The human skin is equipped with several types of exocrine organs, known scientifically as glandulae cutis, which discharge biochemical substances onto the skin's surface. These skin organs are fundamentally composed of a secretory compartment, referred to as the gland or tubule, and an excretory part, the duct. The secretory cells of these skin organs are of epithelial origin, with their secretory compartments situated at varying depths within the dermis.
Three primary types of skin glands are recognized based on their product, excretory function, and the location where their excretory ducts discharge their contents. These glands are categorized into those releasing sebum, known as sebaceous glands, and sweat glands. Regarding their secretory capacity, skin glands are further classified into holocrine glands, where entirely differentiated secretory cells rupture and release both cytoplasmic substance and cell membranes into their ducts, and merocrine glands, which discharge their product through exocytosis from secretory cells without cellular damage.
In terms of duct discharge location, the ducts of sebaceous glands and apocrine sweat glands typically open into the hair follicle canal. In contrast, eccrine sweat glands discharge their product directly onto the skin surface. Structurally, sebaceous glands are holocrine glands, while both eccrine and apocrine sweat glands are merocrine glands.
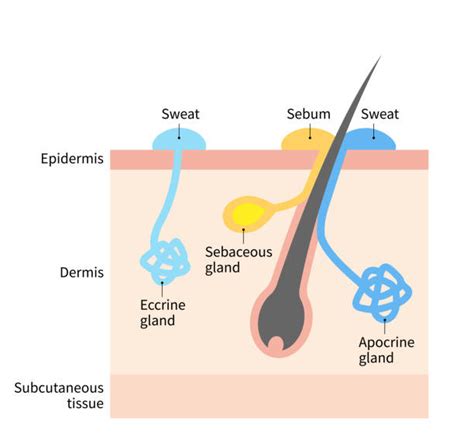
Understanding Sweat Glands: Eccrine and Apocrine
Sweat glands, also referred to as sudoriferous glands, are simple tubular structures found ubiquitously throughout the body. Sweat is produced in the coiled secretory portion of these glands, typically located within the dermis, though in some instances, it may extend into the hypodermis.
Humans possess two principal types of sweat glands: eccrine and apocrine glands. Eccrine glands are distributed across the majority of the body and play a crucial role in thermoregulation by producing a watery, odorless sweat. Conversely, apocrine glands are concentrated in specific regions of the body, such as the armpits and groin. These glands secrete a thicker, milky fluid that, upon breakdown by skin bacteria, can result in body odor.
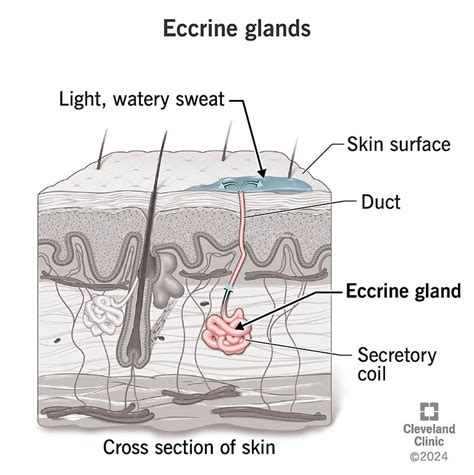
Eccrine Glands: The Thermoregulation Specialists
The most numerous types of sweat glands in human skin are the eccrine sweat glands, found almost everywhere on the body. These are considered the primary sweat glands for regulating body temperature. When the body's internal temperature rises, eccrine glands release a clear, odorless substance, primarily composed of water and NaCl, onto the skin surface. The cooling effect is achieved through the evaporation of this sweat.
Eccrine glands consist of a tube-shaped duct that terminates in a coiled, secretory unit. This unit is composed of cuboidal cells surrounding a central lumen. Surrounding these cuboidal cells are myoepithelial cells, which contract in response to stimuli to aid in secretion.
The initial secretion from eccrine glands is composed of water, sodium, and potassium ions. However, the epithelial lining of the ducts reabsorbs a significant portion of these ions, resulting in sweat with a higher water content. Humans have an estimated two to five million eccrine sweat glands, with an average distribution ranging from 150 to 340 per square centimeter. They are most concentrated on the palms and soles, followed by the head, trunk, and extremities. While some individuals have more glands than others, there is no significant difference in number between males and females.
