Contact dermatitis is a skin inflammation and rash that arises from direct contact with a particular substance. This rash can be itchy, is typically confined to a specific area, and often presents with clearly defined borders. The underlying cause of contact dermatitis is either an irritant or an allergic reaction. The resulting rash may be itchy, painful, or both. Diagnosis is usually based on the appearance of the rash and a thorough history of potential exposures to various substances. Effective management involves avoiding or protecting oneself from the causative agents. Treatment strategies include removing the offending substance, implementing measures to alleviate itching, applying topical corticosteroids, and sometimes using dressings.
Understanding the Mechanisms of Contact Dermatitis
Substances can induce skin inflammation through two primary mechanisms:
- Irritation (Irritant Contact Dermatitis): This type accounts for the majority of contact dermatitis cases. It occurs when a toxic or chemical substance directly damages the skin upon contact. Irritant contact dermatitis tends to be more painful than itchy.
- Allergic Reaction (Allergic Contact Dermatitis): This type involves a delayed hypersensitivity reaction of the body's immune system to a substance that has contacted the skin.
Irritant Contact Dermatitis
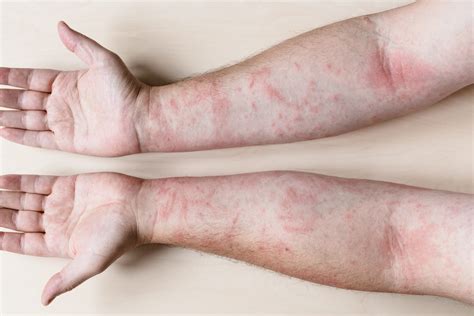
Irritant contact dermatitis occurs when a substance causes direct damage to the skin. This type of dermatitis can be more painful than itchy. Examples of irritating substances include acids, alkalis (like drain cleaners), solvents (such as acetone found in nail polish remover), strong soaps and detergents, certain plants (like poinsettias and peppers), and constant moisture from body fluids (such as urine and saliva).
Some of these substances can cause immediate skin changes within minutes, while others require prolonged exposure. Even mild soaps and detergents may irritate sensitive skin after frequent or prolonged contact. Individual skin sensitivity to irritants varies. Factors such as age (very young or very old individuals) and environmental conditions (low humidity or high temperatures) can influence the development of irritant contact dermatitis.
Occupational dermatitis can also develop from materials encountered at work. This can manifest immediately after exposure or after a long period of repeated contact. In some instances, irritant contact dermatitis can arise after touching certain substances and subsequently exposing the skin to sunlight. This specific form is known as phototoxic contact dermatitis. In such cases, the rash develops only on the skin exposed to sunlight, regardless of whether the substance was touched or ingested. Common culprits include certain perfumes, topical nonsteroidal anti-inflammatory drugs (NSAIDs), and coal tar.
Allergic Contact Dermatitis
Allergic contact dermatitis is an immune system response to a substance in contact with the skin. Initially, the skin becomes sensitized to the substance. This sensitization can occur after a single exposure or require numerous exposures over time. Following sensitization, subsequent contact triggers an intense itching and dermatitis reaction within 4 to 24 hours, though some individuals may take 3 to 4 days to react.
Thousands of substances can lead to allergic contact dermatitis. The most common allergens are found in metals (like nickel), preservatives, plants (such as poison ivy), and rubber (including latex). Nickel sulfate is a prevalent contact allergen globally, often found in jewelry. It is not uncommon for individuals to use or be exposed to substances for years without issue, only to suddenly develop an allergic reaction. Even ointments, creams, and lotions intended to treat dermatitis can sometimes cause such a reaction.
Similar to irritant contact dermatitis, allergic contact dermatitis can also be triggered or exacerbated by sunlight exposure after contact with certain substances or ingestion. This is termed photoallergic contact dermatitis. In contrast to phototoxic reactions, photoallergic dermatitis may spread to areas not directly exposed to the sun. Typical triggers include fragrances (like musk ambrette and sandalwood), antiseptics, NSAIDs, and sunscreens.
Symptoms of Contact Dermatitis
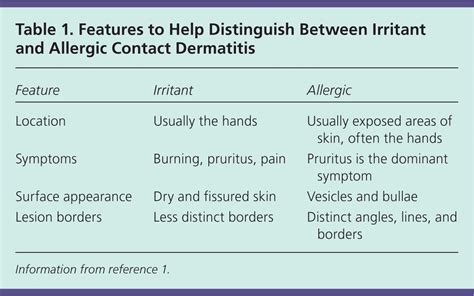
Regardless of the cause or type, contact dermatitis typically results in itching and a rash. Irritant contact dermatitis is characterized by more pain than itching, with symptoms usually subsiding within a day or two after the offending substance is removed. Allergic contact dermatitis generally causes more itching than pain, with symptoms becoming noticeable after a day or more and potentially intensifying for 2 to 3 days post-exposure.
The rash can range from mild redness to severe swelling and blistering. It primarily affects areas that came into contact with the causative substance. However, the rash may appear earlier in thin, sensitive skin areas, such as between the fingers, and later in thicker skin or areas with less contact. Hands and feet may develop small blisters. The pattern of the rash in allergic contact dermatitis can often suggest the specific substance involved; for instance, poison ivy can cause linear streaks on the skin.
It is important to note that touching the rash or blister fluid does not spread contact dermatitis to other individuals or to unaffected parts of one's own body.
