Melanoma is a type of tumor that originates from melanocytes, the cells responsible for producing pigment in the body. While often recognized by its dark, pigmented appearance, melanoma can also be amelanotic, meaning it lacks pigment and presents as pink or flesh-colored masses. In dogs, melanoma is a significant concern, particularly when it affects the oral cavity, digits (toes), or eyes. Oral melanoma is the most common type of cancer in a dog's mouth and can be aggressive, frequently metastasizing to other parts of the body, primarily the lymph nodes and lungs.
Understanding Canine Oral Melanoma
Oral melanoma (OM) is a highly aggressive tumor that can spread rapidly. Dogs may not show obvious signs of the disease at home, often leading to its discovery during routine veterinary examinations or when an owner notices a tumor in the mouth. Owners might observe symptoms such as increased salivation or drooling, difficulty eating or drinking, dropping food, or chewing on only one side of the mouth. Facial swelling and a foul odor to the breath can also be indicators. If the tumor spreads to the lymph nodes, swelling may be noticeable under the jaw or along the neck.
While OM is often suspected when a tumor is pigmented, a significant percentage, up to 38%, are amelanotic and thus lack color. This can sometimes lead to delayed diagnosis, as they may not be as readily apparent as pigmented masses.
The World Health Organization has established a staging system for oral melanoma in dogs, which is crucial for prognosis and treatment decisions. The primary size of the tumor at diagnosis is a key factor in long-term survival. Tumors smaller than 2 cm that have not spread to other areas generally have the best prognosis, while those larger than 4 cm with evidence of spread have the worst.
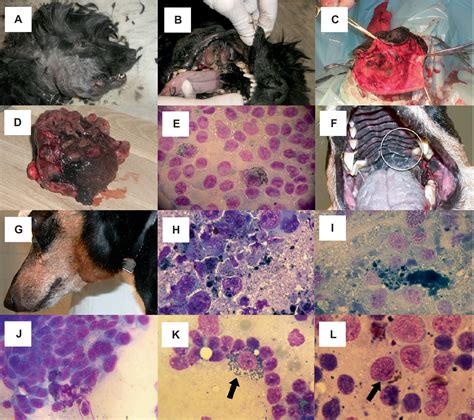
Diagnosis of Amelanotic Melanoma
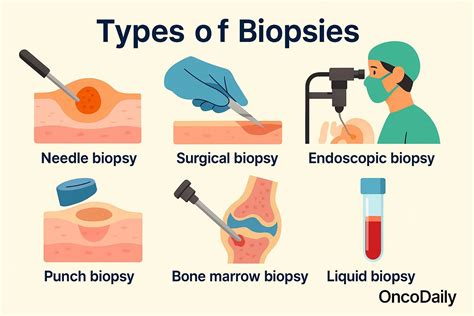
Confirming a diagnosis of canine melanoma, especially amelanotic types, requires specific diagnostic procedures. A complete physical examination is essential to identify both external and internal signs of the disease. The diagnosis is typically confirmed through a biopsy or aspirate of the abnormal tissue.
To assess the overall health of the patient and their suitability for treatment, a complete blood count (CBC), serum chemistry panel, and urinalysis are performed. These tests help determine if the cancer has affected bodily functions and identify any underlying health issues.
Further staging involves evaluating the spread of the cancer. Lymph nodes near the tumor or those that appear abnormal are sampled via aspirate or biopsy. Imaging techniques such as chest X-rays and abdominal ultrasound are used to check for metastasis in the lungs and internal organs. In some cases, advanced imaging like a CT scan or MRI may be necessary to obtain a more detailed view of the tumor's extent and invasion into surrounding tissues, including bone.
For amelanotic melanomas, which can histologically resemble other oral tumors like sarcomas or epithelial tumors, immunohistochemistry (IHC) is often required for accurate differentiation. This may involve additional testing on the biopsy sample, which your veterinarian will discuss with you.
Treatment Options for Canine Melanoma
The treatment approach for canine melanoma is multi-faceted and depends on the stage and location of the tumor. The primary goal is to remove the tumor and prevent its spread.