The specific function of eccrine glands on the palms and soles differs from those on hairy surfaces; they are tasked with keeping these areas moist to prevent flaking or hardening of the horny layer, thereby maintaining tactile sensibility. A dry hand has reduced grip and sensitivity. Therefore, eccrine glands can be categorized into those responding to thermal stimulation for thermoregulation and those responding to psychological stimuli to maintain friction surfaces.
Eccrine glands develop early in fetal development, forming on the palmoplantar skin around the fourth month of gestation and subsequently spreading to the rest of the body about a month later. They are fully formed by the time of birth.
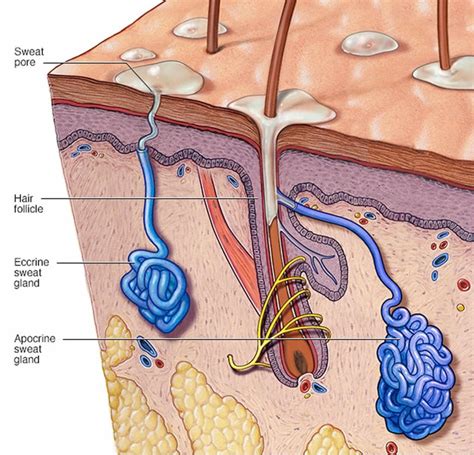
Apocrine Glands: Associated with Body Odor and Hormonal Influence
Apocrine glands, while structurally similar to eccrine glands, possess a larger secretory component lined by either cuboidal or columnar epithelium and associated myoepithelial cells. These glands produce a thicker, oily, and initially odorless secretion containing water, lipids, proteins, and steroids. Their excretions are subsequently broken down by skin bacteria into various chemicals responsible for body odor.
Apocrine glands are found in more restricted areas of the body, including the axilla (armpits), anogenital region, external ear canal, and areola. In some mammals, apocrine glands serve as the primary thermoregulators; however, their exact function in humans is still under investigation. Some hypotheses suggest they are responsible for body odor or pheromone production. While their initial secretion is milky and odorless, bacteria on the skin surface break down the fluid, releasing a distinctive odor.
Apocrine glands present at birth do not become active until puberty. Their exact function remains somewhat unclear, but they are known to become active during times of stress, pain, and sexual arousal, although the underlying reasons are not fully understood. Similarly, the purpose of body odor in humans is not completely known, but research suggests it may play a role in communication. The odor of individual humans primarily stems from apocrine secretion, with some contribution from sebum.
Apocrine glands are derived from the differentiation of a hair follicle. Hair follicles begin to develop in the embryo around 9 weeks of gestation and continue to develop caudally. These follicles are composed of cells that differentiate into the follicle, infundibulum, sebaceous, and apocrine units. Around 4 months of gestation, the apocrine gland arises from the infundibulum, the epithelial structure below the hair follicle, and is continuous with the skin epidermis.
Strictly speaking, apocrine glands are not directly involved in sweating in the same way as eccrine glands. They appear late in fetal development (5 to 5.5 months) nearly everywhere on the body. Most of these rudimentary structures disappear within weeks, except in specific areas like the external ear canals, axillae, nipples, around the navel, and on the anogenital surfaces. Single glands may be found elsewhere.
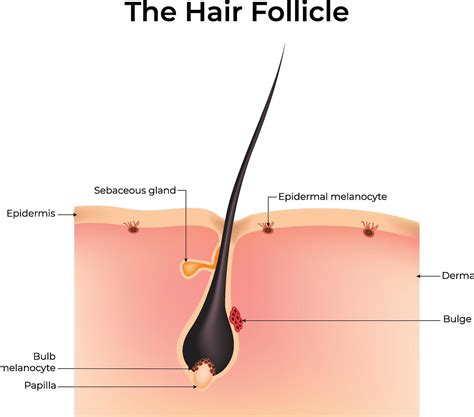
Sebaceous Glands: The Oil Producers
Sebaceous glands, also known as oil glands, are responsible for producing sebum within the dermis. These glands develop from the epithelial cells of the hair follicle itself, specifically from the external root sheath. Consequently, their ducts typically open into the upper part of a hair follicle, known as the infundibulum.
Sebaceous glands function through a holocrine secretion process. This means the entire gland cell fills with sebum and then ruptures to release its oily content. Sebaceous glands are active from birth, producing a waxy coating that protects newborn skin. They become particularly active during puberty under hormonal influence.