Diagnosis of Contact Dermatitis
Diagnosing contact dermatitis involves a thorough evaluation by a doctor, taking into account the patient's medical history, occupation, hobbies, and exposure to various products. The location and pattern of the rash often provide crucial clues. For instance, a rash appearing under clothing or jewelry, or only in sun-exposed areas, can be indicative.
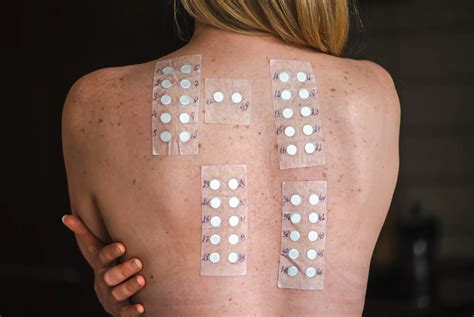
When the cause is not immediately apparent, patch testing may be employed. This procedure involves applying small patches containing standard contact allergens to the upper back. These patches remain for 48 hours, after which the skin is examined for any developing rash beneath them. Further evaluation may occur a day or two later.
Treatment of Contact Dermatitis
Effective treatment for contact dermatitis hinges on the complete avoidance of the substance causing the reaction. Once the offending agent is removed, redness typically fades over time. Blisters may continue to ooze and crust but will eventually dry. Scaling, itching, and skin thickening can persist for days or weeks.
Itching and blisters can be alleviated using topical or oral medications. For localized areas, cool compresses with gauze or thin cloth dipped in cool water or aluminum acetate solution, applied several times a day for an hour, can provide relief. Dressings that are applied wet and then dry can soothe oozing blisters, dry the skin, and promote healing.
Topical corticosteroids are frequently prescribed. Over-the-counter hydrocortisone may offer some relief, but stronger prescription corticosteroid creams might be necessary for more severe cases. In very severe instances, oral corticosteroids may be administered. Oral antihistamines like hydroxyzine and diphenhydramine can also help manage itching.
Phytophotodermatitis
Phytophotodermatitis is a specific type of reaction that occurs when a chemical from certain plants comes into contact with the skin and then reacts with sunlight. This reaction is caused by a natural chemical called furanocoumarin, found in the leaves, stems, and fruits of many plants. When sunlight activates this chemical on the skin, it can lead to irritation or burning, resulting in discoloration, swelling, and other symptoms.
Symptoms typically appear one to two days after skin contact with the plant and subsequent sun exposure. They can include a rash or small blisters, discoloration (red, purple, or darker patches), itchy or irritated skin, streaks or spots resembling drops or splashes, swelling, and mild pain. The rash is localized to the parts of the skin that touched the plant or its oils, and it can spread if the sap or juice is transferred to other body parts or clothing.
Common plants that can cause phytophotodermatitis include anise, bergamot, celery, dill, fennel, figs (especially the sap), hogweed, limes and other citrus fruits, parsley, and parsnips and carrots. Risk factors include handling fruits and vegetables, picking produce, trimming plants, and working or playing in gardens or orchards. While the rash itself is not contagious, others can develop a similar rash if they touch the same plant and are then exposed to the sun.
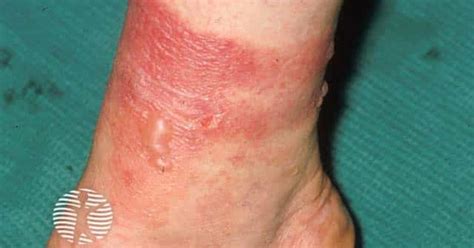
Sun Allergy (Photosensitivity Dermatitis)
Sun allergy, or photosensitivity dermatitis, is a general term encompassing conditions that cause an itchy rash after exposure to sunlight or other sources of ultraviolet (UV) radiation. Some forms are hereditary, while others are triggered by factors like medications or contact with certain plants. Mild cases may resolve independently, but severe rashes often require treatment with steroid creams or pills. Preventive measures may also be necessary for severe sun allergy.
Symptoms typically appear only on skin exposed to the sun or UV light. Causes can include immune system reactions to sunlight, certain medications, and chemicals that increase skin sensitivity to the sun. The exact reasons why some individuals develop sun allergy while others do not are not fully understood. Triggers can include contact with specific substances, taking certain medications, having other skin conditions, or having a family history of sun allergy.
Preventive measures for sun allergy include limiting sun exposure, especially during peak hours, avoiding sudden intense sun exposure, wearing protective clothing and sunglasses, and applying broad-spectrum sunscreen with an SPF of at least 30. It is also advised to avoid known triggers and consider applying UV-blocking window film.
Prognosis and Prevention
Allergic contact dermatitis may take several weeks to resolve after allergen avoidance. Irritant contact dermatitis generally resolves more quickly. Once a person develops a reaction to a substance, they typically remain sensitive to it for life. In rare cases of photoallergic contact dermatitis, flare-ups can persist for years upon sun exposure, a condition known as a persistent light reaction.
Prevention of contact dermatitis primarily involves avoiding contact with the causative substances. If accidental contact occurs, the substance should be washed off immediately with soap and water. For individuals at risk of ongoing exposure, gloves and protective clothing can be beneficial. Those with phototoxic or photoallergic contact dermatitis must avoid sun exposure. Barrier creams are also available to prevent contact with certain substances like poison ivy and epoxy resins.