Surgical Resection
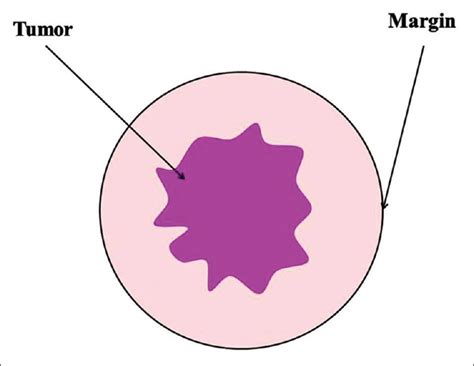
Wide surgical resection is the recommended treatment for oral melanoma tumors. Due to the tendency of these tumors to invade underlying bone, complete removal often necessitates excising portions of the jawbone (mandibulectomy or maxillectomy). While this may sound extensive, dogs can typically resume normal eating, drinking, and playing activities after recovery. Surgical margins of 1-2 cm of normal tissue around the tumor are aimed for to ensure complete removal. Debulking surgery, which removes as much of the tumor as possible without achieving clean margins, is generally not recommended due to the high likelihood of rapid recurrence.
Regional lymph nodes are usually removed during surgery to assess for metastasis. For tumors located on the gums and palate, complete removal may involve removing the underlying bone.
Radiation Therapy
Radiation therapy can be used in several scenarios. It may be employed to shrink large tumors before surgery or administered after surgery if the tumor was not entirely removed (incomplete margins). Radiation can also be a primary treatment for locoregional disease, especially in cases where complete surgical resection is not feasible. Survival times following radiation therapy can vary, with some studies showing remission rates up to 70% in certain cases. However, the effectiveness can be influenced by various factors, including the number of negative prognostic indicators present.
Chemotherapy
Chemotherapy is recommended for most cases of oral melanoma, even though data directly supporting improved patient outcomes is limited. It is considered the treatment of choice for dogs with widespread disease. Carboplatin is a commonly used injectable drug administered every three weeks. While generally well-tolerated, potential side effects include gastrointestinal upset and a temporary decrease in white blood cell counts. Severe reactions are uncommon.
Chemotherapy may be recommended as an adjuvant treatment after surgery or radiation, particularly if there is concern about microscopic disease remaining or if the tumor is unresectable. It can also be a primary treatment for dogs with advanced or metastatic disease.
Immunotherapy
Immunotherapy, specifically a commercially available vaccine (Oncept®), is another treatment option. This therapeutic DNA vaccine is designed to stimulate the dog's immune system to fight melanoma cells. It has shown promise as an adjunctive treatment, particularly for dogs with Stage II and III oral melanoma after surgical removal and potentially radiation therapy, potentially leading to longer median survival times. However, its efficacy as a standalone treatment for untreated tumors is not established. The vaccination protocol typically involves initial doses every two to four weeks, followed by booster vaccinations every six months. It's important to note that it can take several months for the body to mount an adequate immune response.
How Vaccines Work, Herd Immunity, Types of Vaccines, Animation
Prognosis and Supportive Care
The prognosis for dogs with melanoma varies significantly based on the stage of the disease, tumor location, and the extent of treatment received. Dogs with Stage I melanoma generally have much longer survival times than those in later stages. For instance, with aggressive surgery alone, 1-year survival rates can be less than 35%, with survival times ranging from approximately 150 to 874 days. Early detection and prompt treatment are critical factors in improving outcomes.
Supportive medications for potential side effects like nausea (indicated by decreased appetite, increased salivation, or drooling) and diarrhea may be prescribed. It is advisable to administer these medications proactively as soon as any signs are noted.
While melanoma is an aggressive cancer, and many dogs sadly succumb to distant metastasis despite treatment, the combination of surgery, radiation, and immunotherapy offers the best chance for managing the disease and improving quality of life. The selection of therapy is not binding and can be adjusted based on the individual needs of the dog and owner.
tags: #canine #amelanotic #melanoma