While sebaceous glands are present across most of the skin, they are notably absent on the palms of the hands and the soles of the feet. Sebum acts as a natural lubricant, helping to moisturize the skin by slowing down the evaporation of water from its surface. Sebum also plays a protective role by limiting the growth of certain bacteria, containing antimicrobial compounds that prevent bacteria from penetrating deeper skin layers.
Sebaceous glands are implicated in several common skin conditions. During puberty, hormonal changes stimulate these glands to produce more sebum, often leading to oily skin. If a sebaceous duct becomes clogged with sebum, it can form a whitehead. If this trapped material dries and oxidizes, it darkens into a blackhead. When a sebaceous gland becomes infected, it can lead to more severe forms of acne.
Following a daily skincare routine can help prevent pores and hair follicles from becoming clogged with excess sebum, managing the effects of hyperactive sebaceous glands.
Comparison of Sebaceous and Sweat Glands
| Feature | Sebaceous Glands | Sweat Glands (Eccrine & Apocrine) || :---------------- | :-------------------------------------------------- | :---------------------------------------------------- || **Primary Product** | Sebum (oil) | Sweat (water, electrolytes, some lipids/proteins) || **Secretion Method** | Holocrine (entire cell ruptures) | Merocrine (exocytosis) || **Duct Opening** | Usually into hair follicle | Eccrine: onto skin surface; Apocrine: into hair follicle || **Location** | Widespread, absent from palms/soles | Widespread (eccrine); Axilla, groin, etc. (apocrine) || **Function** | Lubrication, waterproofing, antibacterial | Thermoregulation (eccrine), odor/pheromones (apocrine) || **Activity** | Active from birth, increases at puberty | Eccrine: continuous; Apocrine: active from puberty || **Structure** | Alveolar sacs | Tubular (coiled secretory unit, duct) || **Associated with**| Hair follicles | Hair follicles (apocrine); independent (eccrine) |Embryological Development
Eccrine glands originate from the embryonic ectoderm. Apocrine glands, on the other hand, are derived from the differentiation of a hair follicle. The development timelines also differ: eccrine glands form on the palmoplantar skin around the fourth month of gestation, while apocrine glands arise from the infundibulum of the hair follicle at about 4 months of gestation.
Blood Supply, Lymphatics, and Innervation
Both eccrine and apocrine glands receive blood supply from vascular plexuses in the dermis, with capillaries enveloping the glandular structures. Lymphatics run parallel to the blood supply, with capillaries originating in the dermal papillae and draining into larger plexuses. The sympathetic nervous system innervates eccrine glands, with both cholinergic and adrenergic fibers mediating sweat secretion, primarily controlled by the central nervous system. Apocrine glands secrete in response to epinephrine and norepinephrine, though the exact mechanism of neural control is less understood.
Clinical Significance
Disruptions in sweat gland function can lead to various clinical conditions. Hyperhidrosis is characterized by excessive sweating beyond what is needed for thermoregulation. Conversely, hypohidrosis and anhidrosis involve diminished or absent sweat production, increasing the risk of heat stroke.
Hidradenitis suppurativa (HS) is a chronic inflammatory condition affecting hair follicles, often involving apocrine glands, leading to nodules, sinus tracts, and scarring, primarily in intertriginous areas. Treatment involves antibiotics, systemic medications, and surgical intervention.
Bromhidrosis refers to excessive body odor, which can be associated with either eccrine or apocrine glands. Apocrine bromhidrosis, occurring after puberty, is due to bacterial breakdown of sweat components. Eccrine bromhidrosis can be localized (e.g., feet) or generalized. Management focuses on reducing sweat and bacteria.
Chromhidrosis, or colored sweat, is caused by lipofuscin pigment in sweat glands, most commonly apocrine glands, resulting in colored sweat. Treatments include botulinum toxin injections and capsaicin cream.
Miliaria, or sweat rash, results from the blockage or inflammation of eccrine sweat glands, with various types depending on the level of obstruction. Management involves maintaining a cool environment and topical treatments.
Fox-Fordyce disease is a disorder caused by the blockage of apocrine sweat glands, leading to pruritic papules, typically in the axilla and groin. Treatment options include topical therapies, surgical excision, and phototherapy.
The sebaceous glands are also involved in common skin conditions like acne. Hormonal fluctuations, particularly during puberty, increase sebum production. Blockage of sebaceous ducts can lead to comedones (blackheads and whiteheads), and infection can result in more severe inflammatory acne.