick bite.
- The bite is accompanied by a skin rash, particularly the bull's-eye rash characteristic of Lyme disease.
- A tick has buried itself deep in the skin and you cannot remove it.
- You find an engorged tick and are in a high-risk Lyme disease area.
For people in areas where Lyme disease rates are high, one dose of doxycycline can prevent disease if taken within three days of a tick bite. For those at highest risk, early treatment may be appropriate. Other treatments vary depending on the specific disease caused by the tick bite.